Abstract
Distal tibial metaphyseal fractures are commonly caused by high-energy injuries in young men and osteoporosis in older women. These fractures should be clearly distinguished from high-energy pilon fractures. Although the optimal surgical intervention methods for distal tibial metaphyseal fractures remain uncertain and challenging, surgical treatments for nonarticular distal tibia fractures can be broadly divided into two types: plate fixation and intramedullary nail (IMN) fixation. Once functional reduction is achieved using an appropriate technique, distal tibial nailing might be slightly superior to plate fixation in reducing postoperative complications. Thus, the surgical strategy should focus on functional realignment and proceed in the following sequence: (1) restoring the original tibial length, regardless of whether fibular fixation is to be done; (2) making the optimal entry point through an anteroposterior (AP) projection based on the overlapping point between the fibular tip and lateral plateau margin; (3) placing Kirschner wires (Ø2.4 mm) as blocking pins (in the AP orientation for coronal control and in the mediolateral [ML] orientation for sagittal control) as close to the upper locking hole as possible without causing further comminution on the concave aspect of the short fragment; and (4) making the the distal fixation construct with at least two ML and one AP interlocking screw or two ML interlocking screws and blocking screws. After the IMN is adequately locked, blocking pins (Ø2.4 mm) need to be replaced by a 3.5 mm screw.
-
Keywords: Tibia, Bone fracture, Intramedullary fracture fixation
Introduction
Distal tibial metaphyseal fractures are commonly caused by high-energy injuries in young men and to osteoporosis in older women. They should be clearly distinguished from high-energy pilon fractures since the metaphyseal including articular region is inevitably comminuted and impacted owing to axial loading. Currently, surgical treatments for nonarticular distal tibia fractures could be broadly divided into two types: plate fixation and intramedullary nail (IMN) fixation. Biological and biomechanical aspects, surgical equipment, and experience-based techniques should be considered when deciding on a surgical strategy. IMN causes less soft tissue damage, preserves more extraosseous blood supply, and facilitates earlier union and weight-bearing. However, anterior knee pain and surgical technique-related malunion are significant concerns. Plate fixation through limited open reduction or minimally invasive percutaneous plate osteosynthesis employs an indirect bridge reduction technique and causes less damage to blood supply. However, compared with IMN, Plate fixation has a large wound exposure and soft tissue dissection, leading to higher risks of wound complications and delayed union. Ekman et al. [
1] have recently performed a systemic review and meta-analysis and concluded that IMN fixation might be slightly superior to plate fixation in reducing postoperative complications, although their functional outcomes are similar. Li et al. [
2] have also conducted a meta-analysis of randomized controlled trials to compare efficacies of these two surgical modalities and reported that IMN fixation might be preferred over plate fixation since IMN fixation confers more advantages of reduced surgical time, radiation time, weight-bearing time, and wound complications. Thus, optimal surgical intervention methods for distal tibial metaphyseal fractures remain uncertain and challenging.
Considering that elevated rates of malunion after IMN fixation require attention [
1,
3], achieving superior outcomes from distal tibial nailing requires a clear understanding of fracture characteristics, biomechanics of IMN, and technical differences from conventional nailing. Therefore, this study aims to describe how to obtain desired results from distal tibial nailing.
Written informed consent was obtained from the patients for publication of their images in this review.
Anatomy and Fracture Characteristics for Distal Tibial Nailing
Concerning fracture fixation, plain radiographs, computed tomography, and image intensifier without projection errors play a very important role in accurate evaluation of fracture characteristics and technical errors [
4]. With recent advancement of imaging technology, 3-dimensional (3D) rendering software capable of virtual fixation at actual size has been developed and used to verify practical implications of computational anatomy [
4,
5]. From diaphysis to distal metaphysis, the tibial shaft transitions from a triangular shape to a rounded shape. Because the anterior border of the diaphysis is twisted anteromedially from the diaphysis to the distal metaphysis, the twisted tibia on its longitudinal axis can produce a change in the alignment of planes of motion of proximal and distal articulations [
6]. Recently, Yang et al. [
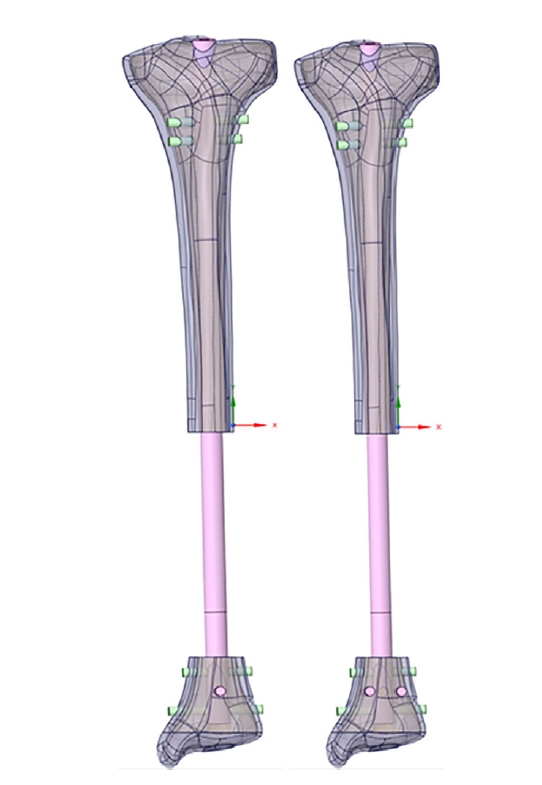
7] have enrolled 77 patients (51 males and 26 females) with a mean age of 47.9 years and measured distal tibia torsion (DTA) of 3D tibia models at actual size using the 3D-Matics software which could convert 3D models into 2D axial models to eliminate projection error of tibial (
Fig. 1). The distal tibia torsion had an average value of 30.06° (range, 12.74°–48.76°; standard deviation [SD], 6.50°). Thus, the fibula is situated posterolateral to the tibia and distally. It articulates with a shallow facet on the lateral surface of the distal tibial metaphysis (fibular notch).
As is already well known, the distal tibial metaphysis is done by constructing a square with the side length defined by the broadest portion of the tibial plafond [
8]. Fractures within 4 cm of the tibial plafond are distal metaphyseal injuries and nonarticular fractures are defined as those with no extension or with simple extension [
8]. Despite a relatively small region of tibia, distal tibia fracture could be classified as distal shaft fracture, distal metaphyseal fracture, distal articular fracture based on the fracture site and anatomic features. Furthermore, considering the injury mechanism, a distal articular fracture should be discriminated from a pilon fracture which involves distal articular surface with metaphyseal comminution due to a high-energy axial loading, and generally, distal tibia fractures are usually caused by the shearing force or rotational injury of slip-down, with most of them not having extensive metaphyseal comminution or axillary unstable fracture (length-unstable pattern) (
Fig. 2). When deciding surgical methods, fracture characteristics of length-stable or length-unstable patterns should be preoperatively verified because restoration and maintenance of original tibia length are prerequisites for achieving functional reduction and desired results.
