Abstract
Avulsion fractures occur when tendons or ligaments are subjected to forces greater than they can withstand at the apophysis or enthesis, regardless of fusion status. The pelvis and hip joint are vulnerable to these injuries due to the diverse muscular structures in these structures, which serve as origins for multiple muscles leading to the lower extremities. Pelvic avulsion fractures commonly affect young athletes, but can also occur in adults. The diagnosis typically involves assessing trauma history, a clinical examination, and radiographic imaging. If the diagnosis is unclear, additional tests such as computed tomography and magnetic resonance imaging may assist in the diagnosis and provide useful information for treatment decisions. While most avulsion fractures respond well to conservative treatment, surgical intervention may be preferred in severe displacements, cases of significant retraction in active athletes, or when a faster recovery is necessary. Chronic or neglected injuries may lead to excessive osseous formation around the pelvis, causing impingement syndromes. Recognizing characteristic radiological findings based on pelvic anatomy helps to make an accurate diagnosis, as chronic injuries can mimic tumors or infectious conditions, necessitating a careful differential diagnosis.
-
Keywords: Bone fractures, Avulsion fractures, Hip joint, Pelvis
Introduction
An avulsion fracture typically occurs at an apophysis or enthesis when the tensile forces on a tendon or ligament exceed the limits of resistance, irrespective of fusion status. This phenomenon is observed around the pelvis and hip as well [
1]. Anatomically, the site where a tendon or ligament attaches to bone is referred to as the enthesis, which plays a critical role in the concentration and transmission of forces between two distinct types of tissue [
2,
3]. Various muscle structures surround the pelvis and hip, and since these areas serve as origins for multiple muscles extending to lower extremity joints, they are particularly vulnerable to such injuries (
Fig. 1) [
1]. While avulsion fractures may occur as a result of a single acute trauma, they can also progress chronically due to repetitive stress. In adults, avulsions are primarily seen in soft tissues, whereas in adolescents, they typically present with displaced bone fragments or apophyseal injuries [
1].
Imaging modalities are essential for diagnosing avulsion fractures around the pelvis and hip. Radiographs should be the first step in the diagnostic process, as they can reveal displaced bone fragments or apophyseal injuries; however, caution is necessary to avoid overlooking lesions obscured by around structures. Although diagnosis can often be achieved with typical trauma history, physical examination, and radiographic findings, computed tomography (CT) or magnetic resonance imaging (MRI) may be utilized to gain a more detailed understanding of the anatomical configuration of the injured area. CT is particularly effective for assessing the presence and morphology of displaced apophyses or bone fragments, as well as identifying callus or heterotopic ossification that aids in distinguishing between acute and chronic avulsion fractures. MRI provides superior visualization of bone marrow edema, hematomas, and soft tissue injuries, and it is valuable for assessing the degree of tendon retraction, which can be crucial in determining the need for surgical intervention. Although ultrasound is a highly effective tool for diagnosing acute avulsion injuries, its accuracy can be significantly influenced by the examiner's expertise, and it may pose challenges in visualizing the anatomical relationships among damaged structures.
There are various types of avulsion fractures around the hip joint and pelvis, most of which are uncommon. While appropriate treatment methods based on fracture type have been proposed for some relatively common fractures, many others lack such guidelines. Due to their low incidence, there is a lack of reported literature or reviews, as well as insufficient evidence regarding treatment methods. Thus, the purpose of this review is to summarize the clinical and radiological findings of various types of avulsion fractures occurring around the pelvis and hip, based on existing literature, and to present appropriate treatment options.
Ethics Statement
This review was approved by the Institutional Review Board (IRB) of Daejeon Eulji Medical Center (IRB No. EMC 2024-11-005). Written informed consent was waived for all patients involved in this review.
Avulsion Fractures Around the Pelvis
Avulsion Fractures of the Iliac Crest
The iliac crest extends from the anterior superior iliac spine (ASIS) to the posterior superior iliac spine and serves as an attachment site for the anterior abdominal wall muscles. Avulsion fractures of the iliac crest typically result from excessive tension and contraction of the abdominal muscles during lateral bending and rotational movements of the trunk [
4]. However, such injuries are rare, accounting for only about 1%–2% of avulsion fractures around the pelvis and hip [
5].
