Search
- Page Path
- HOME > Search
Original Article
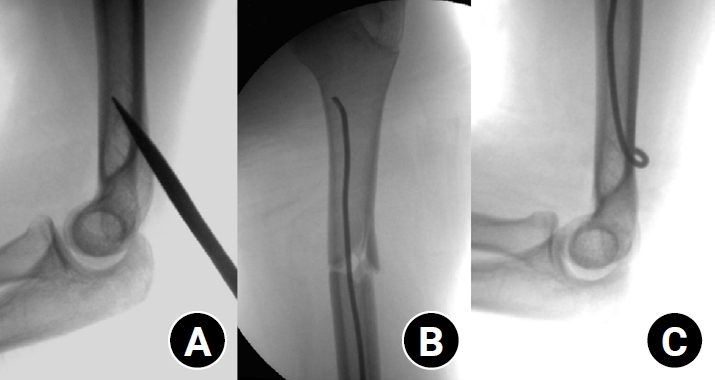
- Clinical and radiographic outcomes of elastic stable intramedullary nailing for pediatric humeral shaft fractures: a retrospective case series
- Kang-San Lee, Dongju Shin, Sang Hee Kim, Il Seo, Tae-Hoon Kim, Sung Jung Kim
- J Musculoskelet Trauma 2026;39(2):156-161. Published online March 10, 2026
- DOI: https://doi.org/10.12671/jmt.2025.00381
-
 Abstract
Abstract
 PDF
PDF - Background
Pediatric humeral shaft fractures are uncommon and are generally treated conservatively, with satisfactory clinical outcomes reported in most cases. However, conservative management often necessitates prolonged immobilization and frequent outpatient follow-up visits, and it carries an inherent risk of residual angular or translational deformity. Elastic stable intramedullary nailing (ESIN) provides a simple and minimally invasive method of fracture fixation that offers adequate stability without disrupting the periosteal blood supply, thereby permitting early mobilization and promoting rapid bone union. The purpose of this study was to evaluate the clinical and radiological outcomes of ESIN fixation in pediatric patients with humeral shaft fractures.
Methods
The medical records of pediatric patients with humeral shaft fractures who underwent ESIN fixation between January 2015 and November 2025 were retrospectively reviewed. Data collected included patient demographics, mechanism of injury, fracture location, number of elastic nails used, time to union, degree of residual angulation, range of motion (ROM), and postoperative complications.
Results
The mean age of the patients was 10.0 years (range, 7 to 15 years). The mean time to radiographic union was 5.4 weeks (range, 2.4 to 10.4 weeks). The mean coronal angulation was 0.2° (range, −9.1° to 5.8°), while the mean sagittal angulation was −1.3° (range, −6.9° to 5.3°). No cases of infection, nerve injury, or nail migration were observed during the follow-up period. At the final follow-up assessment, all patients demonstrated full shoulder and elbow ROM, with no residual deformity or pain reported.
Conclusions
In this small retrospective case series, ESIN fixation resulted in favorable union rates and excellent functional outcomes in pediatric humeral shaft fractures. Level of evidence: IV.
- 343 View
- 12 Download

Review Article
- How to obtain the desired results from distal tibial nailing based on anatomy, biomechanics, and reduction techniques
- Jungtae Ahn, Se-Lin Jeong, Gu-Hee Jung
- J Musculoskelet Trauma 2025;38(2):74-85. Published online March 31, 2025
- DOI: https://doi.org/10.12671/jmt.2025.00024

-
 Abstract
Abstract
 PDF
PDF - Distal tibial metaphyseal fractures are commonly caused by high-energy injuries in young men and osteoporosis in older women. These fractures should be clearly distinguished from high-energy pilon fractures. Although the optimal surgical intervention methods for distal tibial metaphyseal fractures remain uncertain and challenging, surgical treatments for nonarticular distal tibia fractures can be broadly divided into two types: plate fixation and intramedullary nail (IMN) fixation. Once functional reduction is achieved using an appropriate technique, distal tibial nailing might be slightly superior to plate fixation in reducing postoperative complications. Thus, the surgical strategy should focus on functional realignment and proceed in the following sequence: (1) restoring the original tibial length, regardless of whether fibular fixation is to be done; (2) making the optimal entry point through an anteroposterior (AP) projection based on the overlapping point between the fibular tip and lateral plateau margin; (3) placing Kirschner wires (Ø2.4 mm) as blocking pins (in the AP orientation for coronal control and in the mediolateral [ML] orientation for sagittal control) as close to the upper locking hole as possible without causing further comminution on the concave aspect of the short fragment; and (4) making the the distal fixation construct with at least two ML and one AP interlocking screw or two ML interlocking screws and blocking screws. After the IMN is adequately locked, blocking pins (Ø2.4 mm) need to be replaced by a 3.5 mm screw.
-
Citations
Citations to this article as recorded by- Rigid intramedullary nailing with suprapatellar approach for tibial shaft fractures in adolescents with open physes
Jong Wha Lee, Jae Ho Cho, Tae Hun Kim, Hyung Keun Song, Won-Tae Cho, Seungyeob Sakong, Hyun Il Choi, Sumin Lim
Injury.2026; 57(4): 113130. CrossRef - Impact of Foot Width on Patient-Reported Outcomes Assessed by 3-Dimensional Foot Morphometry in Hallux Valgus
Jungtae Ahn, Dae-Cheol Nam, Gu-Hee Jung
Clinics in Orthopedic Surgery.2025; 17(6): 1062. CrossRef
- Rigid intramedullary nailing with suprapatellar approach for tibial shaft fractures in adolescents with open physes
- 4,177 View
- 94 Download
- 2 Crossref

Original Articles
- Comparison of Results between Minimally Invasive Plate Fixation and Antegrade Intramedullary Nailing of Recon-Type in Low-Energy Injury Distal Femoral Shaft Fractures
- Hong Moon Sohn, Gwangchul Lee, Ba Rom Kim, Jung Soo Oh
- J Korean Fract Soc 2024;37(2):87-94. Published online April 30, 2024
- DOI: https://doi.org/10.12671/jkfs.2024.37.2.87
-
 Abstract
Abstract
 PDF
PDF - Purpose
This study compared the outcomes of minimally invasive plate osteosynthesis and antegrade intramedullary nailing for low-energy fracture of the distal femoral shaft.
Materials and Methods
A study was conducted on 30 patients who underwent surgery for low-energy fractures of the distal femoral shaft between January 2016 and April 2022. The study compared 15patients who underwent minimally invasive plate osteosynthesis (Group P) with 15 patients who underwent recon-type antegrade intramedullary nailing (Group N). We evaluated intraoperative blood loss, operative time, C-arm exposure time, bone density, final union status, anatomical reduction, and clinical evaluation. The complications were also examined, and statistical analysis was conducted to compare the two groups.
Results
The blood loss, surgery time, and C-arm time were similar in the two groups. The radiographic assessments and clinical evaluations were also similar in the two groups. The clinical results showed no difference between the groups. Group N had one case of nonunion and one case of delayed union, while Group P had one case of nonunion and one case of peri-prosthetic fracture.
Conclusion
Antegrade intramedullary nailing of the recon-type demonstrated comparable results to minimally invasive plate osteosynthesis. Hence, antegrade intramedullary nailing of the recon-type, which enhances stability by fixing the entire femur and providing additional fixation in the distal portion, is deemed appropriate for treating distal femoral shaft fractures.
- 948 View
- 18 Download

- Comparison of the Clinical and Radiological Outcomes of TFNA (Trochanteric Fixation Nail-Advanced) and PFNA-II (Proximal Femoral Nail Antirotation-II) Treatment in Elderly Patients with Intertrochanteric Fractures
- Min Sung Kwon, Young Bok Kim, Gyu Min Kong
- J Korean Fract Soc 2022;35(4):162-168. Published online October 31, 2022
- DOI: https://doi.org/10.12671/jkfs.2022.35.4.162
-
 Abstract
Abstract
 PDF
PDF - Purpose
Trochanteric fixation nail advanced (TFNA) was modified to compensate for the shortcomings of proximal femoral nail antirotation-II (PFNA-II). The clinical and radiological outcomes of surgeries us-ing the PFNA-II and TFNA for femoral intertrochanteric fractures were compared.
Materials and Methods
Eighty-two patients who underwent surgeries using PFNA-II or TFNA were analyzed. Only those who were followed up for more than a year were enrolled. Bone union, shortening of the femoral neck, and the tip–apex distance of the intramedullary nail were compared in the radiological findings. Clinical outcomes, including the frequency of complications and gait ability (Koval score), were also assessed.
Results
The mean follow-up periods were 22 and 19 months for the PFNA-II and TFNA groups, re-spectively. In the PFNA-II group, two cases of femoral head cut-out and one case of varus collapse were observed. In the TFNA group, only one case of femoral head cut-out was observed; however, there was no significant difference in the frequency of complications between the two groups (p=0.37). Ad-ditionally, both the shortening of the femoral neck and the decrease in gait ability after surgery showed relative improvement in the TFNA group compared to the PFNA-II group; however, there was no sig-nificant difference between the two groups.
Conclusion
The use of both TFNA and PFNA-II was associated with satisfactory outcomes. In patients who underwent surgeries using TFNA, the recovery of gait ability, frequency of complications, and short-ening of the femoral neck were not significantly different from PFNA-II, suggesting that both are suitable instrument choices for intertrochanteric fracture treatment. However, the clinical significance must be further assessed using a larger group of patients over a longer follow-up period in future studies. -
Citations
Citations to this article as recorded by- Treatment of Incompletely Displaced Femoral Neck Fractures Using Trochanteric Fixation Nail-Advanced in Patients Older Than 50 Years of Age
Jee Young Lee, Gyu Min Kong
Journal of Orthopaedic Trauma.2025; 39(7): 352. CrossRef - Clinical and Radiological Outcomes of Unstable Intertrochanteric Fractures Treated with Trochanteric Fixation Nail-Advanced and Proximal Femoral Nail Antirotation-II: Correlation between Lateral Sliding of the Helical Blade and Lateral Trochanteric Pain
Sung Yoon Jung, Myoung Jin Lee, Lih Wang, Hyeon Jun Kim, Dong Hoon Sung, Jun Ha Park
Journal of the Korean Orthopaedic Association.2024; 59(3): 208. CrossRef
- Treatment of Incompletely Displaced Femoral Neck Fractures Using Trochanteric Fixation Nail-Advanced in Patients Older Than 50 Years of Age
- 5,171 View
- 71 Download
- 2 Crossref

- Intra-Articular Alterations after Suprapatellar Nailing in Tibial Shaft Fractures: An Arthroscopic Evaluation
- GwangChul Lee, Sung Hun Yang, Sung Min Jo, Jeong Min Kook
- J Korean Fract Soc 2022;35(4):129-134. Published online October 31, 2022
- DOI: https://doi.org/10.12671/jkfs.2022.35.4.129
-
 Abstract
Abstract
 PDF
PDF - Purpose
This study attempted to study the intra-articular changes due to intramedullary nailing through the suprapatellar approach by evaluating the joint cartilage damage and presence of foreign bodies through a comparison of the pre- and post-operative status evaluated by knee arthroscopy.
Materials and Methods
This retrospective study analyzed fifteen patients who underwent intramedullary nailing through the suprapatellar approach for proximal tibial shaft fracture from January 2017 to March 2020. The condition of the joint cartilage and the presence of foreign substances in the patellofemoral joint were evaluated. The cartilage status of the patellofemoral joint was evaluated using the International Cartilage Repair Society (ICRS) grading system. Data from the ICRS grading and the visual analogue scale (VAS) scores of the femoral and patellar cartilage were compared to each independent variable surveyed.
Results
All the intra-articular structures before nailing were normal. In all cases after nailing, articular cartilage damage of the patellofemoral joint and intra-articular debris were observed. The average VAS score was 0.6 (0-1) before surgery and 2.27 (0-4) after surgery. There were no statistically significant differences except for the correlation in the diameter of the tibia nail and femoral ICRS grade (p=0.001) and the damage to the cartilage was greater in the femoral cartilage than that to the patella (p=0.001).
Conclusion
Intra-articular damage appears to be unavoidable in suprapatellar nailing. Further research is needed on the long-term effects of intra-articular damage and on methods to reduce this damage.
- 660 View
- 11 Download

