Search
- Page Path
- HOME > Search
Review Articles
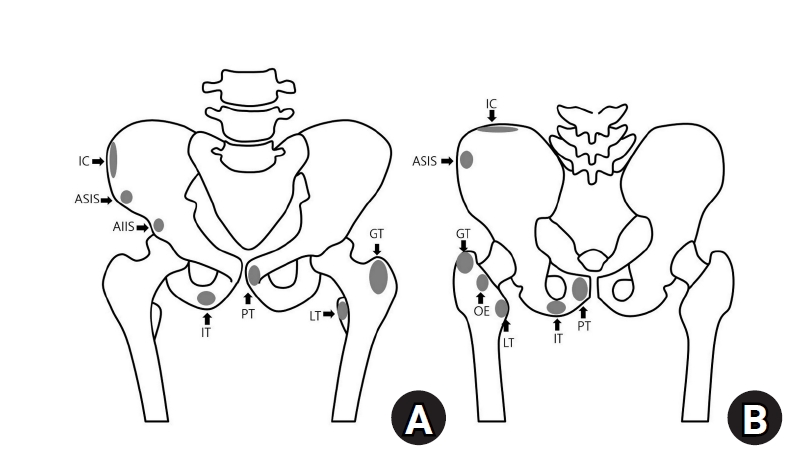
- Avulsion fractures around the hip joint and pelvis
- Won-Sik Choy, Yonghan Cha, Jung-Taek Kim, Jun-Il Yoo, Jin-Woo Kim
- J Musculoskelet Trauma 2025;38(2):53-62. Published online March 24, 2025
- DOI: https://doi.org/10.12671/jmt.2025.00010
-
 Abstract
Abstract
 PDF
PDF - Avulsion fractures occur when tendons or ligaments are subjected to forces greater than they can withstand at the apophysis or enthesis, regardless of fusion status. The pelvis and hip joint are vulnerable to these injuries due to the diverse muscular structures in these structures, which serve as origins for multiple muscles leading to the lower extremities. Pelvic avulsion fractures commonly affect young athletes, but can also occur in adults. The diagnosis typically involves assessing trauma history, a clinical examination, and radiographic imaging. If the diagnosis is unclear, additional tests such as computed tomography and magnetic resonance imaging may assist in the diagnosis and provide useful information for treatment decisions. While most avulsion fractures respond well to conservative treatment, surgical intervention may be preferred in severe displacements, cases of significant retraction in active athletes, or when a faster recovery is necessary. Chronic or neglected injuries may lead to excessive osseous formation around the pelvis, causing impingement syndromes. Recognizing characteristic radiological findings based on pelvic anatomy helps to make an accurate diagnosis, as chronic injuries can mimic tumors or infectious conditions, necessitating a careful differential diagnosis.
-
Citations
Citations to this article as recorded by- Avulsion Fracture of the Lesser Trochanter and the Use of Conservative Treatment
Dawid Bartosik, Bartlomiej Cwikla, Anna Kowalczyk, Michalina Loson-Kawalec, Anna Palka-Szymaniec, Bartosz Starzynski, Alina Keska, Jakub Szkuta, Klaudia Wojcik
Cureus.2026;[Epub] CrossRef - Outcomes of Conservative Versus Surgical Treatment of Adolescent Pelvic and Hip Avulsion Fractures: A Systematic Review and Meta-Analysis
Lindsey L. Molina, Andrew M. Block, Sasha Carsen, Allison E. Crepeau, Tyler J. Stavinoha, Michael M. Chau, Jeffrey J. Nepple
Journal of Pediatric Orthopaedics.2026;[Epub] CrossRef
- Avulsion Fracture of the Lesser Trochanter and the Use of Conservative Treatment
- 13,660 View
- 178 Download
- 2 Crossref

- Avulsion Fractures around the Hip Joint and Pelvis
- Ha-Yong Kim, Hajun Jang, Jung-Taek Kim, Jin-Woo Kim, Jun-Il Yoo, Won-Sik Choy, Yonghan Cha
- J Korean Fract Soc 2024;37(3):150-157. Published online July 31, 2024
- DOI: https://doi.org/10.12671/jkfs.2024.37.3.150
-
 Abstract
Abstract
 PDF
PDF - Avulsion fractures occur when tendons or ligaments are subjected to forces greater than they can withstand at the apophysis or enthesis, regardless of the fusion status. Given the diverse muscular structures around the pelvis and hip joint, which serve as origins for multiple muscles leading to the lower extremities, these areas are vulnerable to such injuries. Pelvic avulsion fractures commonly af-fect young athletes, but they can also occur in adults. Diagnosis typically involves assessing the trauma history, clinical examination, and radiographic imaging. In cases of unclear diagnosis, additional tests, such as computed tomography or magnetic resonance imaging, may assist in treatment decisions and diagnosis. Although most avulsion fractures respond well to conservative treatment, surgical interven-tion may be preferred in severe displacements, significant retraction in active athletes, or when a faster recovery is necessary. Chronic or neglected injuries may lead to excessive osseous formation around the pelvis, causing impingement syndromes. Recognizing the characteristic radiological findings based on the pelvic anatomy aids in accurate diagnosis because chronic injuries might mimic tumors or infectious conditions, necessitating a careful differential diagnosis.
- 2,113 View
- 49 Download