On physical examination, patients with iliac crest avulsion fractures may report tenderness over the iliac crest. Radiographs can reveal asymmetry at the iliac crest, while MRI may show edema, bone separation, and avulsion at the attachment site of the anterior abdominal wall muscles [
6,
7].
In most cases, conservative treatment yields excellent outcomes. However, surgical intervention may be considered if there is significant displacement greater than 3 cm, or if the patient requires rapid rehabilitation and return to sports [
8,
9].
The sartorius muscle originates from the ASIS, with part of the tensor fascia lata attaching nearby. Avulsion fractures at the ASIS are relatively common, accounting for approximately 28% of pelvic avulsion injuries, and are typically triggered by sudden and rapid hip extension during activities such as running or jumping [
10]. On physical examination, patients often exhibit tenderness over the ASIS, and in some cases, the avulsed fragment may be palpable [
7]. The displaced fragment tends to migrate inferolaterally and can sometimes be mistaken for an avulsion injury of the anterior inferior iliac spine (AIIS).
Although diagnosis can generally be made based on clinical presentation and radiographs alone, additional imaging with CT or MRI may be necessary when radiographs are inconclusive or when the patient presents later after the injury (
Fig. 2) [
11,
12]. In rare instances, a hematoma or excessive bone formation following an avulsion fracture may compress the lateral femoral cutaneous nerve, potentially leading to meralgia paresthetica [
13,
14]. Cases have also been reported where avulsion fractures were initially mistaken for bony tumors invading the soft tissues [
15].
Most avulsion fractures with minimal displacement can be managed successfully with conservative treatment, which is widely recommended in the literature [
16]. Typically, patients undergo partial weight-bearing for approximately 3 weeks, followed by full weight-bearing within the next 3 weeks, with return to sports activities around 3 months post-injury. However, surgical intervention, such as open reduction and screw fixation, may be considered in cases of displacement greater than 1.5 to 2 cm, large fragment size, or patient preference for rapid recovery [
16,
17]. Akhter et al. [
16] proposed a surgical approach using suture anchors and lag screws to minimize irritation caused by hardware protrusion. Eberbach et al. [
10] and Kautzner et al. [
18] reported heterotopic ossification in five out of 13 patients who underwent surgical treatment, a rate higher than in those treated conservatively. While surgical management may provide a shorter initial recovery period, long-term outcomes between conservative and surgical treatments may not differ significantly [
10,
18-
20].
The straight head of the rectus femoris originates from the AIIS and spans both the hip and knee joints. Since the rectus femoris functions to flex the hip and extend the knee, avulsion fractures of the AIIS are often caused by hip extension injuries, similar to avulsion fractures of the ASIS. These fractures typically occur during activities involving running, jumping, or kicking, making them common injuries in sports such as soccer. AIIS avulsion fractures, like those of the ASIS, are relatively frequent and are reported to account for approximately 20%–25% of pelvic avulsion fractures [
21].
On clinical examination, patients often present with anterior hip or groin pain and tenderness. Pain may be elicited during resisted hip flexion or knee extension combined with hip flexion. While a small bone fragment may be visible on standard anteroposterior pelvic radiographs, an oblique view can be helpful for confirming the diagnosis. Ultrasound and MRI may also be used as additional diagnostic tools, with MRI particularly valuable for assessing soft tissue injuries and the degree of muscle retraction (
Fig. 3). Excessive heterotopic callus formation can lead to a reduced distance between the greater trochanter and the acetabular roof, potentially resulting in femoroacetabular impingement, which may cause chronic hip pain [
22].
Both AIIS and ASIS avulsion fractures generally produce milder symptoms and functional limitations and have a shorter recovery period compared to avulsion fractures of the ischial tuberosity (
Fig. 4) [
1].