- Assessment of Noncontiguous Posterior Malleolar Fractures in Distal One-Third Tibia Shaft Fractures with Proximal Fibula Fractures
- Dae-Geun Kim, Byung Hoon Kwack
- J Korean Fract Soc 2022;35(3):103-108. Published online July 31, 2022
- DOI: https://doi.org/10.12671/jkfs.2022.35.3.103
-
 Abstract
Abstract
 PDF
PDF - Purpose
Posterior malleolar fractures after intramedullary nail surgery rarely occur in distal tibia shaft fractures. The importance of preoperative ankle evaluation in preventing these fractures is also common knowledge. There are no studies in the literature on posterior malleolar fractures in distal onethird tibia shaft fractures except for distal metaphyseal tibia fractures to the best of our knowledge. The purpose of this study was to evaluate the incidence and radiological features of posterior malleolar fractures in distal one-third tibia shaft fractures with proximal fibula fractures.
Materials and Methods
Thirty-one patients diagnosed with distal one-third tibia shaft fractures with proximal fibula fractures from January 2016 to May 2021 were retrospectively reviewed. With the aid of plain radiographs and computed tomography (CT) scans, the fracture patterns of the tibia and fibula were classified according to the AO Foundation/Orthopedic Trauma Association (AO/OTA) classification, and posterior malleolar fractures were identified. The fracture pattern was classified according to the Haraguchi classification, and the angle between the bimalleolar axis and the posterior malleolar fracture line was measured when there was a posterior malleolar fracture.
Results
Out of the 31 distal one-third tibia shaft fractures with proximal fibula fractures, 16 cases (51.6%) had noncontiguous posterior malleolar fractures that were confirmed on a CT scan, while 3 cases (18.8%) were visible on initial plain radiographs. There was no statistically significant variation seen in the presence of a posterior malleolar fracture in the tibia (p=0.15) and fibula (p=0.87) fractures. According to the Haraguchi classification, there were 15 posterolateral-oblique fractures (Type I) and 1 medial-extension fracture (Type II), and the mean angle was 24.5°.
Conclusion
Noncontiguous posterior malleolar fractures occurred in approximately half of the distal one-third tibia shaft fractures with proximal fibula fractures, and a CT scan was considered necessary to diagnose posterior malleolar fractures before surgery
- 817 View
- 11 Download

- Minimal Invasive Fixation Methods for the Metacarpal Fracture
- Ki Youn Kwon, Jin Rok Oh, Ji Woong Kwak
- J Korean Fract Soc 2022;35(1):9-15. Published online January 31, 2022
- DOI: https://doi.org/10.12671/jkfs.2022.35.1.9
-
 Abstract
Abstract
 PDF
PDF - Purpose
This study compared the radiologic and clinical outcomes of metacarpal fractures treated with two minimally invasive surgical techniques: Kirschner wire (K-wire) fixation and headless screw fixation.
Materials and Methods
This study included 52 patients (46 males and 6 females; age 18-55 years) with distal metacarpal fractures (middle and distal shaft, including the neck) who had undergone K-wire fixation or headless screw fixation. All subjects were followed up for at least six months. The radiologic assessments were performed to evaluate the angular deformity and shortenings. The total active motion (TAM), grip strength, and patients’ subjective functional assessment were measured to evaluate the hand function. The time taken to return to work (RTW) and adverse events were analyzed.
Results
Of the 52 cases, metacarpal fractures treated with headless screw fixation and K-wire fixation showed a significant difference associated with early RTW (p<0.05). There were no significant differences between the subjects treated with K-wire fixation and those with headless screw fixation in terms of the radiologic measurement, hand function examinations, complications, and adverse events (p>0.05).
Conclusion
After a six-month follow-up, minimally invasive K-wire fixation and headless screw fixation produced similar clinical and radiologic outcomes in subjects with metacarpal fractures. Compared to K-wire fixation, however, headless screw fixation led to earlier functional recovery and might be a better option for treating metacarpal fractures in this regard.
- 721 View
- 5 Download

- Comparison of the Results between Plating and Intramedullary Nailing for Ipsilateral Fibular Fractures in Pilon Fractures
- Yong Jin Cho, Jun Young Lee, Jae Hwan Lim, Je Hong Ryu, Jung Ho Lee
- J Korean Fract Soc 2021;34(3):97-104. Published online July 31, 2021
- DOI: https://doi.org/10.12671/jkfs.2021.34.3.97
-
 Abstract
Abstract
 PDF
PDF - Purpose
To compare the results between plating and intramedullary nailing for ipsilateral fibular fractures in pilon fractures.
Materials and Methods
Among 124 patients with pilon fractures from November 2008 to March 2019, 50 patients with a fibular fracture were studied retrospectively and divided into two groups: Group A using a plate and Group B using a Rush pin. The radiological tests confirmed the fracture pat-terns (Rüedi–Allgöwer classification, AO/OTA classification) and evaluated the degree of reduction of fibular and tibial fractures after surgery. The American Orthopaedic Foot & Ankle Society (AOFAS) was examined for a clinical evaluation, and the complications were checked.
Results
The two groups showed similar distributions in gender, age, injury mechanism, diabetes, smoking, mean follow-up period, Rüedi–Allgöwer classification, AO/OTA classification, and open fracture. The fibular fractures were classified as simple, wedge, multiple, and segmental, showing significant differences between the two groups (p=0.03). There was no difference in the Talocrural angle, Shenton line, and Dime sign. In the reduction of pilon fractures, the appropriate reduction was obtained in 22 cases (88.0%) for both groups. The AOFAS averaged 83.24 in Group A and 80.44 points in Group B, showing no significant difference in complications (nonunion, malunion, infection, and arthritis).
Conclusion
Regardless of how the fibular fracture was fixed, the reduction of pilon fractures in both groups showed good results. Both intramedullary nail and plate fixation could be a suitable fixation method for ipsilateral fibular fractures with a low risk of shortening in pilon fractures.
- 653 View
- 3 Download

- Results of Intramedullary Nailing for Distal Metaphyseal Intra-Articular Fractures of Tibia
- Jun Young Lee, Yongjin Cho, Hyung Seok Park, Se Woong Jang
- J Korean Fract Soc 2020;33(4):196-203. Published online October 31, 2020
- DOI: https://doi.org/10.12671/jkfs.2020.33.4.196
-
 Abstract
Abstract
 PDF
PDF - Purpose
This study examined the results of internal fixation using an intramedullary nail in the treatment of distal metaphyseal fractures involving the articular surface.
Materials and Methods
From November 2009 to November 2018, distal tibia fractures involving the articular surface were treated with intramedullary nailing only for fractures corresponding to AO type 43 B and 43 C1, twenty-four cases were studied retrospectively. The tibial alignment was measured preoperatively and postoperatively, and the bone union time and nonunion were assessed. In addition, the clinical evaluation of ankle joint function was assessed using the Olerud and Molander ankle score (OMAS).
Results
Complete bone union was obtained in all cases, and the mean union time was 17.7±1.87 weeks (range, 15-20 weeks). The average preoperative coronal alignment was 6.4°±1.0° (range, 5.2°-8.4°), and sagittal alignment was 2.7°±0.6° (range, 1.9°-3.8°). The average postoperative coronal alignment was 2.5°±0.13° (range, 2.2°-2.6°) and sagittal alignment was 0.4°±0.25° (range, 0.09°-0.95°). There was no nonunion. The OMAS had an average of 85±7.9 points (range, 70-95 points).
Conclusion
In the treatment of distal metaphyseal fractures involving the articular surface, internal fixation using an intramedullary nail reduces complications and achieves satisfactory reduction and union. This method is considered an excellent treatment to obtain good clinical results.
- 727 View
- 6 Download

Case Report
- Rare Experience of Bilateral Femoral Neck and Shaft Fractures - A Case Report -
- DaeHyun Choe, Jae-Ho Lee, Ki-Chul Park
- J Korean Fract Soc 2020;33(3):154-158. Published online July 31, 2020
- DOI: https://doi.org/10.12671/jkfs.2020.33.3.154
-
 Abstract
Abstract
 PDF
PDF - Ipsilateral fractures of the femoral neck and shaft are relatively common injuries and accompany 2% to 9% of all femoral shaft fractures. On the other hand, it is extremely rare for these injuries to occur bilaterally. This paper reports the authors’ experience of a case with bilateral femoral neck and shaft fractures. The patient sustained multiple injuries, including liver laceration with hemoperitoneum, bilateral open fractures of the tibia, and bilateral femoral neck, and shaft fractures caused by a high-speed motor vehicle accident. Under the circumstances, damage-control orthopedic principles were applied, and external fixators were initially placed. After the patient’s general condition showed improvement, both femurs were fixed with a reconstruction nail. Fracture healing was achieved without complications, such as avascular necrosis of the femoral head. Despite the rare occurrence, this paper describes this case because these injuries must be managed with meticulous attention.
- 719 View
- 8 Download

Original Articles
- Clinical Outcome after Treatment of Tibia Segmental Fracture with Intramedullary Nailing and Minimal Invasive Plate Osteosynthesis
- Jun Young Lee, Hyung Seok Park, Dong Hyuk Cha
- J Korean Fract Soc 2020;33(3):142-147. Published online July 31, 2020
- DOI: https://doi.org/10.12671/jkfs.2020.33.3.142
-
 Abstract
Abstract
 PDF
PDF - Purpose
This study examined the clinical outcomes after the treatment of a tibia segmental fracture with intramedullary nailing (IM nailing) and minimal invasive plate osteosynthesis (MIPO).
Materials and Methods
From July 2012 to December 2017, 14 out of 17 cases from a treatment cohort of 32 cases of AO type 42 C2 tibia segmental fractures with IM nailing and MIPO were studied retrospectively. Periodic radiographs were used to evaluate the presence of union, union time, and radiographic evaluation of bony union (varus-valgus deformity, anteroposterior angular deformity, shortening). To evaluate the postoperative clinical function, modified Rasmussen’s system was used for proximal fractures, and the American Orthopaedic Foot and Ankle Society functional score was used for distal fractures.
Results
Bony union was achieved in all 14 cases, and the average union time was 26 weeks. In one case of soil contamination, there were no other complications other than simple debridement after a soft tissue infection. The mean varus was two degrees; the mean anteroposterior angular deformity was three degrees of anterior oblique; the mean length shortening was 5 mm (2-9 mm). The mean functional score of the knee joint with the Modified Rasmussen’s system measured for the postoperative clinical function was relatively good (excellent 9, good 4, fair 1, and poor 0). The results of the Molander and Olerud Functional scores of the ankle joints were also good (excellent 8, good 3, fair 2, poor 0).
Conclusion
The treatment of tibia segmental fractures with IM nailing and MIPO can effectively reduce the gap of fracture sites. Hence, it is possible to increase the bony union probability and obtain relatively satisfactory alignment. Overall, the treatment of tibia segmental fractures with IM nailing and minimally invasive plate osteosynthesis appears to be a useful treatment, considering the preservation of the soft tissue and the alignment of the tibia.
- 866 View
- 7 Download

- Three-Dimensional Analysis of the Morphological Features in the Femur of Atypical Fracture and Practical Implications of Intramedullary Nailing
- Yong Uk Kwon, Kyung-Jae Lee, Joo Young Choi, Gu-Hee Jung
- J Korean Fract Soc 2020;33(2):87-95. Published online April 30, 2020
- DOI: https://doi.org/10.12671/jkfs.2020.33.2.87
-
 Abstract
Abstract
 PDF
PDF - Purpose
This study analyzed the morphological features of the contralateral femur without an atypical fracture by constructing a three-dimensional model with an actual size medullary canal.
Materials and Methods
Lateral and anterior bowing of the shaft were measured for 21 models, and the shape of the medullary canal was analyzed. To eliminate the projection error, the anteroposterior (AP) femur was rotated internally to the extent that the centerline of the head and neck, which is the ideal position of cephalomedullary nail screw, was neutral, and the lateral femur matched the medial and lateral condyle exactly.
Results
The lateral bowing and anterior bowing was an average of 5.5° (range, 2.8°-10.7°; standard deviation [SD], 2.4°) and 13.1° (range, 6.2°-21.4°; SD, 3.2°), respectively. In the area where lateral bowing increased, the lateral cortex became thicker, and the medullary canal was straightened. On the lateral femur, the anterior angle was increased significantly, and the diameter of curvature averaged 1,370.2 mm (range, 896-1,996 mm; SD, 249.5 mm).
Conclusion
Even if the anterolateral bowing increases in the atypical femur, the medullary canal tends to be straightened in the AP direction. So, it might be considered as a reference to the modification of an intramedullary nail to increase the conformity.
- 666 View
- 6 Download

- Analysis of the Changes in Femoral Varus Bowing and the Factors Affecting Nonunion for the Treatment of Femoral Shaft Fractures over 60 Years Old Using Piriformis Fossa Insertion Intramedullary Nailing
- Yonghan Cha, Chan Ho Park, Jun-Il Yoo, Jung-Taek Kim, WooSuk Kim, Ha-Yong Kim, Won-Sik Choy
- J Korean Fract Soc 2020;33(2):65-71. Published online April 30, 2020
- DOI: https://doi.org/10.12671/jkfs.2020.33.2.65
-
 Abstract
Abstract
 PDF
PDF - Purpose
This study examined the bony morphological changes to analyze the factors affecting bony union in the treatment of elderly femoral shaft fractures with varus bowing using piriformis fossa insertion intramedullary nailing.
Materials and Methods
This study included 26 patients over 60 years of age, who were admitted for femoral shaft fractures between January 2005 and December 2014 and treated with piriformis fossa insertion intramedullary nailing. Age, sex, height, weight, bone mineral density, injury mechanism, fracture type, diameter and length of the nail, postoperative lengthening of the femur, postoperative change in varus angle, contact between the lateral and anterior cortex, and the gap between the fracture line and the bony union were checked. The patients were divided into a varus group and nonvarus group, as well as a bone union group and nonunion group. Logistic regression analysis was performed to analyze the factors affecting nonunion.
Results
The patients were classified into 11 in the varus group and 15 in the non-varus group and 24 in the union group and 2 in the nonunion group. The varus group showed a larger increase in leg length and varus angle reduction than the non-varus group (p<0.05). The union group had more contact with the lateral cortical bone than that of the nonunion group (p<0.05). The factor affecting bone union in regression analysis was contact of the lateral cortical bone (p<0.05).
Conclusion
Treatment of a femoral shaft fracture in elderly patients with a varus deformity of the femur using piriformis fossa insertion intramedullary nail increases the length of the femur and decreases the varus deformity. For bony union, the most important thing during surgery is contact of the lateral cortical bone with the fracture site. -
Citations
Citations to this article as recorded by- Straight nail insertion through a laterally shifted entry for diaphyseal atypical femoral fractures with bowing: good indications and limitations of this technique
Seong-Eun Byun, Young-Ho Cho, Young-Kyun Lee, Jung-Wee Park, Seonguk Kim, Kyung-Hoi Koo, Young Soo Byun
International Orthopaedics.2021; 45(12): 3223. CrossRef
- Straight nail insertion through a laterally shifted entry for diaphyseal atypical femoral fractures with bowing: good indications and limitations of this technique
- 1,439 View
- 9 Download
- 1 Crossref