Original Articles
- The Cause of Primary Reduction Failure in Hip Dislocation with or without Hip Fracture
- Hee Gon Park, Yong Eun Shin, Sung Hyun Kim
- J Korean Fract Soc 2017;30(1):9-15. Published online January 31, 2017
- DOI: https://doi.org/10.12671/jkfs.2017.30.1.9
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
A rapid and accurate reduction is important for hip dislocated patients to avoid various potential complications, including avascular necrosis of the femoral head. We analyzed hip dislocation cases, ones that particularly failed during the primary reduction trial.
MATERIALS AND METHODS
Eighty-seven patients with hip dislocation, who visited the emergency department between January 2007 and September 2015, were retrospectively analyzed. Of them, 68 patients were successfully treated in the first closed reduction trial, and the remaining 19 patients were unsuccessful. Of the 19 unsuccessful first trial, 12 patients were successfully treated in the second closed reduction; however, in the remaining 7 patients, open reduction was performed in the operation room with general anesthesia. Every closed reduction was practiced by at least 2 orthopedic doctors, and open reduction was performed by a single senior author.
RESULTS
The rate of first reduction failure was higher, with statistical significance, in patients aged under 50 years, male gender, and those with combined around hip fractures, including femoral head and acetabular fracture (p<0.05). In particular, the presence of impacted fracture fragment in the hip joint and large size of the impacted fracture fragment was highly related to the failure of second closed reduction trial requiring open reduction. Conversely, the method of reduction, Thompson-Epstein classification, Pipkin classification were not related to the failure of closed reduction statistically (p>0.05).
CONCLUSION
To evaluate the patients with hip dislocation, realizing the type of dislocation, presence of accompanied fracture, location and size of fracture fragment, age, as well as gender of patients is important. If the fracture fragment is impacted in the hip joint and the size of the fragment is large, then the operative treatment is considered, rather than the repetitive trial of closed reduction by constraint. -
Citations
Citations to this article as recorded by- Atypical and unclassifiable hip dislocation with capsule and labrum incarceration: a case report and review of the literature
Francis Zifa Pentèce Zengui, Moise Radam Ellah, Kevin Bienvenu Parfait Bouhelo-Pam, Arnauld Sledge Wilfrid Bilongo-Bouyou, Nevil Stève Ngona Gampio Mvili, Marius Monka
International Journal of Surgery Case Reports.2025;[Epub] CrossRef - Traumatic obturator dislocation of the hip joint
Z. F. Zengui, O. El Adaoui, M. Fargouch, O. Adnane, Y. El Andaloussi, M. Fadili
International Journal of Surgery Case Reports.2022; 93(C): 106983. CrossRef
- Atypical and unclassifiable hip dislocation with capsule and labrum incarceration: a case report and review of the literature
- 1,361 View
- 8 Download
- 2 Crossref

- Result of Surgical Treatment for the Femoral Head Fracture
- Joon Soon Kang, Kyoung Ho Moon, Tong Joo Lee, Jong Hyuck Yang
- J Korean Fract Soc 2014;27(3):198-205. Published online July 31, 2014
- DOI: https://doi.org/10.12671/jkfs.2014.27.3.198
-
 Abstract
Abstract
 PDF
PDF - PURPOSE
This study analyzed the clinical and radiological long-term follow-up results of patients with femoral head fracture who received surgical treatments.
MATERIALS AND METHODS
Retrospective evaluation was performed for 20 patients with femoral head fracture who received surgical treatments between December 1997 and May 2010. According to Pipkin's classification, there were five type I, six type II, one type III, and eight type IV fractures.
RESULTS
The average Merle d'Aubigne'-Postel score was 12.8 (12.80+/-3.53). According to surgical method, the score for the bony fragment excision group was 9.8 (9.83+/-2.79), and that for the open reduction and internal fixation group was 13.9 (13.92+/-3.07). Depending on Thompson-Epstein criteria, two patients were good, two were fair, and two were poor in the bony fragment excision group. Four patients were excellent, six were good, and three were poor in the open reduction and internal fixation group.
CONCLUSION
Bony fragment excision should be performed with caution in patients with femoral head fracture. Considering fragment size, location, and presence of acetabular fracture, better outcome can be expected using the open reduction and internal fixation method in comparison with excision.
- 691 View
- 3 Download

Case Reports
- Vertically Unstable Fracture of the Pelvis Combined with Anterior Dislocation of the Hip Joint: A Case Report
- Kap Jung Kim, Ha Yong Kim, Dae Suk Yang, Won Sik Choy
- J Korean Fract Soc 2007;20(3):272-276. Published online July 31, 2007
- DOI: https://doi.org/10.12671/jkfs.2007.20.3.272
-
 Abstract
Abstract
 PDF
PDF - Pelvic fractures result from high energy trauma and often associated with concomitant injuries. But, vertically unstable pelvic fractures combined with anterior dislocation of the hip is far less common. The traumatic dislocation of the hip is a true orthopedic emergency and it should be considered that a femoral head can be exposed to deteriorized vascularity. We report a case of vertically unstable pelvic fractures combined with traumatic anterior dislocation of the hip joint with the review of the literature.
- 605 View
- 1 Download