Surgical Strategy for Distal Tibial Nailing
Fixing the fibula or not during distal tibial nailing
Although the necessity of fibular fixation remains controversial, before a nailing procedure, surgeons should restore and maintain the original tibia length without performing manual traction. Concerning the original tibia length, an intact fibula or anatomically fixed fibula could be used as an indicator, especially for comminuted fractures without special equipment or additional procedures. Fibular fixation is related to a better anatomical alignment and better control over rotation [
3]. Additionally, significantly higher rates of loss of reduction in distal tibia nailing without fibular plate fixation have been reported [
3,
9]. Even if the role of the fibula in weight-bearing could be considered, the fibular fixation may result in delayed union or nonunion because it can inhibit cyclic loading on the fracture site [
3]. When performing distal tibial nailing, surgeons should consider the indication of fibular fixation and fixation method to improve rotational alignment of the leg, restore the original tibia length, achieve functional reduction, and allow controlled impaction.
Concerning the indication of fibular fixation in the distal tibial nailing, fracture morphologies of the tibia should be clarified first. In the case of a simple or wedge fracture where there is contact between proximal and distal fragments, once the fracture is reduced, the fibular fixation does not necessarily have to be performed. However, if the distal tibial fracture has a length-unstable type of comminution, the fibular fracture should be fixed first to restore the original tibia length. Concerning the fixation method of a comminuted or wedge fibular fracture, the distractive bridge plating technique can be considered [
10]. A distractive force could be easily applied with a laminar spreader similar to a large distractor used for lower limb fractures (
Fig. 3). Through this distractive procedure, surgeons could actively control the fibular length based on the dime sign with soft tissue preservation. After the length is restored, screw fixations of both fibular fragments should be performed partially to maintain the slightly flexible tibia because fracture reduction of the distal tibia needs intraoperative adjustments using manual manipulation, blocking pins, or several instruments (
Fig. 4).
Traditional incision point for IMN is made with an infra-patellar approach. However, it is challenged by a high incidence of postoperative complications such as anterior knee pain [
11]. A para- and supra-patellar approach has been introduced as an alternative surgical approach, which has an advantage because the procedure is performed at a knee flexion of approximately 20° with fluoroscopic visualization. In addition, fracture manipulation is intraoperatively easier to obtain [
11]. Another potential advantage is that the rotational alignment of proximal tibiofibular joint can be verified more easily without a positional change of leg or an image intensifier. Concerning the optimal entry point, several studies [
5,
12,
13] have shown that the ideal starting point of the safety zone is located at the anterior edge of the tibial plateau, just medial to the lateral tibial spine from a true anteroposterior (AP) radiograph. Walker et al. [
14] and Byun and Jung [
5] have emphasized that the entry point could be varied radiographically according to tibial rotation. Thus, a radiologic landmark with consistency might be used intraoperatively. Through cadaveric study, Walker et al. [
14] have demonstrated fluoroscopic movement of entry point according to tibial ration. The entry point moves laterally along the plateau with an external rotation of tibia and medially with an internal rotation. They emphasized that the relative external rotation of the tibia could lead to medial insertion points when using the lateral tibial spine as a landmark [
14]. They have introduced fluoroscopic landmarks which could be used without special equipment or additional procedures. A neutral AP to determine the starting point should be obtained by ensuring that the fibula is bisected by the lateral margin of tibial plateau [
14]. Recently, authors of this study have also performed a computational simulation study using the Mimics software (Materialise Interactive Medical Image Control System; Materialise) and introduced a fluoroscopic landmark by analyzing a 3D tibia model at actual size [
5]. Instead of using an imaginary fibular bisecting line, we suggested an overlapping point between lateral margin of tibial plateau and fibular tip (
Fig. 5). When the overlapping point was placed just around fibular tip, the guide wire was almost aligned in a straight line and could be used as neutral AP projection to verify the optimal entry point [
5]. Among 104 models of tibia and fibula, the overlapping point was just lateral to the fibular tip in 62 models. For 42 models, it exactly matches the fibular tip. There was no significant difference according to the height of cadaver (P=0.0832) [
5]. Therefore, the overlapping point is useful as a practical landmark for making neutral AP projection to determine the optimal entry point without additional procedures or equipment (
Fig. 6).
Despite the widespread use of distal tibial nailing with newer nailing systems, surgeons still face many difficulties and pitfalls of intraoperative fracture reduction. Besides, clear indications of several reduction techniques and instruments remain unavailable. Considering that malalignment occurs with a relatively high frequency compared with plate osteosynthesis [
1,
3], functional reduction through a closed method will be an essential part of distal tibial nailing. As mentioned above, although fibular fixation is not perfect, it can achieve better anatomical alignment and better control over rotation of distal tibia [
3]. For further reduction of distal tibia, several options might be utilized according to the surgeon’s preference, including facilitation with manual manipulation, clamps, and universal distractors. To achieve functional realignment, the original tibial length should be maintained before the nailing procedure without manual traction or manipulation because the AP angulation or varus/valgus could be correctable based on the author’s experience (
Fig. 7). To optimize reduction adequacy of distal tibia, authors prefer the use of Kirschner wires (Ø2.4 mm) first as blocking pin instead of 3.5 mm screws. Manual manipulation inevitably increases radiation exposure to the surgeon and operating room personnels during nail insertion. Compared to other techniques, blocking pins are technically simple, practical, and reproducible without requiring special instruments or hardware [
15]. Blocking pins can be used to create a corridor and effectively reduce the width of the metaphyseal region during nail insertion. They also have an advantage of being easily adjusted by changing their positions. Furthermore, after adequately locking the IMN, the pin can be removed, and a 3.5 mm screw can be fixed in its place without requiring additional procedures (
Fig. 8). Overall, blocking pins were used as a reduction tool for guiding the pathway of IMN and facilitating more accurate fracture reduction.
Carefully analyzing preoperative and intraoperative imaging with traction is essential for identifying where blocking pins should be placed. Conventional placement of blocking pins based on previously published principles can be used in shorter, displaced mobile fragments to achieve reduction [
15,
16]. For coronal control of distal fragment, the blocking pin should be placed AP (and mediolateral for sagittal control) as close to the fracture line as possible without causing further comminution. However, based on the author’s experience, Kirschner wires (Ø2.4 mm) can be placed on the concave aspect of the short fragment, just superior to the 1st interlocking hole to mimic and increase the area of isthmic cortical contact. They can then be replaced with a 3.5 mm screw after nail insertion.
Traditionally, it is well known that IMN fixation provides load sharing characteristics and confers relative stability at the fracture site. The degree of stability is influenced significantly by the chosen IMN, its rigidity, and interlocking screw options. Conventional nailing for midshaft fracture aims to increase isthmic cortical contact through intraoperative technical considerations of reaming procedure and IMN as large as possible (
Fig. 9). Concerning distal tibial nailing, however, the elastic energy of IMN built under the tension of blocking screws contributes to long-term compression and improvement in fracture reduction over time (
Fig. 10) [
17]. Tennyson et al. [
17] have reported that an IMN of Ø10 mm cannot harness the full benefit of blocking screws and that deflection of the IMN is essential for generating further stability. Thus, when performing distal tibial nailing, a fully tight nail is not necessarily required. It is more advantageous to use smaller nails than conventional nails since nail deflection around a blocking screw could increase long-term compression (
Fig. 10). Furthermore, smaller nails can help create more space for blocking screws.