Maalouly et al. [
23] reported a case of an avulsion fracture of the AIIS following hip arthroscopy for femoroacetabular impingement. The procedure was performed on a traction table, with cam and pincer lesions removed using a burr. Since the acetabular labrum was stable, no additional fixation was required. Eleven months postoperatively, an avulsion fracture of the AIIS was identified, and open reduction and internal fixation were performed, yielding satisfactory results. Conservative treatment for AIIS avulsion fractures typically involves protected weight-bearing for 6–8 weeks [
24]. Hsu et al. [
25] reported on two American football players who were treated conservatively, achieving normal activity by 6 weeks. Gamradt et al. [
26] also reported cases of AIIS avulsion fractures in 11 American football players, all of whom successfully returned to sport with conservative management. Conversely, Irmola et al. [
27] presented five cases in four American football players who underwent surgical treatment and were able to return to sport after 9 months, although two cases experienced lateral femoral cutaneous nerve palsy.
Rossi and Dragoni [
5] reported that the ischial tuberosity is the most common site of pelvic avulsion fractures in adolescents. The ischial tuberosity serves as the insertion point for the hamstring muscles, including the long head of the biceps femoris, semitendinosus, and semimembranosus. Avulsion fractures in this area can occur during intense hip flexion and knee extension or as a result of excessive, sudden leg traction, particularly among athletes such as soccer players, runners, and dancers [
28]. Patients typically present with characteristic buttock pain that worsens when sitting rather than standing, along with gait disturbances and localized swelling. Despite the typical injury mechanism and symptoms, delayed diagnosis may occur, necessitating careful attention.
Radiographically, acute fractures are seen as bone fragments with curved, sharp borders, while non-displaced fractures may require differentiation from tumor-related bone formations (
Fig. 5) [
29]. Although radiographs may suffice for diagnosis, ultrasound and MRI can be useful for assessing associated injuries or hematoma formation.
Currently, there are no definitive guidelines for treating this type of fracture, but conservative management is generally recommended [
24]. Surgical intervention with open reduction and internal fixation is considered only in cases of significant fragment displacement. Eberbach et al. [
10] and Ferlic et al. [
30] reported that surgical treatment is indicated when displacement exceeds 1.5 cm. In conservative management, it is important to prevent hip flexion and maintain the knee in a flexed position, which may require a brace [
24]. Return to sports is typically advised after 1.5 to 3 months. The surgical approach can involve the Kocher-Langenbeck approach or an incision along the gluteal crease, using metal plates, screws, or suture anchors, or creating a bone tunnel for suturing [
31]. Postoperatively, weight-bearing should be gradually resumed to avoid complications with hardware failure. A brace should limit excessive hamstring tension for 6–12 weeks, with return to full activity usually allowed after 5–6 months, as rehabilitation takes longer than for other pelvic avulsion fractures.
Complications of this fracture include neuralgia due to sciatic nerve irritation from fracture fragments, callus formation, or heterotopic ossification [
32]. Other complications include excessive bone formation around the ischial tuberosity or decreased space between the ischium and femur, which may lead to ischiofemoral impingement syndrome, where the quadratus femoris muscle becomes compressed [
33]. Delayed diagnosis may result in sciatic nerve palsy caused by the displaced bone fragment [
24].
The hip adductor muscles, including the adductor longus, adductor brevis, gracilis, and the distal rectus abdominis, originate from the pubic body, pubic symphysis, and the inferior pubic ramus [
34]. Among these, the adductor longus is the most frequently injured, followed by the adductor brevis and the pectineus muscle [
35]. In contrast, the gracilis and adductor magnus are less prone to injury. Avulsion fractures caused by the adductors typically result from chronic overuse and accumulation of repeated microtraumas, with acute injuries from sudden contractions being rare. Such injuries are common in athletes, particularly soccer, ice hockey, and tennis players.
Patients usually present with unilateral groin pain, which may be nonspecific, and chronic cases are referred to as "Athletic Pubalgia." Differential diagnosis should consider osteitis pubis, sports hernia (core muscle injury), acetabular labral tear, and spinal disorders [
36,
37].
Since adductor injuries primarily involve soft tissue and avulsion fractures are rare, diagnosis is challenging through radiographs and physical examination alone. MRI can be particularly helpful in identifying the type and extent of the injured adductor muscles [
38,
39]. Treatment typically involves conservative management, with recommendations to cease sports activities and avoid weight-bearing for several weeks.