- Hip Fracture-dislocation with Sciatic Nerve Palsy and Ipsilateral Femoral Shaft Open Fracture: A Case Report
- Kap Jung Kim, Ha Yong Kim, Sung Il Kang, Won Sik Choy
- J Korean Fract Soc 2007;20(1):94-98. Published online January 31, 2007
- DOI: https://doi.org/10.12671/jkfs.2007.20.1.94
-
 Abstract
Abstract
 PDF
PDF - The posterior dislocation of the hip accounts for about 85~90% of traumatic hip dislocations and high energy mechanisms such as traffic accidents may cause them. The traumatic dislocation and fracture-dislocation of the hip are true orthopedic emergencies and it should be considered that a femoral head has poor vascularity and the sciatic nerve is closely located to it. We report on one patient who went through the surgical treatment of the concomitant ipsilateral open fracture of the femoral shaft and hip fracture-dislocation accompanying sciatic nerve injury with the review of the literatures.
- 981 View
- 4 Download

Original Article
- Differences of Bone Mineral Density and Fracture Threshold Between Hip Joint Fracture and the Control group
- Ig Gon Kim, Jae Hyek Kim, Cul Hyun Kim, Jong Suck Kim
- J Korean Soc Fract 1999;12(2):231-238. Published online April 30, 1999
- DOI: https://doi.org/10.12671/jksf.1999.12.2.231
-
 Abstract
Abstract
 PDF
PDF - Osteoporosis represents reduced amount of bone mass per unit volume as compared with controls of the same age and sex. In this condition, bone mineral density decreases and the skeleton becomes more prone to fracture. The purpose of this study was to show how bone mineral densities of the femoral neck area decrease with aging, to in vestigate the relationship between the bone mineral densities of the control and fracture group, and to obtain fracture threshold values. This report observed BMD of femoral neck region in femoral neck and intertrochanteric fracture group was less than that of control group and the differences were significant. We measured and evaluated BMD of femoral neck region by DEXA in 234 normal volunteers(99 men and 135 women), in 105 patien ts with femoral neck fracture(41 men and 64 women) and in 103 patients with intertrochanteric fracture(40 men and 63 women) above 50 years-old. Following results were obtained: 1. The average BMD of femoral neck region in control group, femoral neck fracture group and intertrochanteric fracture group were 0.751+/-0.030 g/cm2 in male and 0.661+/-0.089g/cm2 in female, 0.660+/- 0.031g/cm2 in male and 0.557+/-0.002g/cm2 in female and 0.661+/-0.008g/cm2 in male and 0.562+/-0.005g/cm2 in 2. The BMD of the control group and fracture group decreased with aging and were higher in men than in women and there were statistically significant difference(p<0.001). 3. There were statistically significant difference between BMD of the control group and BMD of the hip fracture group(p<0.005) but no significant differences between BMD of the femoral neck fracture group and intertrochanteric fracture group. 4. Fracture threshold of the hip fracture group were 0.815g/cm2(male:0.832g/cm2, female:0.733g/cm2) according to 95 percentile.
- 586 View
- 2 Download

Case Report
- Subluxation of the Hip Following to the Treatment of Irochanteric Fracture of the Femur: A case report
- K Y Kim, J S Chang, S H Lee, B H Han
- J Korean Soc Fract 1996;9(1):235-240. Published online January 31, 1996
- DOI: https://doi.org/10.12671/jksf.1996.9.1.235
-
 Abstract
Abstract
 PDF
PDF - It has been emphasized that the choice of treatment for the trochanteric fracture of the femur is open reduction and stable internal fixation to reduce complications by early ambulation. Recently dynamic hip screws(DHS) are very popular to the treatment of trochanteric fracture of the femur but they have some complications. Postoperative complications of the trochanteric fracture of the femur include malunion, delayed union, nonunion, disengagement of lag screw from sideplate, metal failure and the screw cutting-out of the femoral head, but subluxation of the hip has not reported as a complication. We experienced a rare case of trochanteric fracture which was treated with open reduction and internal fixation with DHS and was found to be subluxation of its hip at postoperative 4 weeks, which was managed by cemented bipolar endoprethesis.
- 435 View
- 0 Download

Original Article
- Application of orthofix dynamic axial fixator for the fracture and dislocation around the hip joint report of four cases
- Kyu Hyun Yang, Joon Sup Jahng, Hyun Woo Kim
- J Korean Soc Fract 1991;4(2):275-280. Published online November 30, 1991
- DOI: https://doi.org/10.12671/jksf.1991.4.2.275
- 573 View
- 2 Download


 E-submission
E-submission KOTA
KOTA TOTA
TOTA TOTS
TOTS

 First
First Prev
Prev