Biomechanics of Distal Interlocking Screws and Blocking Screws
Currently, there is a paucity of research focusing on improving the construction stability of distal tibial fragments. Although a biomechanical model does not consider progressive healing of fracture, which will inevitably contribute to fracture stability further, Lowenberg et al. [
18] have biomechanically demonstrated that at least two distal and one proximal interlocking screws are recommended to resist torsional loading of distal tibia fractures. The addition of a third distal interlock did not only provide any meaningful additional stability, but the orientation of the distal interlocks (medial to lateral versus anterior to posterior) did not influence stability [
18]. However, it has been widely accepted that two distal interlocking screws of distal tibial nailing can provide inadequate stability in compression/bending despite adequate axial/torsional stiffness in a distal tibia fracture gap model [
15,
19].
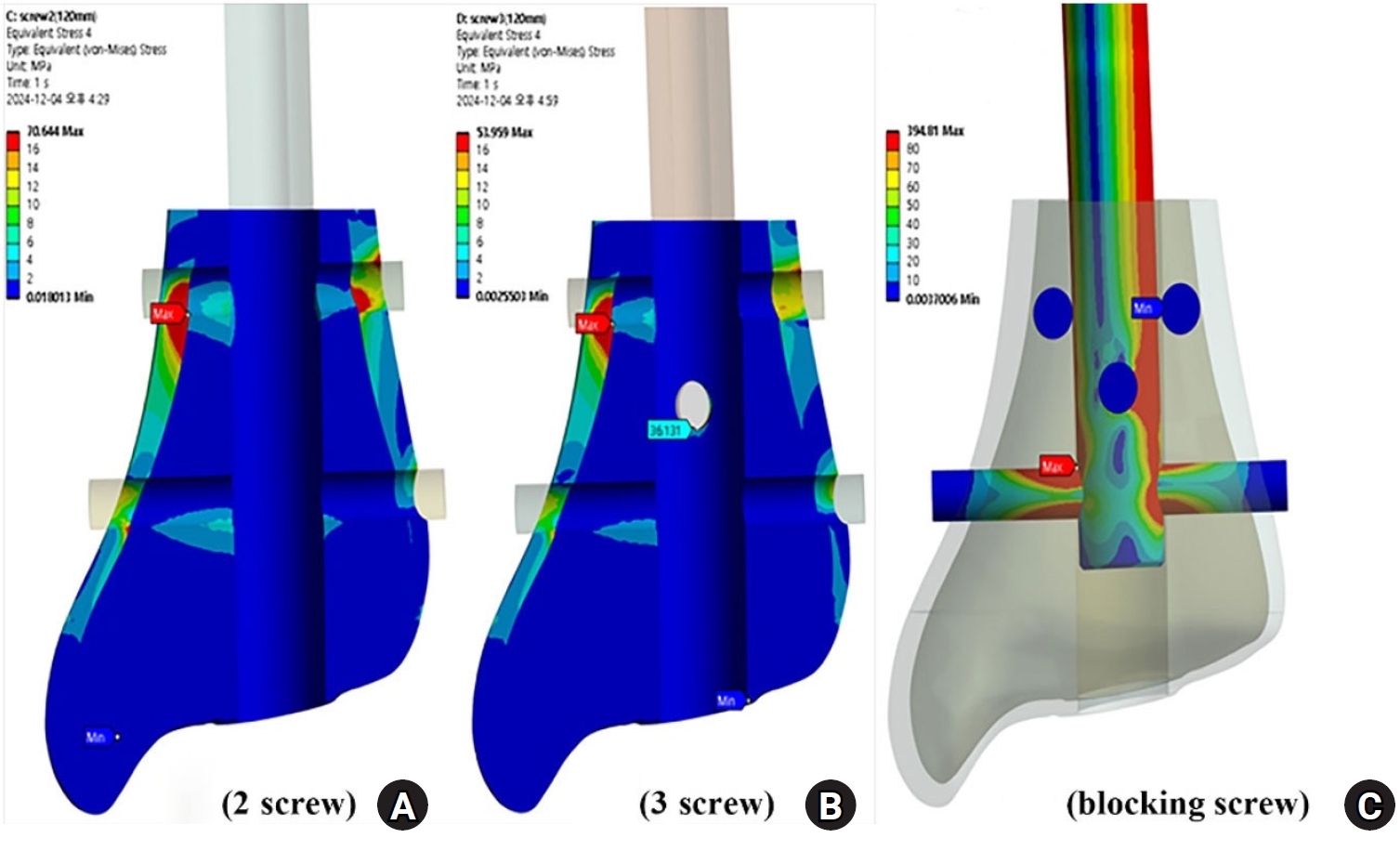
A fixation construct of distal fragment should be focused on increasing angular resistance. Theoretically, a single bicortical interlocking screw can create three points of distal fixation and improve construct stiffness while reducing interfragmentary motion. The interlocking screw should purchase the near and opposite cortex with sufficient length because the threads and diameter of screw tip is so different. Through our experiments using a finite element method with Ansys ver. 19.0 (Ansys Inc.), stress distribution areas of distal tibia had maximum values at the medial cortex around the upper interlocking screw. When a blocking screw model was compared with a three-screw model, the maximal von Mises stress value of implant was decreased in the 1st interlocking screw hole and increased in the 2nd interlocking screw hole. Regarding stress distributions for distal fixation construct, the maximum values were found at the upper hole of the interlocking screw (
Fig. 11). Thus, the upper interlocking screw of the distal tibia should be placed to achieve complete cortical contact at the opposite cortex by an over-length of 3–4 mm.
Preferred Indications and Practical Technique
For the past 15 years or more, the authors have preferred distal tibial nailing based on evolved indication and techniques. When deciding on a surgical method, first, the following absolute contraindications of distal tibial nailing should be verified (1) articular fracture should be reconstructed or repaired through open approach, (2) short-sized distal fragment could not be secured by two AP interlocking screws (
Fig. 12), and (3) there was significant deformity or obliteration of medullary canal. After confirming these, we can plan how to perform distal tibial nailing. In case of a simple distal articular fracture, the compression screw should be placed, taking into account the interlocking screw position before nailing procedure. If fibular fracture is a simple/wedge or spiral fracture and the tibial fracture is not a comminuted/length-stable type, the guide wire insertion through optimal entry point could be performed without fibular fixation. However, when the tibia fracture is comminuted and length-unstable, the fibula should be anatomically restored for achieving the original tibial length and rotational realignment. Concerning the fixation technique, the distractive technique for restoring the fibular length is used more often than expected. After the length is restored, screw fixations of both fragments should be performed partially rather than definitively because fracture reduction of distal tibia needs intraoperative adjustments using manual manipulation, blocking pins, and/or several instruments. Regardless of a para- or supra-patellar approach, the optimal entry point is made based on the neutral AP which suggested the overlapping point between the lateral margin of tibial plateau and fibular tip was placed just around the proximal portion of the fibular tip. For optimizing the reduction adequacy except tibial length, Kirschner wires (Ø2.4 mm) can be placed to create a corridor and effectively reduce the width of the metaphyseal region just superior to the upper interlocking hole while avoiding further comminution around the fracture. The blocking pin might be placed on the concave aspect of the short fragment to prevent the nail from shifting (
Fig. 13). The distal fixation construct should be made with at least two mediolateral (ML) and one AP interlocking screw or two ML interlocking screws and blocking screws. The interlocking and blocking screws should be placed to achieve complete cortical contact at the opposite cortex. After the IMN is adequately locked, blocking pins (Ø2.4 mm) should be replaced with a 3.5 mm screw.