- Results of Exchange Nailing in Hypertrophic Nonunion of Femoral Shaft Fracture Treated with Nailing
- Suenghwan Jo, Gwang Chul Lee, Sang Hong Lee, Jun Young Lee, Dong Hwi Kim, Sung Hae Park, Young Min Cho
- J Korean Fract Soc 2019;32(2):83-88. Published online April 30, 2019
- DOI: https://doi.org/10.12671/jkfs.2019.32.2.83
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
This study examined the outcomes of exchange nailing for the hypertrophic nonunion of femoral shaft fractures treated with intramedullary nailing as well as the factors affecting the treatment outcomes.
MATERIALS AND METHODS
From January 1999 to March 2015, 35 patients, who had undergone intramedullary nailing with a femoral shaft fracture and underwent exchange nailing due to hypertrophic nonunion, were reviewed. This study investigated the time of union and complications, such as nonunion after exchange nailing, and analyzed the factors affecting the results.
RESULTS
Bone union was achieved in 31 cases (88.6%) after exchange nailing and the average bone union period was 22 weeks (14–44 weeks). Complications included persistent nonunion in four cases, delayed union in one case, and superficial wound infection in one case. All four cases with nonunion were related to smoking, three of them were distal shaft fractures, and one was a midshaft fracture with underlying disease.
CONCLUSION
Exchange nailing produced satisfactory results as the treatment of hypertrophic nonunion after intramedullary nailing. Smoking is considered a factor for continuing nonunion even after exchange nailing. In the case of a distal shaft, where the intramedullary fixation is relatively weak, additional efforts are needed for stability.
- 1,186 View
- 13 Download

Case Report
- Subtrochanteric Fracture Reduction during Intramedullary Nailing: Technical Note
- Gyu Min Kong
- J Korean Fract Soc 2019;32(2):107-111. Published online April 30, 2019
- DOI: https://doi.org/10.12671/jkfs.2019.32.2.107
-
 Abstract
Abstract
 PDF
PDF - The subtrochanteric area is the place where mechanical stress is most concentrated in the femur. When a fracture happens, bone union is delayed and nonunion often occurs. The recommended treatment for atypical fractures is an anatomical reduction of the fracture site as the frequency of nonunion is higher than that of ordinary fractures. Various reduction methods have been suggested, and good results have been obtained. On the other hand, the occurrence of posterior displacement of the distal fragment during the insertion of an intramedullary nail is often overlooked. This is probably because the bone marrow of the femur tends to form an elliptical shape in the anteroposterior direction. The author attempted to insert a blocking screw into the distal part of the fracture to prevent posterior displacement of the distal fragment while performing intramedullary nailing of the femur fracture and achieved a good reduction state easily.
- 956 View
- 12 Download

Original Article
- Treatment of the Proximal Femoral Fracture Using the New Design Cephalomedullary Nail: Prospective Outcomes Study
- Young Ho Roh, Joseph Rho, Kwang Woo Nam
- J Korean Fract Soc 2019;32(1):35-42. Published online January 31, 2019
- DOI: https://doi.org/10.12671/jkfs.2019.32.1.35
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
The aim of this study is to investigate the clinical performance and safety of Zimmer® natural nail cephalomedullary nail (ZNN CM nail) in the treatment of proximal femur fractures.
MATERIALS AND METHODS
The following research was conducted as a prospective, non-comparative, single center outcome study. Upon providing written informed consent, enrolled patients' data were collected and analyzed. Postoperative follow-up visits were scheduled at 6 weeks, 3 months, 6 months, and 1 year. Follow-up evaluation included radiographic assessment, physical examination, and quality of life and adverse events reports.
RESULTS
Thirty-nine patients were available for evaluation at one year postoperative. The patients reported the mean EuroQol-5 Dimension score increased after surgery: from 0.4 points at discharge (n=49) to 0.6 points at 1-year post-surgery (n=39). The mean Harris hip score also increased after surgery: from 56.3 points at discharge (n=49) to 72.1 points at 1 year (n=12). Bone union was seen in 64% (n=16) in 6 months and 95% (n=37) in 1 year.
CONCLUSION
The results of this 1-year follow-up study affirmed the effectiveness and safety of the ZNN CM nail in the treatment of proximal femur fractures. -
Citations
Citations to this article as recorded by- Clinical and Radiologic Outcome of Intertrochanteric Fracture Treatment Using TFNA (Trochanteric Fixation Nail-Advanced)
Hyeon Joon Lee, Hyun Bai Choi, Ba Rom Kim, Seung Hwan Jo, Sang Hong Lee
Journal of the Korean Fracture Society.2021; 34(3): 105. CrossRef - Treatment of Proximal Femur Fracture with a Newly Designed Nail: Trochanteric Fixation Nail-Advanced (TFNA)
Jae Youn Yoon, Ji Wan Kim
Journal of the Korean Fracture Society.2020; 33(4): 189. CrossRef
- Clinical and Radiologic Outcome of Intertrochanteric Fracture Treatment Using TFNA (Trochanteric Fixation Nail-Advanced)
- 1,250 View
- 0 Download
- 2 Crossref

Review Article
- Atypical Femoral Fractures: What Do We Know about Them?
- Beom Seok Lee, Young Kyun Lee, Heejae Won, Hyungkook Kim, Kyung Hoi Koo
- J Korean Fract Soc 2018;31(4):159-164. Published online October 31, 2018
- DOI: https://doi.org/10.12671/jkfs.2018.31.4.159
-
 Abstract
Abstract
 PDF
PDF - Recently, atypical femoral fractures (AFFs) have been found in patients who were prescribed bisphosphonate to prevent osteoporotic fractures. Although the occurrence of AFF is rare, there are some concerns, such as a higher risk of delayed or non-union of AFF. This paper reviews the treatment of AFF and suggests some considerations during surgery.
-
Citations
Citations to this article as recorded by- How to Improve Fracture Healing in Atypical Femoral Fractures
Sang-Jin Jeong, Chan-Woo Park, Seung-Jae Lim
Journal of the Korean Orthopaedic Association.2024; 59(1): 9. CrossRef - Atypical Femoral Fracture Occurring at a Proximal Screw Insertion Site after Plate Removal in a Distal Femoral Fracture
Jin Woo Jin, Sung Jin Shin, Jong Min Jeon
Journal of the Korean Orthopaedic Association.2024; 59(4): 314. CrossRef - Position Statement: Atypical Femoral Fracture from the Korean Society for Bone and Mineral Research in 2023
Jae-Hwi Nho, Byung-Woong Jang, Dong Woo Lee, Jae-Hyun Kim, Tae Kang Lim, Soo Min Cha, Dong-Kyo Seo, Yong-Geun Park, Dong-Geun Kang, Young-Kyun Lee, Yong-Chan Ha
Journal of Bone Metabolism.2023; 30(3): 209. CrossRef
- How to Improve Fracture Healing in Atypical Femoral Fractures
- 809 View
- 7 Download
- 3 Crossref

Original Articles
- Comparative Analysis of Minimally Invasive Plate Osteosynthesis and Intramedullary Nailing in the Treatment of the Distal Tibia Fractures
- Ho Min Lee, Young Sung Kim, Jong Pil Kim, Phil Hyun Chung, Suk Kang, Kaung Suk Jo
- J Korean Fract Soc 2018;31(3):94-101. Published online July 31, 2018
- DOI: https://doi.org/10.12671/jkfs.2018.31.3.94
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
This study compared the radiological and clinical results of minimally invasive plate osteosynthesis (MIPO) and intramedullary nailing (IMN) of distal tibial fractures, which were classified as the simple intra-articular group and extra-articular group.
MATERIALS AND METHODS
Fifty patients with distal tibial fractures, who could be followed-up more than 12 months, were evaluated. Group A consisted of 19 patients treated with MIPO and group B consisted of 31 patients treated with IMN. The results of each group were analyzed by radiological and clinical assessments.
RESULTS
The mean operation times in groups A and B were 72.4 minutes and 65.7 minutes, respectively. The mean bone union times in groups A and B were 16.4 weeks and 15.7 weeks, respectively. The bone union rate in groups A and B were 100% and 93%, respectively. The ranges of ankle motion were similar in the two groups at the last follow-up. The mean American Orthopaedic Foot and Ankle Society score was similar: 90.1 in group A and 90.5 in group B. The radiological and clinical results were similar in the intra and extra-articular groups. In groups A and B, two cases of posterior angulation and five cases of valgus deformity of more than 5° were encountered.
CONCLUSION
Both MIPO and IMN achieved satisfactory results in extra-articular AO type A and simple articular extension type C1 and C2 distal tibia fractures. -
Citations
Citations to this article as recorded by- Intramedullary Nailing versus Minimally Invasive Plate Osteosynthesis for Distal Tibia Shaft Fractures: Retrospective Comparison of Functional and Cosmetic Outcomes
Kahyun Kim, In Hee Kim, Geon Jung Kim, SungJoon Lim, Ji Young Yoon, Jong Won Kim, Yong Min Kim
Journal of Korean Foot and Ankle Society.2023; 27(3): 93. CrossRef
- Intramedullary Nailing versus Minimally Invasive Plate Osteosynthesis for Distal Tibia Shaft Fractures: Retrospective Comparison of Functional and Cosmetic Outcomes
- 714 View
- 2 Download
- 1 Crossref