The obturator externus muscle originates from the outer rim of the obturator foramen and the obturator membrane, attaching to the piriformis fossa on the medial aspect of the femoral greater trochanter. While the exact mechanism of avulsion fractures in this area is unclear, these injuries are rare and are more often muscle strains than true avulsion fractures [
35]. They are characteristically seen in high-level athletes, such as professional soccer players, presenting with anterior hip pain that is exacerbated by internal and external rotation of the flexed hip [
40]. Recovery is generally swift, allowing athletes to return to sports relatively quickly.
Avulsion Fractures around the Proximal Femur
Avulsion Fractures of the Greater Trochanter
The muscles attaching to the greater trochanter include the hip external rotators and abductors, and avulsion fractures in this area are extremely rare, typically occurring during sudden, forceful directional changes. Radiographs may reveal displacement of the fracture, while MRI can show widening of the growth plate gap and edema. Clinically, patients present with pain and tenderness at the greater trochanter, with pain worsening during abduction and adduction movements.
As this is a very rare injury, there is no clear evidence supporting a specific treatment protocol. In adolescents, conservative treatment typically involves limiting movement and gradually increasing stress over a 6-week period [
21]. Open reduction and internal fixation may be considered in cases of significant displacement, particularly in older individuals where direct trauma from a fall might occur. For apparent avulsion fractures of the greater trochanter in the elderly, the differential diagnosis should include occult intertrochanteric fractures [
41]. In many cases, the avulsion fragments are only part of the fracture, and an incomplete intertrochanteric fracture may be present, which can be detected using MRI [
41].
There have been reports of avascular necrosis of the femoral head following avulsion fractures of the greater trochanter, likely due to damage to the associated blood vessels, such as the medial circumflex artery and the cervical branches [
42-
44]. Khalifa et al. [
45] reported the case of a 13-year-old boy who sustained an avulsion fracture of the greater trochanter of the left femur along with an open dislocation of the hip following a tractor accident. The fracture was easily reduced with traction, and non-surgical treatment was successfully implemented. However, severe heterotopic ossification around the hip joint limited its range of motion, and after 3 years, avascular necrosis of the femoral head developed, ultimately leading to the need for total hip replacement surgery at the age of 18. Giles et al. [
46] reported a case of apophyseal avulsion of the greater trochanter in a 14-year-old boy that occurred during a soccer game after being tackled. They applied a hip abduction brace (with the hip in 30° of flexion and 20° of abduction) for 8 weeks, followed by gradual weight-bearing. The patient was allowed to return to sports activities 6 months after the injury [
46].
Avulsion fractures of the lesser trochanter are rare injuries that can occur in competitive young athletes, such as track and field and soccer players, accounting for 1%–3% of hip avulsion fractures [
10,
21]. These fractures typically occur between the ages of 13 and 18, with very few cases observed in healthy adults [
47,
48]. The iliopsoas muscles attach to the lesser trochanter, and the fracture usually results from a strong contraction of the iliopsoas. It can also occur after a tonic-clonic seizure [
49]. The fracture is associated with significant pain and functional impairment, with relief often occurring in the hip flexion position. Tenderness is noted along the medial thigh, and hip flexion is not possible under resistance.
Radiographs will show displacement of the lesser trochanter, and CT or MRI are generally unnecessary (
Fig. 6). However, if an avulsion fracture of the lesser trochanter is observed in an adult, it may indicate a pathological avulsion fracture due to tumor metastasis, so caution is required during diagnosis (
Fig. 7) [
50,
51]. For these patients, careful history taking including cancer histories and considering contrast-enhanced MRI could be helpful.
Conservative treatment typically yields good results, and surgical intervention is rarely required [
52,
53]. Miyake et al. [
54] reported a case of stress avulsion fracture of the lesser trochanter in a 40-year-old male patient. After 2 weeks of non-weight-bearing and 2 weeks of partial weight-bearing, followed by full weight-bearing, the patient responded well to conservative treatment, despite 1.8 cm of displacement and nonunion. However, Anderson et al. [
55] suggested that surgical intervention should be considered for displacements greater than 2 cm, while Quarrier and Wightman [
56] reported a case of chronic pain due to a lesser trochanter avulsion fracture in an 18-year-old female ballet dancer, where resection of the lesser trochanter was performed after 5 years of symptoms, leading to improvement. Khemka et al. [
57] utilized arthroscopy-assisted fixation with metal screws or suture anchors, achieving satisfactory results.