However, the risk of radiation exposure will inevitably increase with additional procedures of blocking pin placement. It is known that radiation exposure poses a risk to orthopedic surgeons, with a relative risk of cancer being 5.37 times greater compared with the general population [
20,
21]. Authors previously clearly demonstrated that the intraoperative radiation emission and exposure by an image intensifier could be appreciably reduced by the surgeon’s awareness of radiation hazards and clear strategies in reducing radiation exposure: (1) use the pulsed fluoroscopy, not the continued fluoroscopy, (2) use the mark-pen and temporary K-wire fixation whenever possible, (3) retrieve the intraoperative radiation emission data from fluoroscopy machine as often as necessary [
20,
22].
Conclusions
If functional reduction is achieved based on an appropriate surgical technique, distal tibial nailing might be slightly superior to plate fixation in reducing postoperative complications. Thus, surgical strategy for functional realignment is the prerequisite for optimizing distal tibial nailing to obtain desired results. To achieve the reduction adequacy of distal tibia, it is recommended that the blocking pin (Ø2.4 mm) be used first instead of 3.5 mm screws because of simple, practical, and reproducible technique without requiring special instruments or hardware.
Once the original tibial length is secured, functional reduction could be easily achieved by making the optimal entry point through neutral AP projection and by using blocking pins for coronal/sagittal control on the concave aspect of a short fragment. The distal fixation construct should be made with at least two ML and one AP interlocking screw or two ML interlocking screws and two blocking screws. The interlocking and blocking screws should be placed to achieve complete cortical contact at the opposite cortex. In the future, clinical and biomechanical studies on the optimal combination and location of interlocking screws and blocking screws are considered necessary.
Article Information
-
Author contributions
Conceptualization: GHJ. Data curation: JTA. Investigation: SLJ. Writing-original draft: JTA, GHJ. Writing-review & editing: GHJ, SLJ. All authors read and approved the final manuscript.
-
Conflict of interests
None.
-
Funding
This work was supported by the Korea Medical Device Development Fund grant funded by the Korea government (the Ministry of Science and ICT, the Ministry of Trade, Industry and Energy, the Ministry of Health & Welfare, the Ministry of Food and Drug Safety) (project No. RS-2022-0164554).
-
Data availability
Not applicable.
Fig. 1.Distal tibial torsion of a 3-dimensional (D) model at actual size is measured using the 3D-Matics software, which converts 3D distal models into 2D axial models to eliminate projection errors.
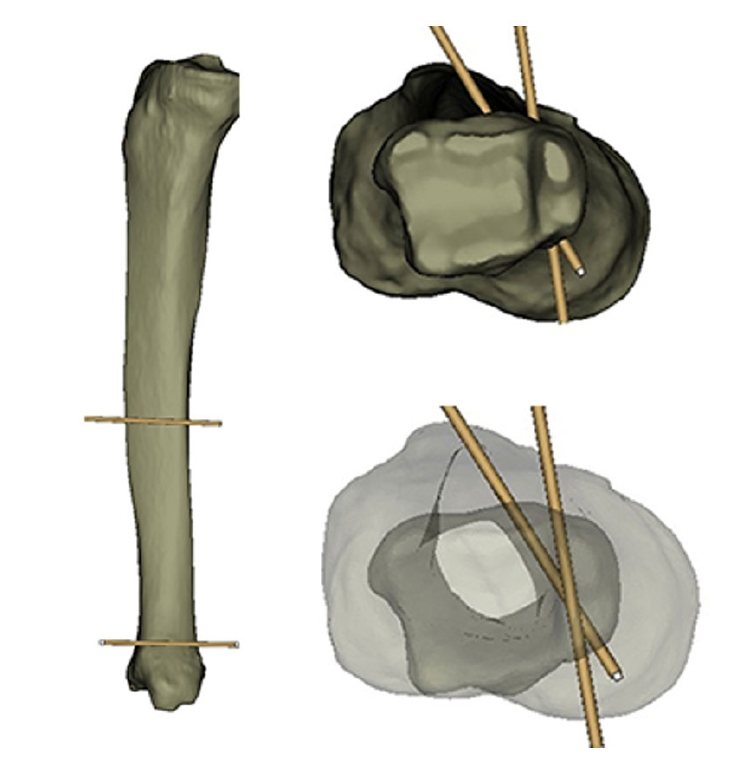
Fig. 2.(A) Distal tibial (metaphyseal) fractures should be clearly distinguished from high-energy pilon fractures. (B, C) Despite involving a relatively small region of the tibia, distal tibial fractures can be classified as distal metaphyseal fractures, distal shaft fractures, and distal articular fractures based on the fracture site and anatomic features.

Fig. 3.(A) A distal tibiofibular fracture with comminution, shortening, and angulation in a 58-year-old male patient. (B) The distal fragment of the fibular fracture is fixed with a one-third tubular plate. (C–E) A distractive force is applied using a laminar spreader to restore the original fibular length, and the proximal fragment is then fixed. (F) An external fixator is applied for a staged operation.
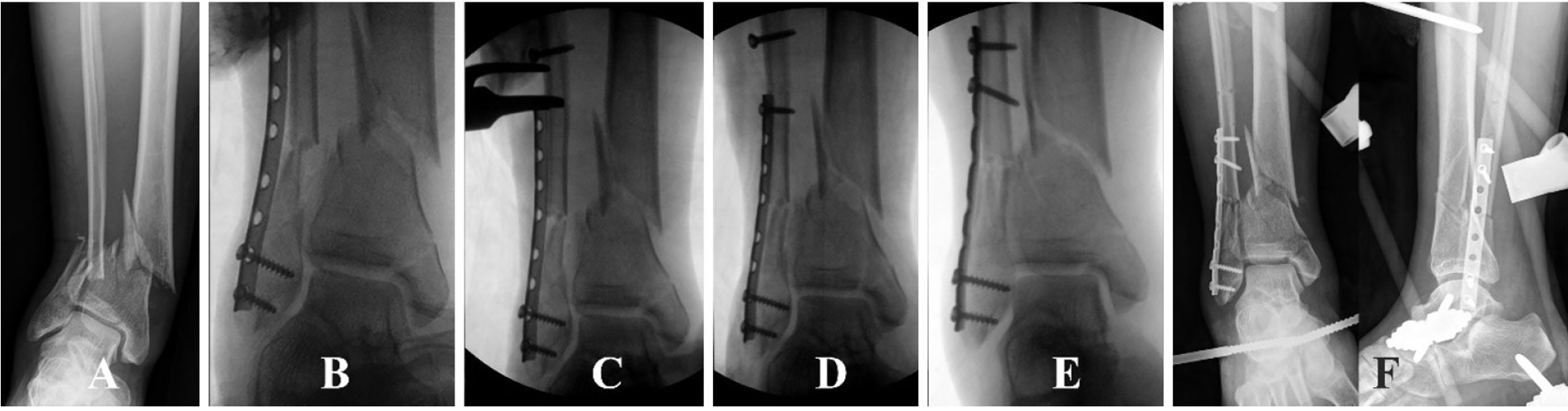
Fig. 4.(A) A distal tibiofibular fracture with comminution, shortening, and angulation in a 47-year-old female patient. (B) The fibular fracture is preferentially fixed by restoring the original length. (C, D) After achieving functional reduction of the tibia, blocking pins are placed to make the optimal nail path through a para-patellar approach. (E–G) The distal tibia fracture is healed with functional realignment and good clinical function.