- The Effects of Extramedullary Reduction in Unstable Intertrochanteric Fracture: A Biomechanical Study Using Cadaver Bone
- Young Chang Park, Soon Phil Yoon, Kyu Hyun Yang
- J Korean Fract Soc 2018;31(3):79-86. Published online July 31, 2018
- DOI: https://doi.org/10.12671/jkfs.2018.31.3.79
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To prevent excessive sliding and subsequent fixation failures in unstable intertrochanteric fractures with posteromedial comminution, extramedullary reduction through overlapping of the anteromedial cortices of both proximal and distal fragments as a buttress has been introduced. The purpose of this study was to compare the biomechanical properties between two reduction methods-intramedullary reduction and extramedullary reduction-in treating unstable intertrochanteric fractures with posteromedial comminution (AO/OTA classification 31-A2.2).
MATERIALS AND METHODS
Eight pairs of frozen human cadaveric femora were used. The femora of each pair were randomly assigned to one of two groups: the intramedullary reduction group or the extramedullary reduction group. A single axial load-destruction test was conducted after cephalomedullary nailing. Axial stiffness, maximum load to failure, and energy absorbed to failure were compared between the two groups. Moreover, the pattern of mechanical failure was identified.
RESULTS
The mean axial stiffness in the extramedullary reduction group was 27.3% higher than that in the intramedullary reduction group (422.7 N/mm vs. 332.0 N/mm, p=0.017). Additionally, compared with the intramedullary reduction group, the mean maximum load to failure and mean energy absorbed to failure in the extramedullary group were 44.9% and 89.6% higher, respectively (2,848.7 N vs. 1,966.5 N, p=0.012 and 27,969.9 N·mm vs. 14,751.0 N·mm, p=0.012, respectively). In the intramedullary reduction group, the mechanical failure patterns were all sliding and varus deformities. In the extramedullary reduction group, sliding and varus deformities after external rotation were noted in 3 specimens, sliding and varus deformities after internal rotation were noted in 3 specimens, and medial slippage was noted in 2 specimens.
CONCLUSION
In unstable intertrochanteric fractures with posteromedial comminution, the biomechanical properties of extramedullary reduction are superior to those of intramedullary reduction. Anteromedial cortex could be the proper buttress, despite a comminuted posteromedial cortex. It could help enhance the stability of the bone-nail construct. -
Citations
Citations to this article as recorded by- The effect of additional reduction screw fixation for basicervical femoral neck fracture: a finite element analysis
Kyoung-Joo Lee, Jihoon Ahn, Chul-Ho Kim
HIP International.2026; 36(2): 324. CrossRef - Comparison of the Dynamic Cut‐Out Failure Modes of Common Proximal Femoral Fixation Devices Using a Mesh‐Free Computational Method
Erica Ueda Boles, Sloan Kulper, Katie Whiffin, Marilyn Janice Oentaryo, Kerstin Schneider, Frankie Leung, Christian X. Fang
Journal of Orthopaedic Research.2026;[Epub] CrossRef - Cortical Support in Unstable Intertrochanteric Fracture without Fixation of Posteromedial Fragment
Ki-Tae Park, Dong-Hoon Lee, Kyung-Hoi Koo, Jung-Wee Park, Young-Kyun Lee
Clinics in Orthopedic Surgery.2026;[Epub] CrossRef - Which side should be taken care of when positioning a lag screw in intertrochanteric femoral fracture: right or left?
Min Uk Do, Kyeong Baek Kim, Sang-Min Lee, Hyun Tae Koo, Won Chul Shin
European Journal of Trauma and Emergency Surgery.2025;[Epub] CrossRef - Distal locking mechanism influences surgical and radiological outcomes in proximal femoral nailing using distal wedge versus distal screw designs
Aytek Hüseyin Çeliksöz, Büşra Tokmak, Ali Okan Tarlacık, Servet Igrek
Scientific Reports.2025;[Epub] CrossRef - The effect of anterior support screw (AS2) in unstable femoral trochanteric fractures: A multicenter randomized controlled trial
Takashi Maehara, Takashi Hayakawa, Shunsuke Mukoyama, Yoshihisa Anraku, Takahiro Hamada, Hiroyuki Suzuki, Takeshi Doi, Tomohiko Shimizu, Masanori Yorimitsu, Hidefumi Teramoto, Takao Mae, Yasunori Okamoto, Jun Hara, Kazushi Mihara, Koichi Kanekasu
Injury.2024; 55(10): 111725. CrossRef - Anteromedial cortical support reduction of intertrochanteric fractures–A review
Wenjun Xie, Liu Shi, Cheng Zhang, Xueliang Cui, Xiangxu Chen, Tian Xie, Sheng Zhang, Hui Chen, Yunfeng Rui
Injury.2024; 55(12): 111926. CrossRef - Anteromedial Cortical Support in Reduction of Trochanteric Hip Fractures
Wei Mao, Chen-Dong Liu, Shi-Min Chang, Ao-Lei Yang, Choon Chiet Hong
Journal of Bone and Joint Surgery.2024; 106(11): 1008. CrossRef - Five states of reduction in OTA/AO A1.3 intertrochanteric fractures of the femur a biomechanical study
Shu Li, Yong-Gang Bao, Rong-Hua Tian, Chun-Yang Meng, Hai-Bin Wang, Bin Wu, Xian-Min Bu
BMC Musculoskeletal Disorders.2024;[Epub] CrossRef - Intramedullary Impaction of the Basicervical Component Is Determinant of Fixation Failure in a Simple Two-Part Pertrochanteric Fracture
Seok Ha Hong, Kang Hun Yu, Seung Beom Han
Journal of Orthopaedic Trauma.2024; 38(4): 220. CrossRef - Flexible reamer use to overcome entry point errors in proximal femoral nail application in severe obese intertrochanteric fracture patients
Levent Horoz, Ali Ihsan Kilic, Cihan Kircil, Mehmet Fevzi Cakmak
BMC Musculoskeletal Disorders.2024;[Epub] CrossRef - Risk Factors Associated with Fixation Failure in Intertrochanteric Fracture Treated with Cephalomedullary Nail
Hyung-Gon Ryu, Dae Won Shin, Beom Su Han, Sang-Min Kim
Hip & Pelvis.2023; 35(3): 193. CrossRef - Positive or negative anteromedial cortical support of unstable pertrochanteric femoral fractures: A finite element analysis study
Qin Shao, Yue Zhang, Gui-Xin Sun, Chen-Song Yang, Na Liu, Da-Wei Chen, Biao Cheng
Biomedicine & Pharmacotherapy.2021; 138: 111473. CrossRef - Clinical and Radiologic Outcome of Intertrochanteric Fracture Treatment Using TFNA (Trochanteric Fixation Nail-Advanced)
Hyeon Joon Lee, Hyun Bai Choi, Ba Rom Kim, Seung Hwan Jo, Sang Hong Lee
Journal of the Korean Fracture Society.2021; 34(3): 105. CrossRef - Factors Associated with Mechanical Complications in Intertrochanteric Fracture Treated with Proximal Femoral Nail Antirotation
Oog-Jin Shon, Chang Hyun Choi, Chan Ho Park
Hip & Pelvis.2021; 33(3): 154. CrossRef - Additional Reduction Screw Fixation Technique for Pertrochanteric Hip Fractures: A Novel Method to Prevent Excessive Sliding in Cephalomedullary Nail Surgery
Chul-Ho Kim, Han Soul Kim, Dou Hyun Moon
Hip & Pelvis.2021; 33(3): 162. CrossRef - Comparison of sliding distance of lag screw and nonunion rate according to anteromedial cortical support in intertrochanteric fracture fixation: A systematic review and meta-analysis
Eic Ju Lim, Seungyeob Sakong, Whee Sung Son, Jae-Woo Cho, Jong-Keon Oh, Chul-Ho Kim
Injury.2021; 52(10): 2787. CrossRef - A new fluoroscopic view for evaluation of anteromedial cortex reduction quality during cephalomedullary nailing for intertrochanteric femur fractures: the 30° oblique tangential projection
Shi-Yi Chen, Shi-Min Chang, Rujan Tuladhar, Zhen Wei, Wen-Feng Xiong, Sun-Jun Hu, Shou-Chao Du
BMC Musculoskeletal Disorders.2020;[Epub] CrossRef - New Approach in the Treatment of Intertrochanteric Fracture Using a Cephalomedullary Nail
Junyoung Kim, Kihong Choi, Kyu Hyun Yang
Journal of the Korean Orthopaedic Association.2020; 55(3): 193. CrossRef - Effect of a synthetic osteoconductive bone graft substitute with zeta potential control (geneX®ds) in the treatment of intertrochanteric fracture: A single center experience of 115 consecutive proximal femoral nail antirotations
Won Chul Shin, Jae Hoon Jang, Jae Yoon Jeong, Kuen Tak Suh, Nam Hoon Moon
Journal of Orthopaedic Science.2019; 24(5): 842. CrossRef
- The effect of additional reduction screw fixation for basicervical femoral neck fracture: a finite element analysis
- 842 View
- 5 Download
- 20 Crossref

- Factors Affecting Posterior Angulation in Retrograde Intramedullary Nailing for Distal Femoral Fractures
- Hohyoung Lee, Ji Ho Jeong, Min Su Kim, Bum Soo Kim
- J Korean Fract Soc 2018;31(2):50-56. Published online April 30, 2018
- DOI: https://doi.org/10.12671/jkfs.2018.31.2.50
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To analyze the factors that cause a posterior angulatory deformity in the retrograde intramedullary nailing of distal femoral fractures.
MATERIALS AND METHODS
Fifty-five patients with distal femur fractures who were treated with retrograde intramedullary nailing were enrolled in this study. They were followed-up for at least one year postoperatively. The posterior angulatory deformity was evaluated according to the fracture location, pattern, and insertion point and the insertion point was compared with the ideal point derived from the radiographs of 100 normal adults. The correlation between the posterior angulation and the entry point of the nail was analyzed.
RESULTS
The posterior angulation was similar in terms of the fracture location; a meaningful difference was noted among the fracture patterns (p=0.047). The posterior angulation was significantly greater when the entry point was located more posteriorly, accepting a malreduced state (p=0.012).
CONCLUSION
Posterior angulation was smaller in the transverse fracture and the posterior location of the entry point from the apex of the Blumensaat's line increased the posterior angulation.
- 541 View
- 8 Download

Case Report
- Delayed Sciatic Nerve Palsy due to Hematoma Related with Anticoagulants Prophylaxis in the Femur Intramedullary Nailing: A Case Report
- Young Mo Kim, Yong Bum Joo, Seok Hwan Song
- J Korean Fract Soc 2017;30(4):198-202. Published online October 31, 2017
- DOI: https://doi.org/10.12671/jkfs.2017.30.4.198
-
 Abstract
Abstract
 PDF
PDF - Femur intramedullary nailing can be one of the most predictable procedures in orthopedic traumatology. The advantage of this method is that the fracture site does not have to be widely exposed for reduction, which can minimize soft tissue damage. For this reason, the incidence of complications related to hematoma has been rare. We experienced only one case of sciatic nerve palsy due to hematoma after intramedullary nailing; the patient was receiving an anticoagulant therapy. Therefore, we report this case with literature review.
-
Citations
Citations to this article as recorded by- Ipsilateral Foot Drop After Leg Traction on Fracture Table for Mid-Shaft Femur Fracture Nailing: A Rare Case Report
Jehad A Alzahrani, Ahmed A Alabdali, Mohammed O Albariqi
Cureus.2023;[Epub] CrossRef
- Ipsilateral Foot Drop After Leg Traction on Fracture Table for Mid-Shaft Femur Fracture Nailing: A Rare Case Report
- 1,164 View
- 8 Download
- 1 Crossref

Original Article
- Radiologic Assessment of Postoperative Stability in Unstable Intertrochanteric Fracture Using Lateral Radiograph
- Suc Hyun Kweon, Jin Yeong Park, Seng Hwan Kook, Byung Min Yoo
- J Korean Fract Soc 2016;29(3):171-177. Published online July 31, 2016
- DOI: https://doi.org/10.12671/jkfs.2016.29.3.171
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
The purpose of this study was to compare the sliding distance of lag screw in patients with unstable femoral intertrochanteric fractures treated with intramedullary fixation using a cephalomedullary nail with a fixed angle between the neck and shaft of the femur in relation to reduction type by lateral radiographs.
MATERIALS AND METHODS
Between January 2009 to October 2013, 86 cases (86 patients) with unstable femoral intertrochanteric fractures were treated with intramedullary fixation using a metal nail with a fixed neck-shaft angle and followed for at least 6 months. We used AO/OTA classification, and all cases were unstable fractures. Twenty cases were 31-A22, 54 cases were 31-A23, and 12 cases were 31-A3. There were 30 men and 56 women. Average patient age was 73.7 years (range, 47-97 years). We classified reduction types into three groups as postoperative lateral radiologic findings. Group 1 showed no displacement, group 2 showed anterior displacement of the femur neck, and group 3 showed posterior displacement of the femur neck. The radiological assessment compared the sliding distance of the lag screw between postoperative X-ray and last follow-up X-ray.
RESULTS
Forty-two cases were in group 1, 22 cases were in group 2, and the other 22 cases were in group 3. There was no significant difference in the patient characteristics of each group. The sliding distances of the lag screw were 4.9±3.2 mm, 4.6±3.6 mm, and 8.5±4.9 mm, respectively, and group 3 showed a significant result (p<0.0001, p=0.024).
CONCLUSION
In cases treated with intramedullary fixation using a cephalomedullary nail with a fixed neck-shaft angle, appropriate reduction with a lateral radiograph before screw fixation is needed to prevent excessive lag screw sliding.
- 642 View
- 6 Download

Case Report
- Iatrogenic Humeral Fracture during Reduction of Shoulder Dislocation: Two Cases Report
- Hyung Lae Cho, Hyoung Min Kim, Ki Bong Park, Tae Hyun Wang, Dong Hyun Lee
- J Korean Fract Soc 2016;29(1):50-54. Published online January 31, 2016
- DOI: https://doi.org/10.12671/jkfs.2016.29.1.50
-
 Abstract
Abstract
 PDF
PDF - Shoulder dislocation is the most common dislocation presenting to the emergency department. In old age, the attempt of closed reduction is made with caution in order to prevent iatrogenic fracture around the shoulder. We report two cases of iatrogenic fractures of humeral shaft and anatomical neck in female patients older than 70 years old, which occurred during the manual closed reduction. One patient was proved as first-time and the other was recurrent. In addition, the second case had a massive irreparable rotator cuff tear. Those patients were treated successfully with humeral nailing and reverse total shoulder arthroplasty, respectively.
- 586 View
- 9 Download

Original Articles
- Operative Treatment of Pediatric Distal Forearm Bothbone Fracture
- Sang Uk Lee, Changhoon Jeong, Il Jung Park, Jaeyoung Lee, Seman Oh, Kyung Hoon Lee, Sanghyun Jeon
- J Korean Fract Soc 2015;28(4):237-244. Published online October 31, 2015
- DOI: https://doi.org/10.12671/jkfs.2015.28.4.237
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
Pediatric patients with distal forearm bothbone fractures of surgical indication were treated with the Kapandji reduction technique for radius and flexible intramedullary nail for ulna at our institution. The purpose of this study is to evaluate clinical and radiological results.
MATERIALS AND METHODS
From February 2012 to June 2014, we retrospectively evaluated 16 out of 18 cases with distal forearm bothbone fractures treated with the Kapandji reduction technique for radius and flexible intramedullary nail for ulna with at least 1-year follow-up. The average age at operation was 9.1 years (7-13 years).
RESULTS
Adequate reduction for both radius and ulna was achieved for all cases, and none of the cases showed re-displacement until the last follow-up. Mean 6.6 weeks lapsed until bony union was observed for the radius. For the ulna, the mean was 6.5 weeks. All patients gained full wrist range of motion at the last visit.
CONCLUSION
For pediatric distal forearm bothbone fractures, intrafocal Kapandji reduction and internal fixation with Kirschner wire for radius and reduction and internal fixation with a flexible intramedullary nail for ulna is the technique for handy reduction. Use of this technique can prevent re-displacement during the union process and achieve excellent clinical and radiologic results.
- 578 View
- 1 Download