Conclusions
Avulsion fractures around the hip joint and pelvis are common in young athletes but can also occur in adults. Diagnosis is typically based on the patient's history of trauma, clinical examination, and radiographic imaging. If the diagnosis is unclear, additional imaging such as CT or MRI can assist in decision-making regarding treatment and confirming the diagnosis. Most avulsion fractures can be treated conservatively, but surgical intervention may be advantageous in cases of significant displacement, in athletes with substantial tendon retraction, or when rapid recovery is required. Chronic or recurrent injuries can lead to excessive heterotopic ossification around the pelvis, potentially causing impingement syndromes. A solid understanding of pelvic anatomy, along with characteristic radiographic findings, is crucial for accurate diagnosis. Since chronic injuries can mimic tumors or infectious diseases, careful differential diagnosis is necessary.
Article Information
-
Author contribution
Conceptualization: YC. Data curation: JTK. Formal analysis: JWK. Investigation: JIY. Methodology: YC. Software: WSC. Validation: YC. Visualization: YC. Project administration: YC. Writing–original draft: WSC, JTK, JIY, JWK. Writing–review & editing: YC. All authors read and approved the final manuscript.
-
Conflict of interests
None.
-
Funding
None.
-
Data availability
Not applicable.
Fig. 1.The main locations of avulsion fractures occurring around the pelvis and hip joints. (A) Anterior view. (B) Posterior view. IC, iliac crest; ASIS, anterior superior iliac spine; AIIS, anterior inferior iliac spine; IT, ischial tuberosity; PT, pubic tubercle; LT, lesser trochanter; GT, greater trochanter; OE, obturator externus muscle insertion.
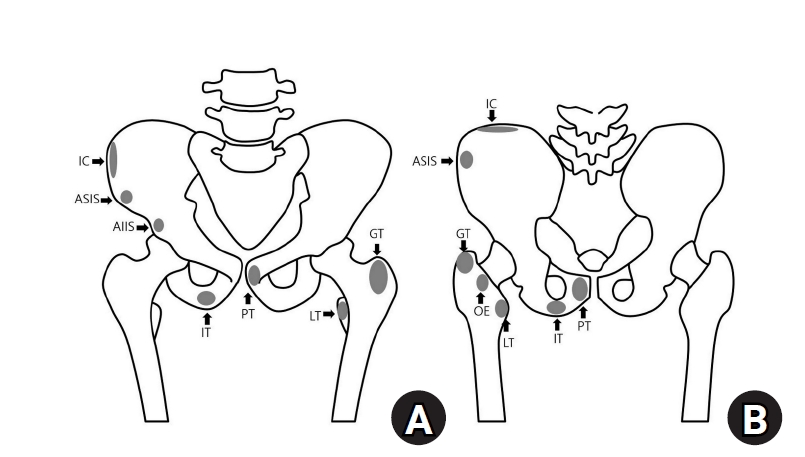
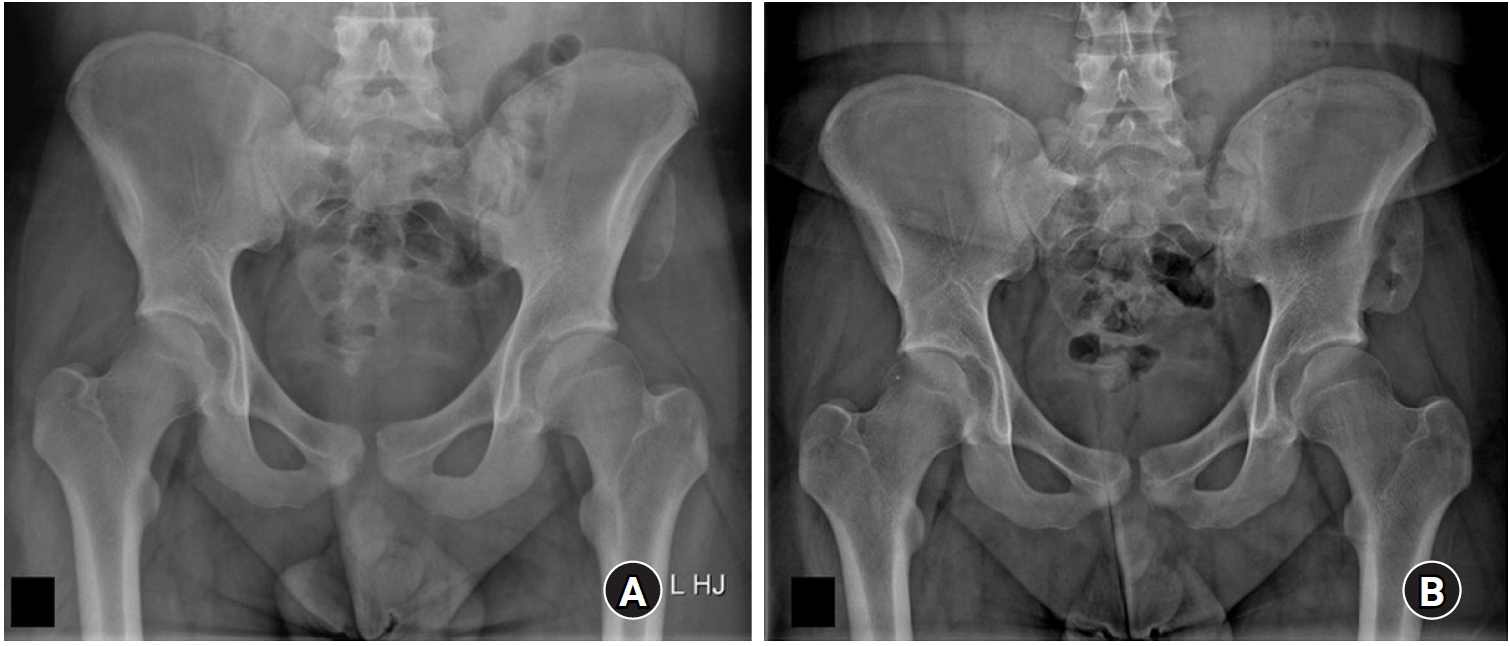