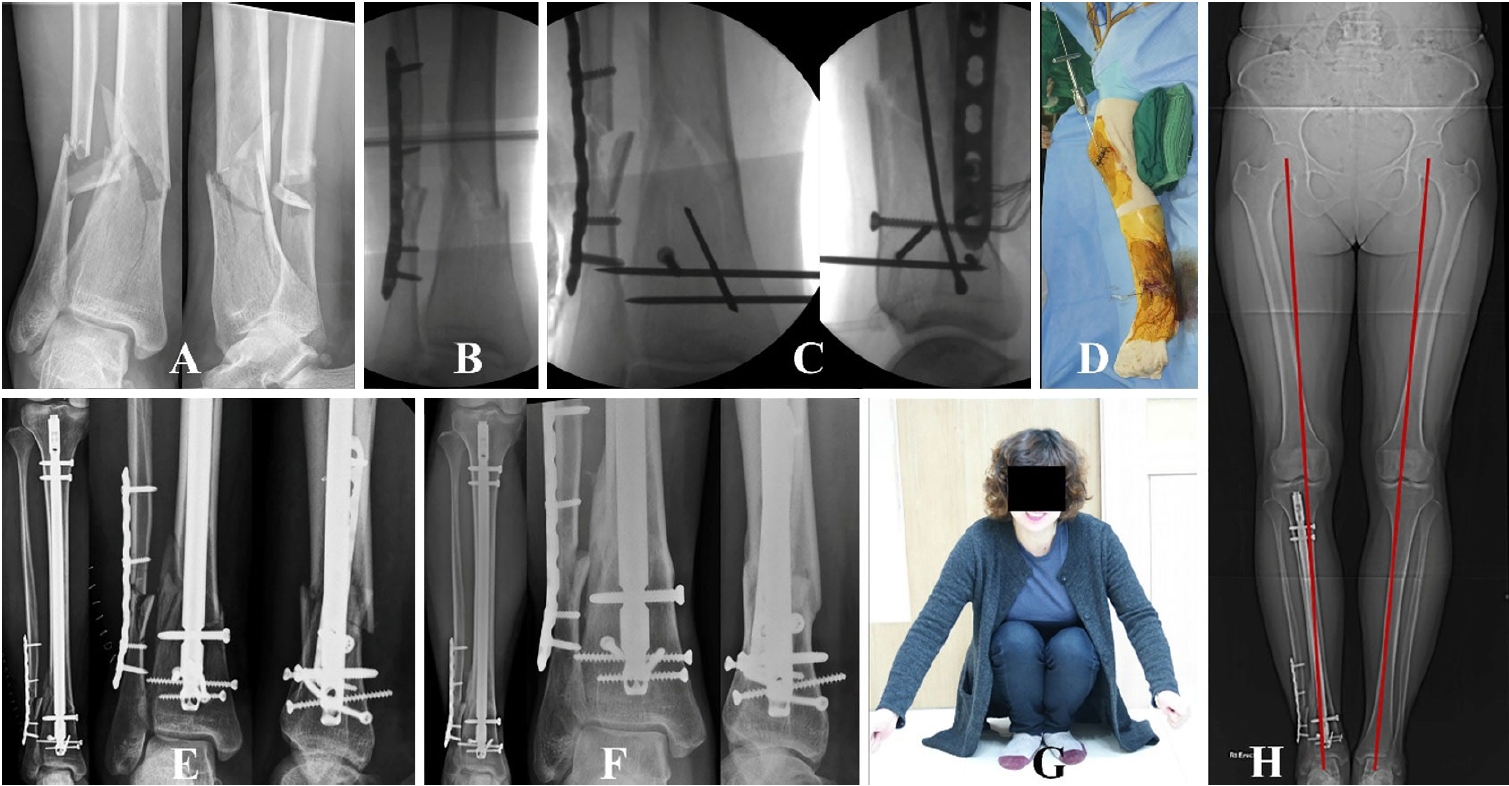
Fig. 5.(A) When the overlapping point between the lateral margin of the tibial plateau and the fibular tip is placed just around the fibular tip, the guide wire is almost aligned in a straight line. This can be used as a neutral anteroposterior projection to verify the optimal entry point. (B, C) The optimal entry point appears medially or laterally translated if the overlapping point is not matched.
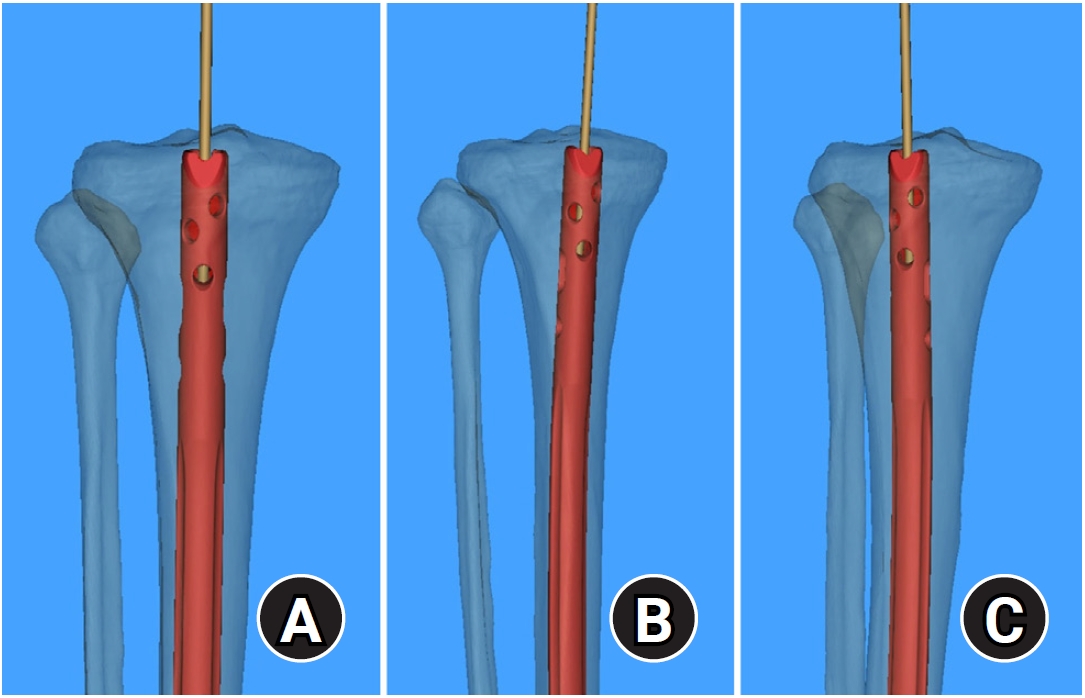
Fig. 6.The overlapping point can be used as a fluoroscopic landmark to create a neutral anteroposterior projection for determining the optimal entry point during nail insertion.

Fig. 7.(A) A distal tibiofibular fracture without comminution in a 53-year-old female patient. (B) An external fixator is applied without fibular fixation. (C) The fracture is manually manipulated to insert the guide wire without a blocking pin or fibular fixation. (D) The nail is placed eccentrically in the distal tibia. (E, F) The fracture, fixed with an intramedullary nail, is angulated posteriorly without achieving functional reduction.