- The Usefulness of Poller Screw with Antegrade Nailing in the Initial Treatment of Infraisthmal Femur Shaft Fracture
- Jeong Hyun Yoo, Hyoung Soo Kim, Chang Geun Kim, Ho Il Kwak, Sang Heon Song
- J Korean Fract Soc 2015;28(4):230-236. Published online October 31, 2015
- DOI: https://doi.org/10.12671/jkfs.2015.28.4.230
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
The purpose of this study was to evaluate the radiologic and clinical outcomes after intramedullary nailing with Poller screw insertion at initial stage in infraisthmal femur shaft fractures.
MATERIALS AND METHODS
Seven consecutive patients (7 femurs) treated with antegrade intramedullary nailing with Poller screw insertion for the infraisthmal femur shaft fracture were reviewed retrospectively. There were 4 male and 3 female patients. Mean age was 46.1 years (20-72 years). Operative time including Poller screw insertion, time for union, malalignment, and range of motion were evaluated.
RESULTS
All 7 cases had primarily healed successfully. Mean time for radiologic union was 19.1 weeks (16-24 weeks) postoperatively. One case had 5 degree valgus malalignment. One case of 15 mm shortening was reported and he required shoe lift orthosis. All cases had a full range of motion in hip and knee joint.
CONCLUSION
Antegrade intramedullary nailing with Poller screw insertion is useful in the initial treatment of infraisthmal femur shaft fracture, because it could provide additional stability. An additional 20 minutes were required but a Poller screw should be considered according to the anatomic location of a femur shaft fracture.
- 667 View
- 6 Download

Case Report
- Extraction of Misplaced Endcap during Tibia Intramedullary Nailing by 'Fish-Hook' Technique: Technical Note
- Se Hyeok Yun, Jae Hyuk Yang
- J Korean Fract Soc 2015;28(3):194-197. Published online July 31, 2015
- DOI: https://doi.org/10.12671/jkfs.2015.28.3.194
-
 Abstract
Abstract
 PDF
PDF - Endcap placement after intramedullary nailing can be cumbersome. Misplacement of the endcap which may be difficult to extract may occur. In this report, a simple Kirschner wire device with 'fish-hook' technique may ease the procedure without further violating bony or soft tissues.
- 573 View
- 0 Download

Original Articles
- A Comparison of Quality of Life Using Short Form 36 between Femoral Shaft Fracture and Tibia Shaft Fracture Treated with Antegrade Nailing
- Sangbong Ko, Hojin Chang
- J Korean Fract Soc 2015;28(3):163-168. Published online July 31, 2015
- DOI: https://doi.org/10.12671/jkfs.2015.28.3.163
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
We sought to compare the quality of life between two similar groups of patients; one group who sustained an isolated femoral shaft fracture, and the other group who sustained an isolated tibial shaft fracture.
MATERIALS AND METHODS
From February 1995 to July 2010, two groups of 168 patients who underwent implant removal operations after intramedullary nailing for an isolated femoral shaft fracture or an isolated tibial shaft fracture were enrolled. Short Form 36 (SF-36) questionnaires were completed at the final follow-up visit. Data analysis was performed by another physician not otherwise involved with clinical evaluation or the surgeries.
RESULTS
Patients ranged in age from 18 to 37 years old. The two groups had similar characteristics, including age, gender ratio, body weight, smoking, and mean follow-up period (all p>0.05). No significant difference in functional outcome using SF-36 was observed between the groups except in the domain of physical functioning (PF) where femoral shaft fracture patients had a slightly higher score (p=0.002).
CONCLUSION
Femoral shaft fracture patients and tibial shaft fracture patients who underwent intramedullary nailing and subsequent implant removal after fracture union with similar epidemiological characteristics had similar functional outcomes using the SF-36 survey, except in the domain of PF, where femoral shaft fracture patients had a slightly better outcome. -
Citations
Citations to this article as recorded by- Health‐related quality of life outcomes after surgical treatment of atypical femur fractures: a multicenter retrospective cohort study
Jonathon Spanyer, Lauren A. Barber, Harrison Lands, Alexander Brown, Mary Bouxsein, Marilyn Heng, Madhusudhan Yakkanti
JBMR Plus.2021;[Epub] CrossRef
- Health‐related quality of life outcomes after surgical treatment of atypical femur fractures: a multicenter retrospective cohort study
- 898 View
- 1 Download
- 1 Crossref

- Analysis of Low-Energy Trochanter Fracture Using the Multiplanar Computed Tomography Image: Application for Intramedullary Nail Fixation
- Gu Hee Jung, Sung Keun Heo, Hyun Je Seo
- J Korean Fract Soc 2015;28(3):155-162. Published online July 31, 2015
- DOI: https://doi.org/10.12671/jkfs.2015.28.3.155
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
The purpose of this radiologic study was to evaluate the geographic patterns of low-energy trochanteric fractures using multiplanar computed tomography (CT) images for application of intramedullary nailing.
MATERIALS AND METHODS
In this study, 117 trochanteric fractures (stable fracture, 39 cases, unstable fractures, 78 cases) sustained from simple slip-down were assessed. The mean age was 78.4 years (range, 60-96 years). Multiplanar CT images were assessed for evaluation of geographic features of trochanteric fracture, and the fracture exit and geographic patterns were analyzed.
RESULTS
The medial and lateral exit of the trochanteric fracture showed no statistical difference by age, bone density, and comorbid disease. The exit was located at an average distance of 10.2 mm (range, 1.0-22.2 mm) from the tip of the greater trochanter (GT), and the medial exit, average distance of 8.1 mm (range, 0.0-18.3 mm) from the tip of the lesser trochanter. It was also found that there was no comminution around the anteromedial cortex of the fracture, and its contact loss was from fracture deformity.
CONCLUSION
Because of no comminution, the contact restoration of the anteromedial cortex resulted in correction of fracture deformity and reduction. Trochanteric nailing by GT tip could be fixed through the proximal fragment of the fracture because the lateral exit is placed at an average distance of 10.2 mm from the GT tip.
- 606 View
- 0 Download

- Treatment of the Femoral Fracture Using Sirus(R) Nail: A Comparison of Complication according to the Entry Potal
- Young Yool Chung, Dong Hyuk Choi, Dae Hyun Yoon, Jung Ho Lee, Ji Hun Park
- J Korean Fract Soc 2015;28(2):103-109. Published online April 30, 2015
- DOI: https://doi.org/10.12671/jkfs.2015.28.2.103
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
The purpose of this study is to analyze the clinical results of fixation using Sirus(R) nail in patients with femoral subtrochanteric and shaft fracture and the difference in the frequency of complications according to the entry portal.
MATERIALS AND METHODS
From July 2006 to August 2013, at least 1-year clinical follow-up, we retrospectively analyzed 36 cases with femoral subtrochanteric (15 cases) and shaft fracture (21 cases) who underwent surgery using Sirus(R) nail. We reviewed the records of operation time, intra-operative amounts of bleeding and complications. At last follow-up, we reviewed clinical results by Ray-Sanders criteria and analyzed the periods of bone union on the radiograph. We also measured changing of the femoral neck-shaft angle in the subtrochanteric fractures and angulation in the shaft fractures, respectively. Considering anatomical variation of the trochanter and fracture position of subtrochanteric and femoral shaft, entry points were divided into subgroups, and the clinical results were compared.
RESULTS
The mean Ray-Sanders score was 27.4, 27 cases (75.0%) were good or excellent. The mean periods of bone union was 21.1 weeks in 31 cases. The mean neck-shaft angles were 135.7o preoperatively, 130.2o postoperatively. The mean angulation of the femur was 24.4o preoperatively, 2.4o postoperatively in patients of femoral shaft fractures. Despite no statistical significance, greater trochanter tip entry point and lateral entry point had a higher rate of frequency than medial entry point, with respect to the occurrence of iatrogenic fracture and malalignment.
CONCLUSION
Using Sirus(R) nail for femoral subtrochanteric and shaft fractures showed good clinical and radiographic results and a high rate of union. Medial entry point yielded slightly better results in the occurrence of iatrogenic fracture and malalignment, compared to greater trochanter tip entry point and lateral entry point.
- 871 View
- 7 Download

- Perioperative Blood Loss in Intramedullary Hip Screw for Intertrochanteric Fracture: Analysis of Risk Factors
- Jai Hyung Park, Hwa Jae Jung, Hun Kyu Shin, Eugene Kim, Se Jin Park, Taeg Su Ko, Jong Hyon Park
- J Korean Fract Soc 2015;28(1):53-58. Published online January 31, 2015
- DOI: https://doi.org/10.12671/jkfs.2015.28.1.53
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
We compared visible blood loss and calculated blood loss after intramedullary fixation in intertrochanteric fracture, and evaluated correlation between blood loss and its risk factors.
MATERIALS AND METHODS
A total of 256 patients who underwent closed reduction and intramedullary fixation in femoral intertrochanteric fracture between 2004 and 2013 were enrolled in this study. The total blood loss was calculated using the formula reported by Mercuiali and Brecher. We analyzed several factors, including fracture pattern (according to Evans classification), gender, age, body mass index (BMI), anesthesia method, cardiovascular and cerebrovascular disease, preoperative anemia, American Society of Anesthesiologists (ASA) score and use of antithrombotic agents.
RESULTS
Total calculated blood loss (2,100+/-1,632 ml) differed significantly from visible blood loss (564+/-319 ml). In addition, the blood loss of unstable fracture patient was 2,496+/-1,395 ml and multivariate analysis showed a significant relationship between blood loss and fracture pattern (p<0.01). However, other factors showed no statistically significant difference.
CONCLUSION
Total calculated blood loss was much greater than visible blood loss. Patients with unstable intertrochanteric fracture should be treated with care in order to reduce blood loss.
- 628 View
- 0 Download

- Comparison of Greater Trochanter Versus Piriformis Entry Nail for Treatment of Femur Shaft Fracture
- Jong Hee Lee, Jong Hoon Park, Si Yeong Park, Seong Cheol Park, Seung Beom Han
- J Korean Fract Soc 2014;27(4):287-293. Published online October 31, 2014
- DOI: https://doi.org/10.12671/jkfs.2014.27.4.287
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
The purpose of this study was to compare the clinical outcome of femoral shaft fracture treatment with intramedullary nailing performed using a greater trochanter and a piriformis entry nail.
MATERIALS AND METHODS
A total of 57 patients treated by antegrade nailing for a femoral shaft fracture between January 2008 and April 2013 were included in this study. We evaluated postoperative radiographs of 57 femoral shaft fractures stabilized with femoral intramedullary nailing at a single institutional center. The cases included 25 piriformis fossa entry nails and 32 greater trochanter entry nails. Outcome measures included the alignment, union rate and duration of union, complications, operation time, intra-operative bleeding, and a pain rating scale.
RESULTS
The alignment, union rate, and duration of union did not differ significantly between the groups with piriformis fossa and trochanteric nailing. In addition, no significant differences regarding complications and operation time were observed between the two groups. Less intra-operative bleeding was observed in the trochanteric nailing group. This difference was statistically significant (p=0.044).
CONCLUSION
Use of a femoral nail specially designed for the trochanteric insertion resulted in equally high union rates, duration of union, and low complication rates. Thus, greater trochanter entry nails were similar to conventional antegrade femoral nailing through the piriformis fossa.
- 993 View
- 2 Download

- Surgical Fitness for Trochanteric Fracture in Elderly: Prospective Study
- Gu Hee Jung, Jong Seo Lee, Sung Gun Heo, Jae Do Kim, Hyun Ik Cho
- J Korean Fract Soc 2014;27(4):261-266. Published online October 31, 2014
- DOI: https://doi.org/10.12671/jkfs.2014.27.4.261
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
The purpose of this study was to evaluate the risks of undergoing intramedullary nailing with minimum surgical optimization (fast-track) for geriatric trochanter fracture due to fall from a standing height.
MATERIALS AND METHODS
From May 2006 to August 2013, 48 fractures were enrolled in fast-track, and were an average age of patients was 77.6 years (range, 62-97 years). They underwent primary testing for anesthesia, including basic body fluid test, arterial blood, electrocardiography, and chest radiographs. The time from visit to surgery was 28.9 hours (range, 1-96 hours).
RESULTS
During hospitalization, there was one case of stress-induced cardiac arrest; however, other complications, infection, and 30-day mortality did not occur. According to preoperative classic test, the average albumin was 3.45 g/dl, blood sugar, 169 mg/dl, blood urea nitrogen, 20.5 mg/dl, Cr, 1.5 mg/dl, Na, 135.3 mEq/L, and K, 4.21 mEq/L. The average PaCO2 of arterial blood was 37.6 mmHg.
CONCLUSION
We found that the fast-track for trochanteric fracture due to slip-down was relatively safe, and could be considered as a therapeutic approach.
- 579 View
- 2 Download