Fig. 2.A 17-year-old male patient presented to the emergency department with sudden pelvic pain while running. (A) A radiograph of the patient's pelvis revealed an avulsion fracture at the left anterior superior iliac spine. (B) Conservative treatment led to healing with anterior displacement but union of the fracture.
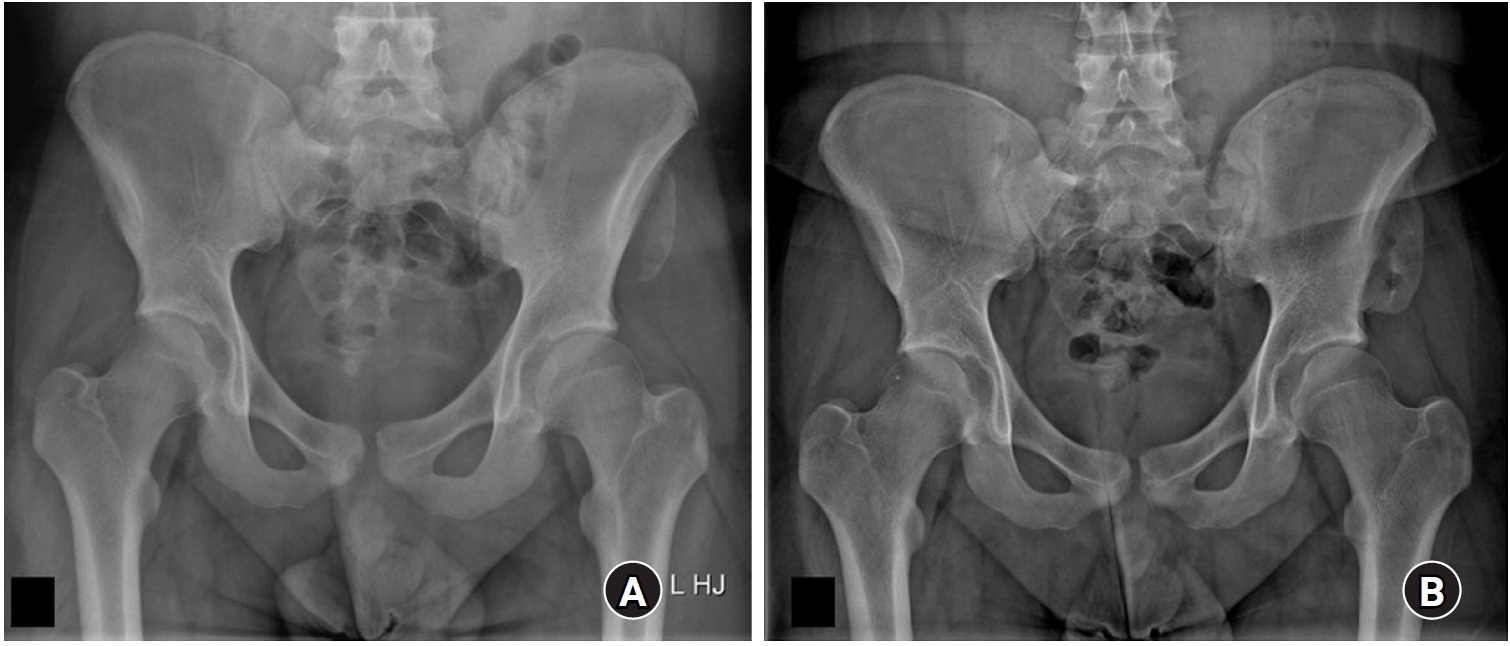
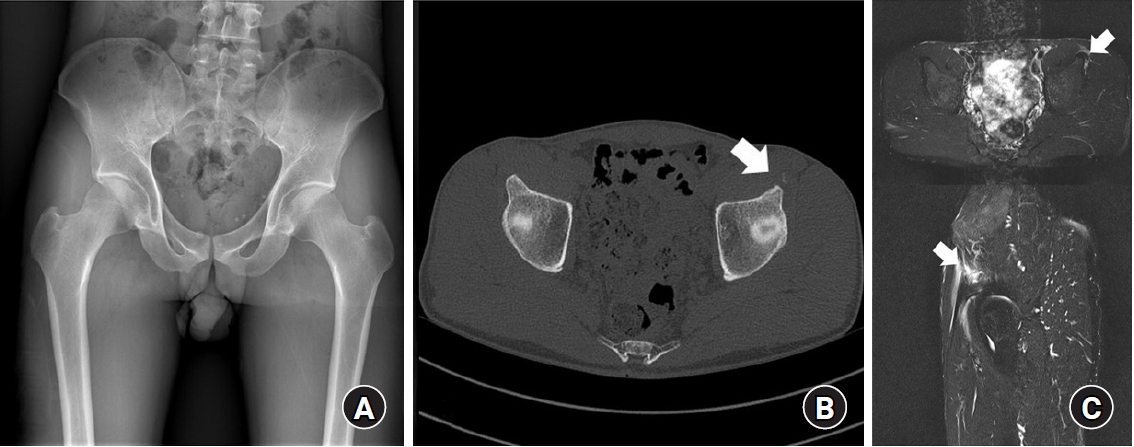
Fig. 3.A 40-year-old male patient presented to the emergency department with left hip pain following excessive stretching. (A) A pelvic radiograph of the patient did not reveal any abnormalities. (B) However, a small avulsion fracture at the left lesser trochanter was observed on computed tomography (arrow). (C) Magnetic resonance imaging showed edema around the avulsion fracture at the lesser trochanter and the tendon of the iliopsoas muscle (arrows). The patient improved with conservative treatment over approximately 3 weeks.