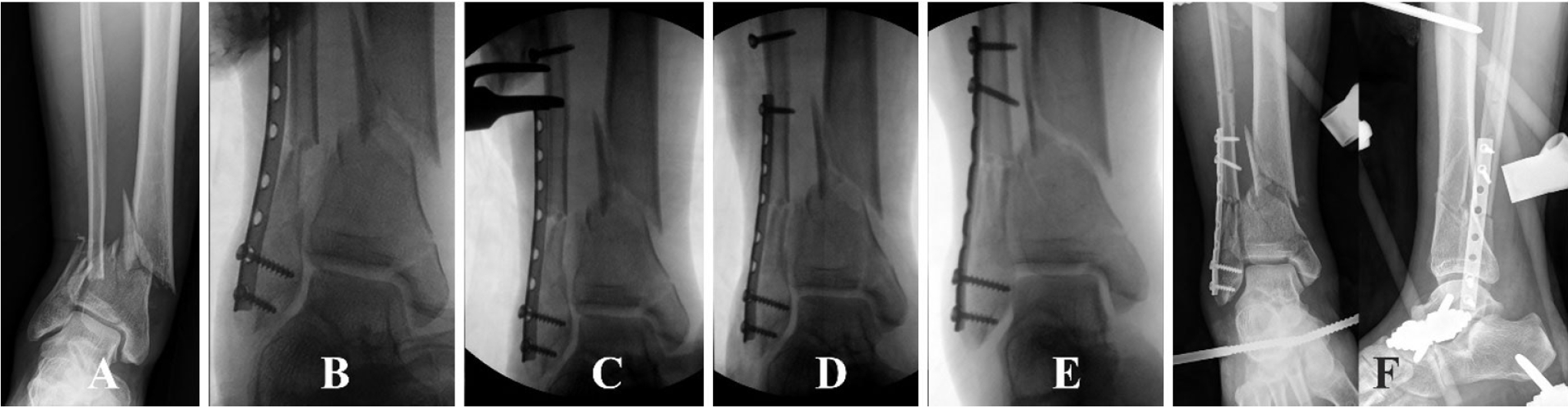
Fig. 8.(A) A distal tibial fracture with a segmented fibular fracture in a 51-year-old male patient. (B) The fibular fracture is preferentially fixed, but the original length is not restored. (C) For a staged operation, an external fixator is applied. (D) The fibular fracture is revised to restore the original length. (E, F) A Ø2.4 mm locking pin is placed for coronal control of the distal fragment. The fibular fracture is then definitively fixed. (G–I) After nail insertion, functional realignment of the distal tibial fracture is achieved, and the fracture unites completely.
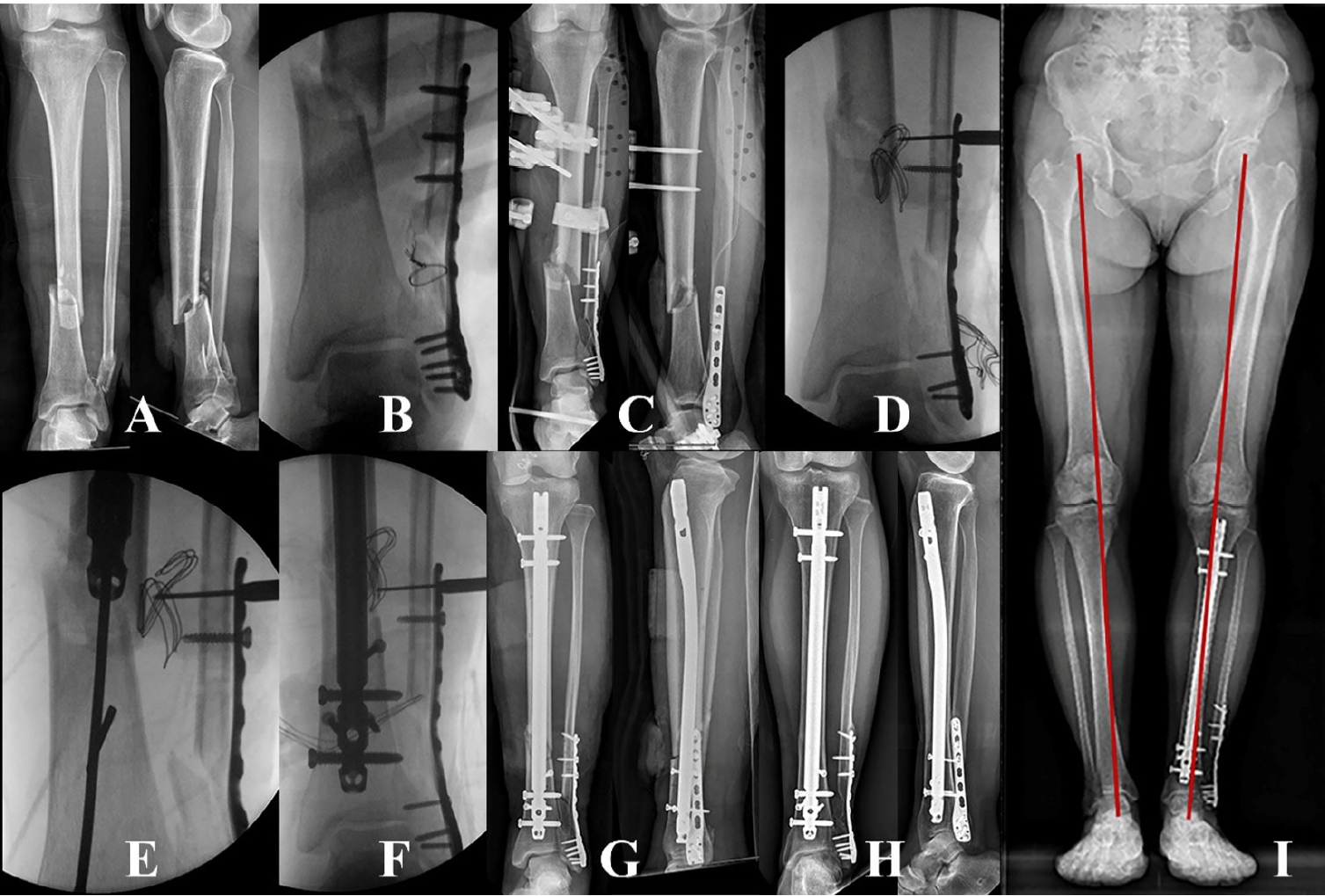
Fig. 9.The area of isthmic cortical contact is located in the mid-shaft area in conventional nailing. This area can be increased with a reaming procedure.

Fig. 10.The finite element method demonstrates the elastic energy of an intramedullary nail under the tension of blocking screws.

Fig. 11.(A, B) Stress distribution areas of the distal tibia show maximum values at the medial cortex around the first interlocking screw. (C) Stress distributions for the distal fixation construct show nail deflection and a maximal value around the distal interlocking hole.