- Intramedullary Nailing of Distal Tibial Fractures with Percutaneous Reduction by Pointed Reduction Forceps
- Jae Kwang Hwang, Chung Hwan Kim, Young Joon Choi, Gi Won Lee, Hyun Il Lee, Tae Kyung Kim
- J Korean Fract Soc 2014;27(2):144-150. Published online April 30, 2014
- DOI: https://doi.org/10.12671/jkfs.2014.27.2.144
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
The purpose of this study is to analyze the radiographic and clinical results of intramedullary nailing after percutaneous reduction using pointed reduction forceps for spiral or oblique fractures of the distal tibia. The benefit of percutaneous reduction using pointed reduction forceps in anatomical reduction and maintenance was assessed.
MATERIALS AND METHODS
From January 2005 to December 2009, 47 cases of distal one-third tibial fracture were managed by intramedullary nailing using pointed reduction forceps. Thirty-eight cases were spiral fracture and nine cases were oblique fracture. In all cases, the percutaneous reduction was achieved using pointed reduction forceps under fluoroscopy control. While maintaining the reduction with the pointed reduction forceps, the intramedullary nail was inserted. The pointed reduction forceps were removed after insertion of proximal and distal inter-locking screws. Alignment was evaluated with anterior-posterior and lateral radiographs taken immediately post-operation and at the time of union.
RESULTS
At immediate post-operation, the mean displacement of valgus and anterior angulation was 0.57degrees and 0.24degrees, respectively. That of valgus and anterior angulation at bone union was 0.37degrees and 0.16degrees, respectively. The average duration of bone union was 16.1 weeks.
CONCLUSION
Intramedullary nailing with percutaneous reduction using pointed reduction forceps for distal tibial fractures was an easy and effective method for achievement of accurate alignment intra-operatively. Accurate alignment was successfully maintained until bone union.
- 731 View
- 2 Download

- Results of Intramedullary Nailing of Femoral Shaft Fracture: Trochanteric Entry Portal (Sirus Nail) versus Piriformis Entry Portal (M/DN Nail)
- Sang Ho Ha, Woong Hee Kim, Gwang Chul Lee
- J Korean Fract Soc 2014;27(1):50-57. Published online January 31, 2014
- DOI: https://doi.org/10.12671/jkfs.2014.27.1.50
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To compare treatment results obtained using the trochanteric (Sirus nail) entry portal with those obtained using the Piriformis fossa (M/DN) entry portal during intramedullary (IM) nailing of femur shaft fractures.
MATERIALS AND METHODS
Four hundreds and thirty-two patients treated for femur shaft fracture using IM nails from February, 2001 to May, 2010 were divided into two groups. group 1 was composed of 180 patients treated through the trochanteric (Sirus nail; n=180) entry portal, while group 2 contained 170 patients treated through the piriformis fossa (M/DN nail; n=170) entry portal. We compared the clinical and radiographic findings of both groups to evaluate the treatment results.
RESULTS
Functional result, range of motion and union time (18, 20 weeks) were similar in both groups. The operation time of patients in the over-weighted group was 90 minutes in group 1 and 120 minutes in group 2 (p<0.05). Additionally, the blood loss was 280 ml in group 1 and 335 ml in group 2, and in case of over-weight patients, group 2 showed more blood loss (p<0.05). The duration of exposure to fluoroscopy differed slightly, with group 1 being less exposed than group 2; however, this difference was not significant (p>0.05). There were 18 iatrogenic fractures in group 1 and 4 in group 2 (p<0.05).
CONCLUSION
There was not much difference in complications based on clinical and radiographic findings of both groups. For groups using the trochanteric entry portal, the operation time was shorter and blood loss was lower than in groups using the piriformis entry portal. Iatrogenic fracture occurred more often in the group using the trochanteric entry portal than in the group using the piriformis entry portal. -
Citations
Citations to this article as recorded by- Analysis of different entry portals for femoral nail with two different nail designs-straight nail versus lateral angulated nail - Does it make a difference?
Sanjay Yadav, Saurabh Singh, Anil Kumar Rai
Journal of Clinical Orthopaedics and Trauma.2019; 10(5): 912. CrossRef - Comparing Entry Points for Antegrade Nailing of Femoral Shaft Fractures
Ujash Sheth, Chetan Gohal, Jaskarndip Chahal, Aaron Nauth, Tim Dwyer
Orthopedics.2016;[Epub] CrossRef - The Curative Effect Comparison Between Prolonged Third Generation of Gamma Nail and Prolonged Dynamic Hip Screw Internal Fixation in Treating Femoral Intertrochanteric Fracture and the Effect on Infection
Wenye He, Wei Zhang
Cell Biochemistry and Biophysics.2015; 71(2): 695. CrossRef - Treatment of Femur Subtrochanteric Fracture Using the Intramedullary Long Nail; Comparison of Closed Reduction and Minimal Open Reduction
Sang Joon Lee, Sang Hong Lee, Sang Soo Park, Hyung Seok Park
Journal of the Korean Orthopaedic Association.2015; 50(1): 18. CrossRef - Failure to Remove a Trochanteric Entry Femoral Nail and Its Cause in Adolescent Patients: Two Cases Report
Ji-Hwan Kim, Seung-Oh Nam, Young-Soo Byun, Han-Sang Kim
Journal of the Korean Fracture Society.2015; 28(1): 71. CrossRef - Treatment of the Femoral Fracture Using Sirus® Nail: A Comparison of Complication according to the Entry Potal
Young-Yool Chung, Dong-Hyuk Choi, Dae-Hyun Yoon, Jung-Ho Lee, Ji-Hun Park
Journal of the Korean Fracture Society.2015; 28(2): 103. CrossRef - Comparison of Greater Trochanter Versus Piriformis Entry Nail for Treatment of Femur Shaft Fracture
Jong-Hee Lee, Jong-Hoon Park, Si-Yeong Park, Seong-Cheol Park, Seung-Beom Han
Journal of the Korean Fracture Society.2014; 27(4): 287. CrossRef
- Analysis of different entry portals for femoral nail with two different nail designs-straight nail versus lateral angulated nail - Does it make a difference?
- 1,881 View
- 21 Download
- 7 Crossref

- Treatment of Periprosthetic Femoral Fractures Following Total Knee Arthroplasty
- Lih Wang, Kyu Yeol Lee, Chul Hong Kim, Myung Jin Lee, Min Soo Kang, Jin Soo Hwang, Sun Hyo Kim
- J Korean Fract Soc 2014;27(1):42-49. Published online January 31, 2014
- DOI: https://doi.org/10.12671/jkfs.2014.27.1.42
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
The purpose of this study is to compare the treatment results of fracture fixations by using two minimal invasive techniques for patients with periprosthetic femoral fractures following total knee arthroplasty.
MATERIALS AND METHODS
We reviewed 36 patients (5 males, 31 females) of periprosthetic femoral fractures whom were treated surgically between January 2005 and January 2011. Mean patient age was 68.9 years (range, 43 to 81 years) old and the follow-up period averaged 41 months (range, 18 to 72 months). Nineteen patients were treated with minimal invasive locking plate fixations (group I) and 17 patients with retrograde intramedullary nailing (group II). Clinical and radiological outcomes in each group were comparatively analyzed.
RESULTS
Successful bone unions occurred in all patients and the mean time to bone union was 3.7 months in group I and 4.2 months in group II. There were no statistical differences between the two groups according to mean operative time and mean intraoperative blood loss. There were also no statistical differences between two groups according to clinical outcomes but the valgus deformity was apparent in group II and radiological outcomes revealed significant differences between the two groups.
CONCLUSION
For the treatment of periprosthetic femoral fractures after total knee arthroplasty, two minimal invasive techniques have shown good clinical results. However, the minimal invasive plate fixation showed better results in the radiological alignments. -
Citations
Citations to this article as recorded by- The Result of Treatment of Femoral Periprosthetic Fractures after Total Knee Arthroplasty
Jun-Beom Kim, In-Soo Song, Dong-Hyuk Sun, Hyun Choi
Journal of the Korean Orthopaedic Association.2014; 49(6): 446. CrossRef
- The Result of Treatment of Femoral Periprosthetic Fractures after Total Knee Arthroplasty
- 1,133 View
- 5 Download
- 1 Crossref

Case Report
- Breakage of Reamer during Tibia Intramedullary Nailing: A Case Report
- Ho Yoon Kwak, Jin Su Kim, Ki Won Young, Joo Won Joh, Sae Min Hwang
- J Korean Fract Soc 2013;26(4):333-337. Published online October 31, 2013
- DOI: https://doi.org/10.12671/jkfs.2013.26.4.333
-
 Abstract
Abstract
 PDF
PDF - The reamer crack, followed by breakage at its distal part occurred during intramedullary nailing of tibial shaft fracture. The broken reamer was trapped in the intramedullary canal, making it very difficult to pull out. We successfully extracted the broken reamer by retrograde impaction through the fracture site and completed intramedullary nailing procedure. Thus, we present this case with a review of the literature.
-
Citations
Citations to this article as recorded by- A novel technique for retrieval of a broken flexible reamer during proximal femur nailing: A case report and review of the literature
Gowtham Sushruth, Sudhir Shankar Mane, Murali Krishna
Journal of Orthopaedic Reports.2026; 5(1): 100691. CrossRef - Clamshell Corticotomy: A Technique to Address Challenges of Narrow Medullary Canal during Intramedullary Nailing of Tibial Shaft Fracture Fixation
Ranjith Kumar Yalamanchili, Deepankar Satapathy, Deepak Kumar Maley, Syed Ifthekar, Maheshwar Lakkireddy
Journal of West African College of Surgeons.2025; 15(4): 481. CrossRef - ‘Extended tibia osteotomy’: a technical tip for removal of incarcerated reamer with broken guide wire bead during tibia nailing and literature review
Pulak Vatsya, Samarth Mittal, Aashraya Karpe, Vivek Trikha
BMJ Case Reports.2022; 15(3): e247812. CrossRef - Removal of intra-operatively broken flexible reamer: An innovative use of jumbo cutter
Tankeshwar Boruah, Sapan Kumar, Mohit Kumar Patralekh, Shambhu Prashad, Vibash Chandra, Ijack Debbarma, Ramesh Kumar
Journal of Clinical Orthopaedics and Trauma.2019; 10(3): 620. CrossRef
- A novel technique for retrieval of a broken flexible reamer during proximal femur nailing: A case report and review of the literature
- 937 View
- 5 Download
- 4 Crossref

Original Articles
- Outcomes and Analysis of Factors Affecting Bone Union after Interlocking Intramedullary Nailing in Segmental Tibia Fractures
- Sang Soo Park, Jun Young Lee, Sang Ho Ha, Sung Hae Park
- J Korean Fract Soc 2013;26(4):275-283. Published online October 31, 2013
- DOI: https://doi.org/10.12671/jkfs.2013.26.4.275
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To evaluate the radiological results and complications of interlocking intramedullary nailing for segmental tibia fractures.
MATERIALS AND METHODS
Twenty-six patients (26 cases) who underwent interlocking intramedullary nailing for segmental tibia fractures between January 2003 and May 2011 were followed for more than one year. We evaluated the complications and statistically analyzed the factors influencing bone union, including open fracture, fracture site, reaming, postoperative angulation, and postoperative fracture gap.
RESULTS
Nineteen cases (73%) achieved bone union with one operation at an average of 7 months (range, 5 to 11). Seven cases had secondary procedures before achieving union. Complications included 7 cases of nonunion, 3 cases of incomplete peroneal nerve injury, 2 cases of superficial infection, 1 case of compartment syndrome. Factors showing statistically significant differences were open fracture, postoperative angulation, and postoperative fracture gap. Factors showing no statistically significant difference were fracture site and reaming.
CONCLUSION
Nonunion is the most common complication in interlocking intramedullary nailing for segmental tibia fractures. To minimize this complication, comprehension of surgical techniques to reduce anatomically and careful evaluation of the fracture are required. -
Citations
Citations to this article as recorded by- Clinical Outcome after Treatment of Tibia Segmental Fracture with Intramedullary Nailing and Minimal Invasive Plate Osteosynthesis
Jun Young Lee, Hyung Seok Park, Dong Hyuk Cha
Journal of the Korean Fracture Society.2020; 33(3): 142. CrossRef
- Clinical Outcome after Treatment of Tibia Segmental Fracture with Intramedullary Nailing and Minimal Invasive Plate Osteosynthesis
- 943 View
- 3 Download
- 1 Crossref

- Augmentative Locking Plate Fixation for the Treatment of Femoral Nonunion after Intramedullary Nailing
- Ki Chul Park, Chul Woong Kim, Kyu Tae Hwang, Ye Soo Park
- J Korean Fract Soc 2013;26(4):268-274. Published online October 31, 2013
- DOI: https://doi.org/10.12671/jkfs.2013.26.4.268
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To evaluate the efficacy of the augmentative locking compression plate fixation in the treatment of femoral shaft nonunion occurring after intramedullary nailing.
MATERIALS AND METHODS
Between July 2004 and September 2012, a total of 17 patients (twelve men, five women, average age 52.5 years) who had femoral nonunions after primary intramedullary nailing for femoral shaft fractures were reviewed. The mean period of nonunion after primary nailing was 18.5 months. Leaving the nail in situ, an augmentative locking plate was applied to the nonunion site with simultaneous autogenous bone grafting, except for five hypertrophic nonunions. We followed up all patients with plain radiograph and evaluated clinical status to determine bone union.
RESULTS
All patients demonstrated evidence of fracture union with an average follow-up time of 5.0 (range 2 to 9) months. The time of operation was an average of 115 (range 45 to 160) minutes, and mean blood loss was 345.9 (range 150 to 700) ml. Two patients noted discomfort at the distal portion of plate, and one noted discomfort of donor site, but functional limitation was not observed in all patients.
CONCLUSION
Augmentative locking plate fixation for diaphyseal femoral nonunion after intramedullary nailing is a reasonable treatment option with increased stability.
- 714 View
- 3 Download

- Clinical Outcomes of the Tibia Segmental Fractures Treated by Intramedullary Nail Using Various Reduction Techniques
- Oog Jin Shon, Ji Hoon Shin, Chul Wung Ha
- J Korean Fract Soc 2013;26(1):50-55. Published online January 31, 2013
- DOI: https://doi.org/10.12671/jkfs.2013.26.1.50
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
We evaluated the clinical outcomes of tibia segmental fractures treated by intramedullary nailing using various reduction techniques.
MATERIALS AND METHODS
From January 2003 to June 2009, 18 segmental tibial fracture patients treated by intramedullary nail were enrolled with a minimum 12-month follow-up. The mean follow-up was 38 months (range 15-72). According to the AO classification, the fractures were types 42C2.1, 42C2.2, and 42C2.3 in four, ten, and four patients, respectively. Ten fractures were closed and eight were open. We used various techniques for reduction during operation and investigated bone union time and complication (non-union, malunion etc.).
RESULTS
Bone grafting was performed in three patients. Complete union was achieved in all patients. The mean time for union was 16.3 weeks (range 12-21), except in three delayed union patients. All radiological evaluations showed good alignment (less than 5 degree) except in two patients; and the mean deformity angle was 2.2 degree. Knee range of motion (ROM) was 129 degree, and ankle ROM was 68 degree. Local wound infection occurred in two patients.
CONCLUSION
Intramedullary nailing is a successful method in the acute management of segmental tibial fractures, if accompanied by appropriate reduction technique.
- 587 View
- 1 Download

- A Comparison between Compression Hip Screw and Intramedullary Nail for the Treatment of AO/OTA A2.2 Intertrochanteric Femoral Fracture
- Phil Hyun Chung, Suk Kang, Jong Pil Kim, Young Sung Kim, Ho Min Lee, Jong Hyun Kim
- J Korean Fract Soc 2013;26(1):44-49. Published online January 31, 2013
- DOI: https://doi.org/10.12671/jkfs.2013.26.1.44
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To compare the result between the compression hip screw (CHS) and intramedullary (IM) nail for the treatment of AO/OTA A2.2 intertrochanteric fracture.
MATERIALS AND METHODS
We retrospectively reviewed 95 cases of AO/OTA A2.2 intertrochanteric fracture, which were treated with CHS or IM nail by one surgeon from March 1994 to December 2009. One group was treated with CHS (Group I, 28 cases) and the other was treated with IM nail (Group II, 67 cases). We evaluated the mean operation time, the amount of bleeding and transfusion, hospital duration, radiological results and the clinical outcome with the mobility score of Parker and Palmer.
RESULTS
Radiologically, the tip-apex distance, change of neck-shaft angle, and union time were not significantly different between both groups (p>0.05). Clinically, the mean operation time, the amount of bleeding and transfusion, hospital duration and the mobility score were not significantly different (p>0.05). The post-operative complications were lag screw slippage over 25 mm (1 case) and loosening of device (1 case) in group I. In group II, there were perforation of the femoral head (1 case), nail breakage (1 case) and deep infection (1 case).
CONCLUSION
There was no significant differences that are clinical and radiological results in the treatment of AO/OTA A2.2 intertrochanteric fracture, using CHS and IM nail. -
Citations
Citations to this article as recorded by- A Comparison of Clinical Results between Compression Hip Screw and Proximal Femoral Nail as the Treatment of AO/OTA 31-A2.2 Intertrochanteric Femoral Fractures
Phil Hyun Chung, Suk Kang, Jong Pil Kim, Young Sung Kim, Ho Min Lee, In Hwa Back, Kyeong Soo Eom
Journal of the Korean Orthopaedic Association.2016; 51(6): 493. CrossRef
- A Comparison of Clinical Results between Compression Hip Screw and Proximal Femoral Nail as the Treatment of AO/OTA 31-A2.2 Intertrochanteric Femoral Fractures
- 1,983 View
- 2 Download
- 1 Crossref

- Polarus Intramedullary Nail for Proximal Humeral and Humeral Shaft Fractures in Elderly Patients with Osteoporosis
- Youn Soo Hwang, Kwang Yeol Kim, Hyung Chun Kim, Su Han Ahn, Dong Eun Lee
- J Korean Fract Soc 2013;26(1):14-20. Published online January 31, 2013
- DOI: https://doi.org/10.12671/jkfs.2013.26.1.14
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To assess the effectiveness of optimal treatment of proximal humeral fractures and humeral shaft fractures in elderly patients with osteoporosis using the Polarus nail.
MATERIALS AND METHODS
Twenty-three patients with proximal humeral and humeral shaft fractures in elderly osteoporosis patients were treated using the Polarus intramedullary nail. Nine patients had proximal humeral fracture, 10 had humeral shaft fracture and 4 had the proximal humeral frac-ture extended diaphyseally. Radiological outcomes included the bone-union and the degree of re-sidual deformity. The residual deformities of the proximal humerus were assessed by the neck-shaft angle and the shaft angulation. Clinical outcome was assessed with the American Shoulder and Elbow Surgeons (ASES) score.
RESULTS
All cases had bony union and the mean union period was 16.5 weeks. The average neck/shaft alignment at the time of bone union was 135degrees and varus deformities of neck-shaft angle was not seen in all patients. Varus shaft angulation was seen in 5 patients. The mean ASES score after surgery was 86.7 points.
CONCLUSION
The Polarus intramedullary nail is effective for the treatment of proximal humeral and humeral shaft fractures in elderly patients with osteoporosis because it not only enables early postoperative mobilization, but also obtains bone-union without avascular necrosis and nonunion. -
Citations
Citations to this article as recorded by- Surgical Management of Osteoporotic Fractures: Humerus Shaft Fractures
Shankar Ramaprasad Kurpad
Indian Journal of Orthopaedics.2025; 59(8): 1053. CrossRef
- Surgical Management of Osteoporotic Fractures: Humerus Shaft Fractures
- 1,023 View
- 5 Download
- 1 Crossref

- Treatment for Bone Defect of Open Tibial Fractures by Using Intramedullary Nail Fixation with Autogenous Iliac Bone Graft
- Hyub Sakong, Ki Cheor Bae, Chul Hyun Cho, Kyung Jae Lee, Eun Seok Son, Du Han Kim
- J Korean Fract Soc 2012;25(4):288-294. Published online October 31, 2012
- DOI: https://doi.org/10.12671/jkfs.2012.25.4.288
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
This study was conducted to evaluate the results of intramedullary nail fixation with autogenous iliac bone graft for defects of bone after tibial fractures.
MATERIALS AND METHODS
Ten patients with bone defects in tibial fractures who had been treated with intramedullary nail fixation with autogenous iliac bone graft between May 2005 and September 2008 with more than 12 month follow-up were subject to study. Of the 10 patients, 8 were male and 2 were female, and the mean age was 50.2 years (29~76 years). By cause of accident, motor vehicle accidents caused 9 cases, a crush caused 1 case, and the average follow-up period was 21.9 months (12~42 months). Radiologically, we analyzed the union of the bone defect on simple x-ray and clinical evaluation was performed using the estimate method of Mekhali.
RESULTS
This study reveals that there was radiological union in all 10 cases and the mean time to union was 8.4 months (5~18 months). By clinical evaluation according to Mekhali's estimate method, 9 patients had excellent outcomes and 1 patient had limitation of motion in the ankle joint rated as a fair clinical result. None of patients developed complications post-operatively.
CONCLUSION
Our study demonstrated that the intramedullary nail fixation with autogenous iliac bone graft can be a useful operative method because it can remove external fixators early and reduce complications, and autogenous bones have exceptional osteoconduction, osteoinduction, and bone-forming ability resulting in excellent union of bones.
- 761 View
- 7 Download

- Alteration of the Patella Tendon Length after Intramedullary Nail in Tibial Shaft Fractures
- Dong Eun Shin, Ki Shik Nam, Jin Young Bang, Ji Hoon Chang
- J Korean Fract Soc 2012;25(4):283-287. Published online October 31, 2012
- DOI: https://doi.org/10.12671/jkfs.2012.25.4.283
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To compare and analyze length change of patella tendon after intramedullary nailing of tibial shaft fracture using transtendinous approach.
MATERIALS AND METHODS
Thirty-two cases were analyzed from December, 1999 to December, 2005. Insall Salvati ratios were estimated. Severity of initial trauma, duration of nail retension, knee function and pain on change of length of patellar tendon was evaluated.
RESULTS
Mean duration of nail retention was twenty-two months. The shortening of patella tendon was observed in 25 cases (p<0.001). The effect of AO type and the duration of nail retension on the decrease of Insall Salvati ratio was not significant (p>0.05, p=0.778). Lysholom score decrease to 89.5. There was no significant difference between the shortening of patellar tendon length and knee pain (p=0.058).
CONCLUSION
After intramedullary nailing for closed tibia fracture, shortening of patellar tendon length is observed. That is irrelevant to the fracture type and the duration of nail retension. The shortening of patella tendon length may contribute to decreasing of knee function, but it was no significance of knee pain after intramedullary nailing.
- 729 View
- 0 Download

Case Report
- Repeated Metal Breakage in a Femoral Shaft Fracture with Lateral Bowing: A Case Report
- Dong Soo Kim, Yong Min Kim, Eui Sung Choi, Hyun Chul Shon, Kyoung Jin Park, Byung Ki Cho, Ji Kang Park, Hyun Cheol Lee, Kyung Ho Hong
- J Korean Fract Soc 2012;25(2):136-141. Published online April 30, 2012
- DOI: https://doi.org/10.12671/jkfs.2012.25.2.136
-
 Abstract
Abstract
 PDF
PDF - Fractures of the femoral shaft with marked bowing face some obstacles in fixation of the fracture such as difficulty in insertion of the intramedullary nail (IM nail) or exact contouring plate. Locking compression plates (LCP) are an option to manage this problem. However, we experienced consecutive breakage of LCP twice and IM nail once in an 80-year-old female. Finally, union of the fracture was achieved after fixation of the IM nail and additional plate together. Fractures of the femur shaft with marked bowing are thought to have different biomechanical properties; therefore, we present this case with a review of the literature.
-
Citations
Citations to this article as recorded by- Comparative analysis of operation time and intraoperative fluoroscopy time in intramedullary and extramedullary fixation of trochanteric fractures
Milan Mitkovic, Sasa Milenkovic, Ivan Micic, Predrag Stojiljkovic, Igor Kostic, Milorad Mitkovic
Vojnosanitetski pregled.2022; 79(2): 177. CrossRef - Pre-operative planning for fracture fixation using locking plates: device configuration and other considerations
Alisdair R. MacLeod, Pankaj Pankaj
Injury.2018; 49: S12. CrossRef - Letter: Repeated Metal Breakage in a Femoral Shaft Fracture with Lateral Bowing - A Case Report -
Hae Seok Koh
Journal of the Korean Fracture Society.2012; 25(3): 240. CrossRef
- Comparative analysis of operation time and intraoperative fluoroscopy time in intramedullary and extramedullary fixation of trochanteric fractures
- 815 View
- 3 Download
- 3 Crossref