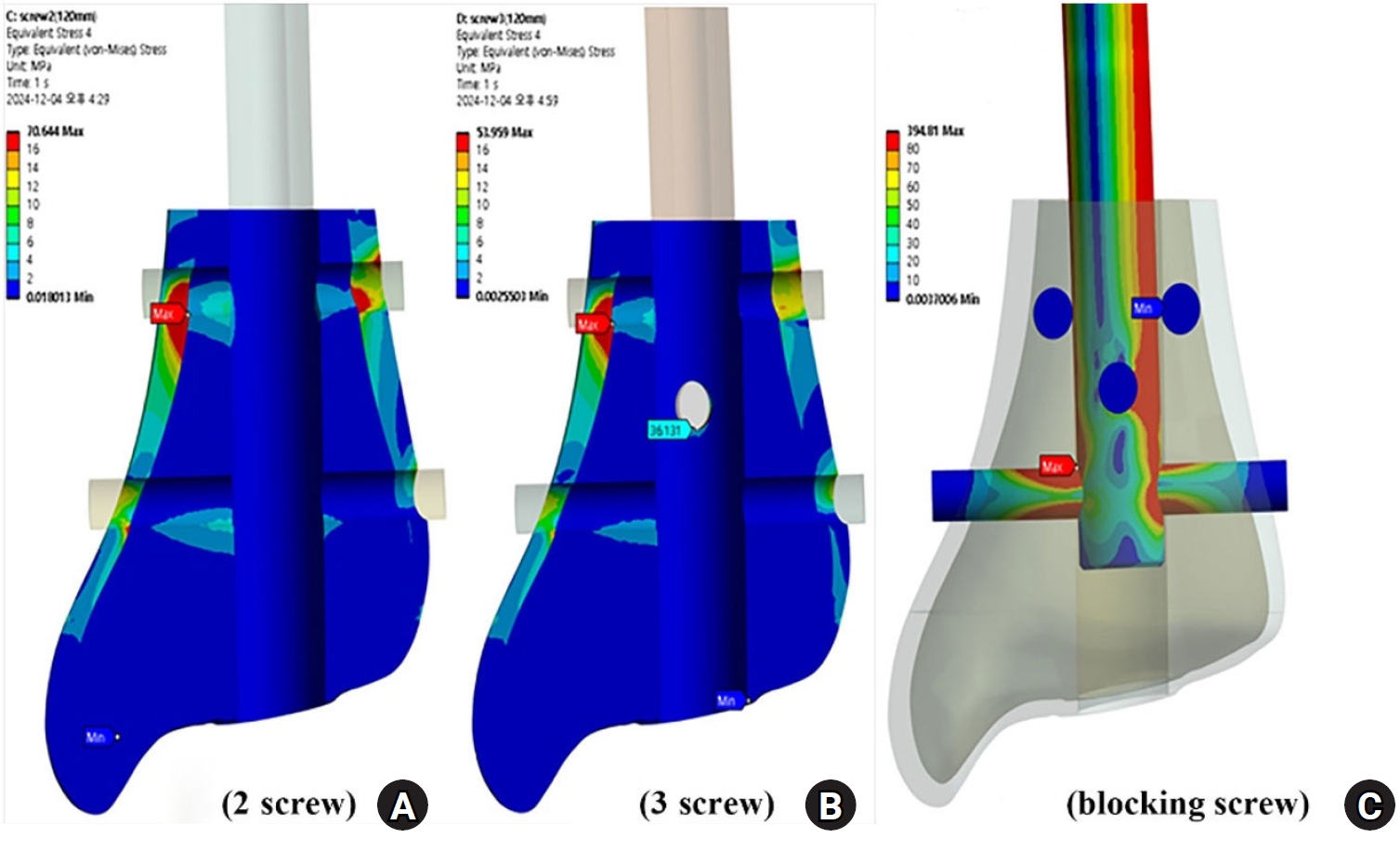
Fig. 12.For distal tibial nailing, a short-sized distal fragment should be secured by at least two anteroposterior interlocking screws.
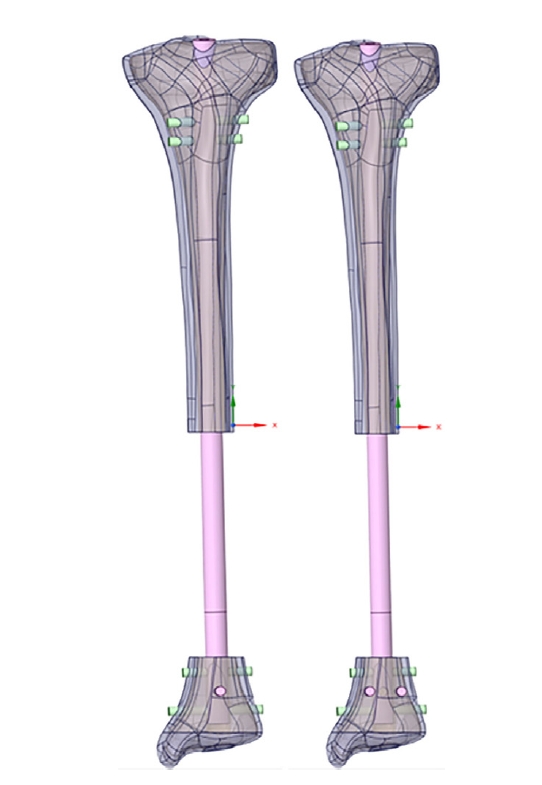
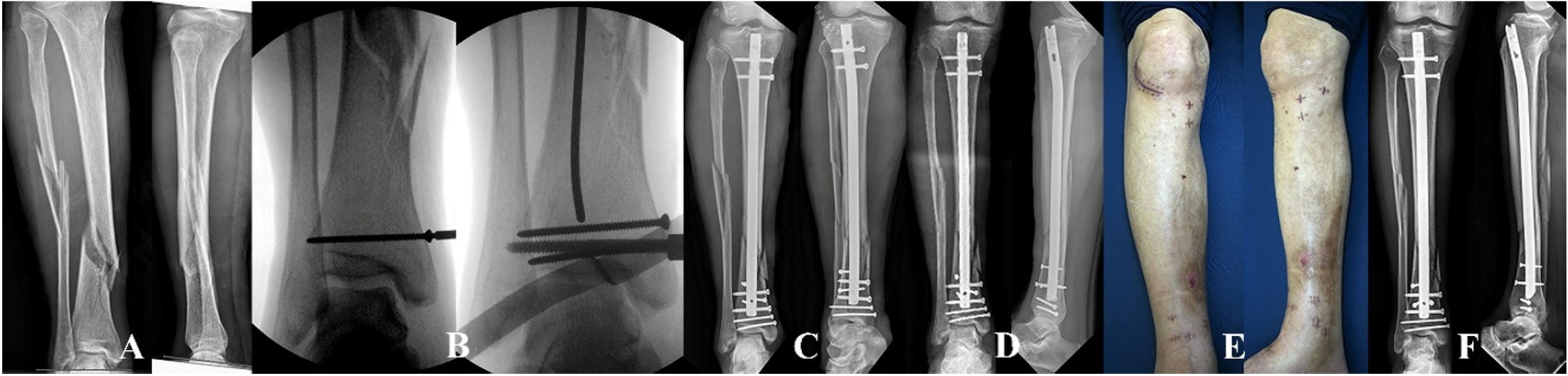
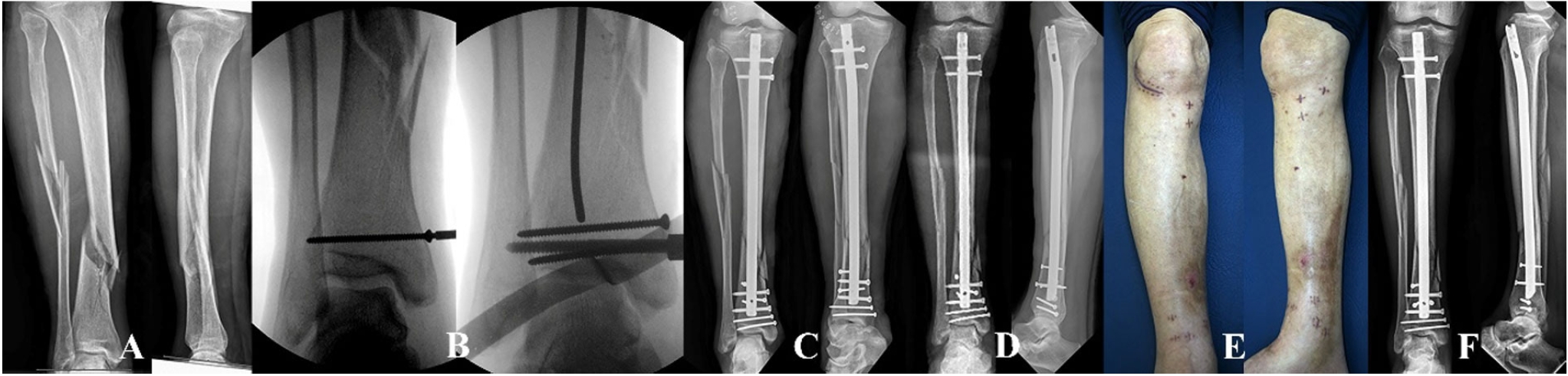
Fig. 13.(A) A distal tibial fracture with a comminuted fibular fracture in a 63-year-old male patient. (B) The distal articular fracture is preferentially fixed using a screw, and the guide wire is inserted through a para-patellar approach. (C–F) The distal fragment is secured by two mediolateral interlocking screws and blocking screws without iatrogenic comminution. After nail insertion, functional realignment is restored without soft tissue complications.