Original Articles
- The Fate of Butterfly Fragments in Extremity Shaft Comminuted Fractures Treated with Closed Interlocking Intramedullary Nailing
- Ki Chan An, Yoon Jun Kim, Jang Suk Choi, Seung Suk Seo, Hi Chul Gwak, Dae Won Jung, Dong Woo Jeong
- J Korean Fract Soc 2012;25(1):46-51. Published online January 31, 2012
- DOI: https://doi.org/10.12671/jkfs.2012.25.1.46
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
For conservative treatment of shaft fractures, the butterfly fragments that were somewhat larger in the closed intra-medullary (IM) nailing. The results of treatment were monitored using radiography separately for the weight-bearing femur and non-weight-bearing humerus.
MATERIALS AND METHODS
27 from Group I and 31 from Group II. In the two groups, the displacement and angulation changes in the fragments, and the degree of improvement of these two factors, were compared using follow-up radiography.
RESULTS
The mean angulation of fragments in Groups I and II were 9.2degrees and 9.6degrees, and the mean degree of displacement of the fragments in Groups I and II were 16.7 mm and 21.2 mm, respectively. Follow-up radiography showed that the above factors improved in both groups. The degree of displacement was significantly lower in the normal cases than in the complicated cases (p=0.001).
CONCLUSION
Displacement and angulation gradually improved in both groups. It was found that the degree of displacement after the initial reduction is more important than the influence of anatomical position or weight bearing. This indicates that care should be taken when inserting IM nails to prevent displacement or angulation. -
Citations
Citations to this article as recorded by- Risk Factors for Failure of Nonsurgical Management of Ulnar Shaft Fractures
Carew C. Giberson-Chen, Cassandra M. Chruscielski, Dafang Zhang, Philip E. Blazar, Brandon Earp
The Journal of Hand Surgery.2025; 50(4): 497.e1. CrossRef - The impact of the third fragment features on the healing of femoral shaft fractures managed with intramedullary nailing: a radiological study
Giovanni Vicenti, Massimiliano Carrozzo, Vincenzo Caiaffa, Antonella Abate, Giuseppe Solarino, Davide Bizzoca, Roberto Maddalena, Giulia Colasuonno, Vittorio Nappi, Francesco Rifino, Biagio Moretti
International Orthopaedics.2019; 43(1): 193. CrossRef - Reply to “Letter to the Editor on: The impact of the third fragment features on the healing of femoral shaft fractures managed with intramedullary nailing: a radiological study”
Giovanni Vicenti, Massimiliano Carrozzo, Davide Bizzoca, Biagio Moretti
International Orthopaedics.2019; 43(6): 1545. CrossRef - Letter to the Editor on “The impact of the third fragment features on the healing of femoral shaft fractures managed with intramedullary nailing: a radiological study”
Shih-Jie Lin, Kevin Liaw, Tsan-Wen Huang
International Orthopaedics.2019; 43(6): 1543. CrossRef - The impact of the third fragment features on the healing of femoral shaft fractures managed with intramedullary nailing: a radiological study
Giovanni Vicenti, Massimiliano Carrozzo, Vincenzo Caiaffa, Antonella Abate, Giuseppe Solarino, Davide Bizzoca, Roberto Maddalena, Giulia Colasuonno, Vittorio Nappi, Francesco Rifino, Biagio Moretti
International Orthopaedics.2018;[Epub] CrossRef - Comparison of the Result of the Intramedullary Nail Fixation and Plate Fixation in Humeral Shaft Fracture with Butterfly Fragments
Duk-Hwan Kho, Hyeung-June Kim, Byoung-Min Kim, Hyun-Ryong Hwang
The Korean Journal of Sports Medicine.2016; 34(2): 120. CrossRef - Clinical and Radiographical Follow-up for Residual Displacement of Fracture Fragments after Interlocking Intramedullary Nailing in Humeral Shaft Fractures
Jae-Kwang Yum, Dong-Ju Lim, Eui-Yub Jung, Su-Een Sohn
The Journal of the Korean Shoulder and Elbow Society.2013; 16(2): 107. CrossRef
- Risk Factors for Failure of Nonsurgical Management of Ulnar Shaft Fractures
- 1,333 View
- 11 Download
- 7 Crossref

- Surgical Techniques for Percutaneous Reduction by Towel Clips and Percutaneous Intramedullary Fixation with Steinmann Pins for Clavicle Shaft Fractures
- Ki Do Hong, Jae Chun Sim, Sung Sik Ha, Tae Ho Kim, Jong Hyun Kim, Jong Seong Lee
- J Korean Fract Soc 2012;25(1):31-37. Published online January 31, 2012
- DOI: https://doi.org/10.12671/jkfs.2012.25.1.31
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To report the clinical results of surgical treatment of clavicle shaft fracture by percutaneous reduction with towel clips and percutaneous intramedullary pin fixation.
MATERIALS AND METHODS
This study reviewed the results of 80 cases of clavicle shaft fracture treated by percutaneous reduction with towel clips and percutaneous intramedullary pin fixation with Steinmann pins from January 2002 to August 2010, after follow-up for 12 months or more. We evaluated the clinical results, such as union time and complications.
RESULTS
Bone union was evident in all cases and the mean time for bone union to appear on radiological findings was 10.3 weeks. Using Kang's criteria, 78 of the 80 patients (97.5%) showed good results and there were no severe complications.
CONCLUSION
Percutaneous reduction with towel clips and the percutaneous intramedullary pin fixation method showed good results for treating clavicle shaft fracture. -
Citations
Citations to this article as recorded by- Additional fixation using a metal plate with bioresorbable screws and wires for robinson type 2B clavicle fracture
Woo Jin shin, Young Woo Chung, Seon Do Kim, Ki-Yong An
Clinics in Shoulder and Elbow.2020; 23(4): 205. CrossRef - A Comparison between Minimally Invasive Percutaneous Plate Osteosynthesis and Plate Fixation in the Treatment of Clavicle Midshaft Fracture
Seong-Ho Yoo, Suk-Woong Kang, Bu-Hwan Kim, Moo-Ho Song, Yeong-Joon Kim, Gyu-Taek Park, Chang-Hun Kwack
Journal of the Korean Orthopaedic Association.2017; 52(1): 1. CrossRef
- Additional fixation using a metal plate with bioresorbable screws and wires for robinson type 2B clavicle fracture
- 972 View
- 3 Download
- 2 Crossref

- Comparative Analysis of Minimally Invasive Plate Osteosynthesis Using Periarticular Plate and Intramedullary Nailing in Distal Tibial Metaphyseal Fractures
- Gwang Chul Lee, Jun Young Lee, Sang Ho Ha, Hong Moon Sohn, Yi Kyu Park
- J Korean Fract Soc 2012;25(1):20-25. Published online January 31, 2012
- DOI: https://doi.org/10.12671/jkfs.2012.25.1.20
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To compare results between minimally invasive plate osteosynthesis using a periarticular plate and intramedullary nailing in distal tibial metaphyseal fractures in two treatment groups.
MATERIALS AND METHODS
Sixty-one cases of distal tibial metaphyseal fractures from December 2008 to December 2009 were evaluated. The minimal follow-up period was 12 months. Thirty patients treated by minimally invasive plate osteosynthesis using a periarticular plate were Group A; 31 patients treated by intramedullary nailing were Group B. We compared and analyzed the results of each group by radiological and clinical assessments.
RESULTS
The mean bony union time was 16.4 weeks in Group A and 17.2 weeks in Group B. The mean operation time was 45 minutes in Group A and 48 minutes in Group B. The mean radiation exposure times were 4.2 minutes and 4.8 minutes, respectively. VAS scores were 0.7 points and 0.5 points in each respective group. In Group A, the VAS score was 1.7 points when we applied pressure on the skin around the plate. The mean Olerud and Molander Ankle Score was 87.4 points and 86.3 points, respectively. A superficial wound infection occurred in 1 case in each group, and angular deformities more than 5 degrees occurred in 2 Group B cases.
CONCLUSION
No significant differences in results were observed between the two groups. However, a higher incidence of angular deformity was seen in the intramedullary nailing group. Therefore, we must be careful during surgery. -
Citations
Citations to this article as recorded by- Comparative Analysis of Minimally Invasive Plate Osteosynthesis and Intramedullary Nailing in the Treatment of the Distal Tibia Fractures
Ho-Min Lee, Young-Sung Kim, Jong-Pil Kim, Phil-Hyun Chung, Suk Kang, Kaung Suk Jo
Journal of the Korean Fracture Society.2018; 31(3): 94. CrossRef - A Comparison of the Results between Intramedullary Nailing and Minimally Invasive Plate Osteosynthesis in Distal Tibia Fractures
Chul-Hyun Park, Chi-Bum Choi, Bum-Jin Shim, Dong-Chul Lee, Oog-Jin Shon
Journal of the Korean Orthopaedic Association.2014; 49(4): 285. CrossRef
- Comparative Analysis of Minimally Invasive Plate Osteosynthesis and Intramedullary Nailing in the Treatment of the Distal Tibia Fractures
- 811 View
- 0 Download
- 2 Crossref

- Analysis of Risk Factors for Nonunion after Intramedullary Nailing of Femoral Shaft Fracture in Adult
- Yong Woon Shin, Yerl Bo Sung, Jeong Yoon Choi, Minkyu Kim
- J Korean Fract Soc 2011;24(4):313-320. Published online October 31, 2011
- DOI: https://doi.org/10.12671/jkfs.2011.24.4.313
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To evaluate the union time and nonunion rate after intramedullary nailing of femoral shaft fracture in adult, we would like to analysis the operation techniques, comminution, contact surface and displacement.
MATERIALS AND METHODS
We reviewed retrospectively 53 patients undergoing femoral intramedullary nailing at least 2 years postoperatively and analysised the union time and nonunion rate by operation techniques, comminution, contact surface and displacement. Patients were operated by either antegrade or retrograde intramedullary nailing.
RESULTS
There were no differences in nonunion rate, the duration of bony union between antegrade and retrograde intramedullary nail groups. Significant differences were found in the duration of bony union between the Winquist and Hansen type I, II and the type III, IV (p<0.05). There were significant differences in the duration of bony union among simple, comminuted, and segmental fracture groups (p<0.05).
CONCLUSION
The union time is affected by not operation techniques and fracture displacement, but Winquist-Hansen classification and number of fracture fragments in intramedullary nailing of adult femoral shaft fracture. -
Citations
Citations to this article as recorded by- Extra-capsular proximal femoral fractures: a cohort comparison of union and complication rates after ballistic versus blunt trauma
Jordan Cook Serotte, Kevin Chen, Julia Nascimben, Jason Strelzow
European Journal of Orthopaedic Surgery & Traumatology.2025;[Epub] CrossRef - Factors Affecting Time to Bony Union of Femoral Subtrochanteric Fractures Treated with Intramedullary Devices
Jung-Yoon Choi, Yerl-Bo Sung, Jin-Hee Yoo, Sung-Jae Chung
Hip & Pelvis.2014; 26(2): 107. CrossRef - Augmentative Locking Plate Fixation for the Treatment of Femoral Nonunion after Intramedullary Nailing
Ki-Chul Park, Chul-Woong Kim, Kyu-Tae Hwang, Ye-Soo Park
Journal of the Korean Fracture Society.2013; 26(4): 268. CrossRef
- Extra-capsular proximal femoral fractures: a cohort comparison of union and complication rates after ballistic versus blunt trauma
- 1,186 View
- 7 Download
- 3 Crossref

- Intramedullary Nailing for Complex Fractures of the Proximal and Midshaft of the Humerus
- Chul Hyun Cho, Gu Hee Jung, Kyo Wook Kim
- J Korean Fract Soc 2011;24(3):237-242. Published online July 31, 2011
- DOI: https://doi.org/10.12671/jkfs.2011.24.3.237
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
To evaluate the results of antegrade interlocking intramedullary nailing for complex fractures of the proximal and midshaft of the humerus.
MATERIALS AND METHODS
We retrospectively analyzed the clinical and radiologic results in 11 cases, which were treated by antegrade interlocking intramedullary nail. We assessed clinical outcomes according to ASES scoring system and radiological result.
RESULTS
All cases had bony union and the mean union period was 14.7 weeks. Postoperative complications were 1 loss of fixation, 2 proximal protrusion of nail and 2 temporary shoulder pain. A case with loss of fixation was treated open reduction and refixation and had union at 14 weeks postoperatively. The mean ASES score was 85.9 and the clinical outcomes were 4 excellent, 5 good, 1 fair and 1 poor.
CONCLUSION
Intramedullary nailing for complex fractures of the proximal and midshaft of the humerus can offer a reliable treatment option.
- 526 View
- 0 Download

Case Report
- Lateral Positioning for Proximal Femoral Nailing of the Intertrochanteric Fracture: Surgical Technique
- Kwan Hee Lee, Hoon Jeong, Jong Kyoung Ha, Yong Ju Kim, Won Hee Jang
- J Korean Fract Soc 2011;24(1):79-82. Published online January 31, 2011
- DOI: https://doi.org/10.12671/jkfs.2011.24.1.79
-
 Abstract
Abstract
 PDF
PDF - In the treatment of intertrochanteric fractures, most of intramedullary nailings are performed on a fracture table in supine position. In supine position, however, soft tissue mass of the patients and drapes make it difficult to access to the piriformis fossa and to straighten the trajectory of reamer and nail insertion. To resolve these problems, we have treated twenty intertrochanteric fractures in lateral position on the general operation table with IM nail. Adjustment of the position of lag screw in femoral head was done with the technique that overlaps the shadows of the femoral head, nail and targeting guide in the lateral view. Because the entire injured limb can be moved readily, it was easy to reduce fracture and to convert to open procedure. In cases likely that the fracture table is unavailable in which patients are obese, have short stature or are amputated, and that open procedure is strongly likelihood, lateral position will be helpful technique in the treatment of intertrochanteric fractures with IM nail.
-
Citations
Citations to this article as recorded by- Outcomes of Internal Fixation with Compression Hip Screws in Lateral Decubitus Position for Treatment of Femoral Intertrochanteric Fractures
Cheon-Gon Park, Taek-Rim Yoon, Kyung-Soon Park
Hip & Pelvis.2018; 30(4): 254. CrossRef - The Effects of Sa-Am Spleen-tonifying Acupuncture on Radial Pulse in Healthy Human Subjects
Kwang Sik Yoon, Hyun Lee
The Acupuncture.2013; 30(4): 1. CrossRef
- Outcomes of Internal Fixation with Compression Hip Screws in Lateral Decubitus Position for Treatment of Femoral Intertrochanteric Fractures
- 1,812 View
- 57 Download
- 2 Crossref


 E-submission
E-submission KOTA
KOTA TOTA
TOTA TOTS
TOTS

 First
First Prev
Prev