References
- 1. Ekman E, Lehtimaki K, Syvanen J, Saltychev M. Comparison between nailing and plating in the treatment of distal tibial fractures: a meta-analysis. Scand J Surg 2021;110:115-22.ArticlePubMedPDF
- 2. Lv C, Jiang C, Lv W, Zhang S, Li C. Effect of intramedullary nail fixation and internal plate fixation in distal tibia fracture surgery on post‐operative wound infection in patients: a meta‐analysis. Int Wound J 2023;21:e14383. PubMedPMC
- 3. Li C, Li Z, Wang Q, Shi L, Gao F, Sun W. The role of fibular fixation in distal tibia-fibula fractures: a meta-analysis. Adv Orthop 2021;2021:6668467.ArticlePubMedPMCPDF
- 4. Kim JY, Kang DG, Jung GH. Clinical research through computational anatomy and virtual fixation. J Korean Orthop Assoc 2023;58:299-310.ArticlePDF
- 5. Byun SE, Jung GH. Implications of three-dimensional modeling of tibia for intramedullary nail fixation: a virtual study on Asian cadaver tibia. Injury 2020;51:505-9.ArticlePubMed
- 6. Snow M. Tibial torsion and patellofemoral pain and instability in the adult population: current concept review. Curr Rev Musculoskelet Med 2021;14:67-75.ArticlePubMedPMCPDF
- 7. Yang SH, Lee JY, Jung GH, Kim HT, Ko BW. Biomechanical investigation to establish stable fixation strategies for distal tibial fractures in various situations: finite element analysis studies. J Korean Fract Soc 2024;37:71-81.ArticlePDF
- 8. Bedi A, Le TT, Karunakar MA. Surgical treatment of nonarticular distal tibia fractures. J Am Acad Orthop Surg 2006;14:406-16.ArticlePubMed
- 9. De Giacomo AF, Tornetta P 3rd. Alignment after intramedullary nailing of distal tibia fractures without fibula fixation. J Orthop Trauma 2016;30:561-7.ArticlePubMed
- 10. Jung GH, Cho CH, Kim JD. Distractive bridge plating in metaphyseal comminuted fractures of the distal radius through a pronator sparing approach. Eur J Orthop Surg Traumatol 2012;22:613-9.ArticlePDF
- 11. Wang Z, Xiong X, Lu Z, Gao Y. A systematic review and meta-analysis comparing suprapatellar versus infrapatellar approach intramedullary nailing for tibal shaft fractures. Eur J Trauma Emerg Surg 2024;50:383-94.ArticlePubMedPDF
- 12. Eastman J, Tseng S, Lo E, Li CS, Yoo B, Lee M. a cadaveric assessment. J Orthop Trauma 2010;24:672-6.PubMed
- 13. Kubiak EN, Widmer BJ, Horwitz DS. Extra-articular technique for semiextended tibial nailing. J Orthop Trauma 2010;24:704-8.ArticlePubMed
- 14. Walker RM, Zdero R, McKee MD, Waddell JP, Schemitsch EH. Ideal tibial intramedullary nail insertion point varies with tibial rotation. J Orthop Trauma 2011;25:726-30.ArticlePubMed
- 15. Zhou AK, Jou E, Lu V, Zhang J, Chabra S, Krkovic M. The evolution of poller screws. EFORT Open Rev 2024;9:252-63.ArticlePubMedPMC
- 16. Stedtfeld HW, Mittlmeier T, Landgraf P, Ewert A. The logic and clinical applications of blocking screws. J Bone Joint Surg Am 2004;86A Suppl 2:17-25.Article
- 17. Tennyson M, Krkovic M, Fortune M, Abdulkarim A. Systematic review on the outcomes of poller screw augmentation in intramedullary nailing of long bone fracture. EFORT Open Rev 2020;5:189-203.ArticlePubMedPMCPDF
- 18. Lowenberg DW, DeBaun MR, Behn A, Sox-Harris A. Interlocking screw configuration influences distal tibial fracture stability in torsional loading after intramedullary nailing. Eur J Orthop Surg Traumatol 2020;30:1205-13.ArticlePubMedPDF
- 19. Gorczyca JT, McKale J, Pugh K, Pienkowski D. Modified tibial nails for treating distal tibia fractures. J Orthop Trauma 2002;16:18-22.ArticlePubMed
- 20. Kwak JM, Heo SK, Jung GH. Simple way to reduce radiation exposure in the orthopaedic operating theater: an 18-month prospective study. Med Case Rep J 2018;1:111.
- 21. Zabel EW, Alexander BH, Mongin SJ, et al. Thyroid cancer and employment as a radiologic technologist. Int J Cancer 2006;119:1940-5.ArticlePubMed
- 22. Jung GH, Jang JH, Kim JD, Kim CK. Radiation exposure over the course of a year from an image intensifier in the orthopaedic operating room. J Korean Fract Soc 2012;25:58-63.Article
 , Se-Lin Jeong, BS2
, Se-Lin Jeong, BS2 , Gu-Hee Jung, MD, PhD1,2
, Gu-Hee Jung, MD, PhD1,2
























 E-submission
E-submission KOTA
KOTA TOTA
TOTA TOTS
TOTS
 ePub Link
ePub Link Cite
Cite