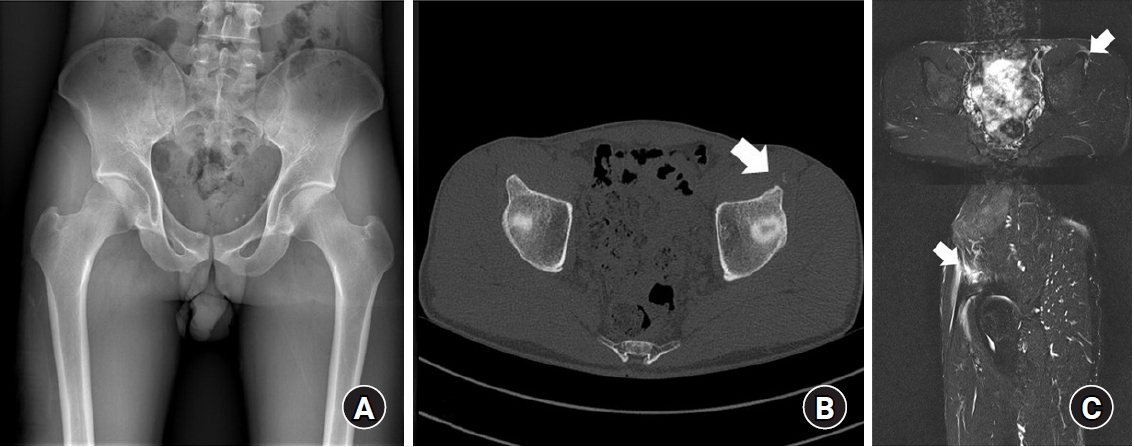
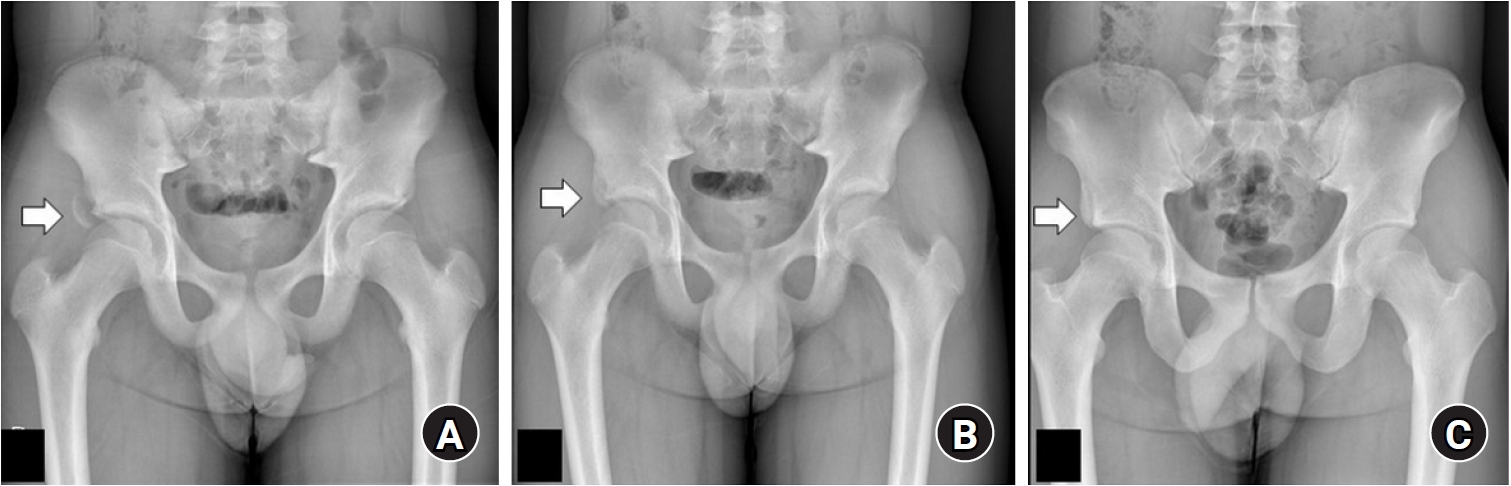
Fig. 4.An 11-year-old male patient presented to the clinic with right hip pain after playing soccer. (A) A radiograph of the hip joint showed an avulsion fracture at the right lesser trochanter (arrow). (B) After 3 months of conservative treatment, radiographs demonstrated bone union (arrow). (C) Seven years after the injury, no specific imaging concerns related to growth were noted, and bone remodeling proceeded well (arrow).
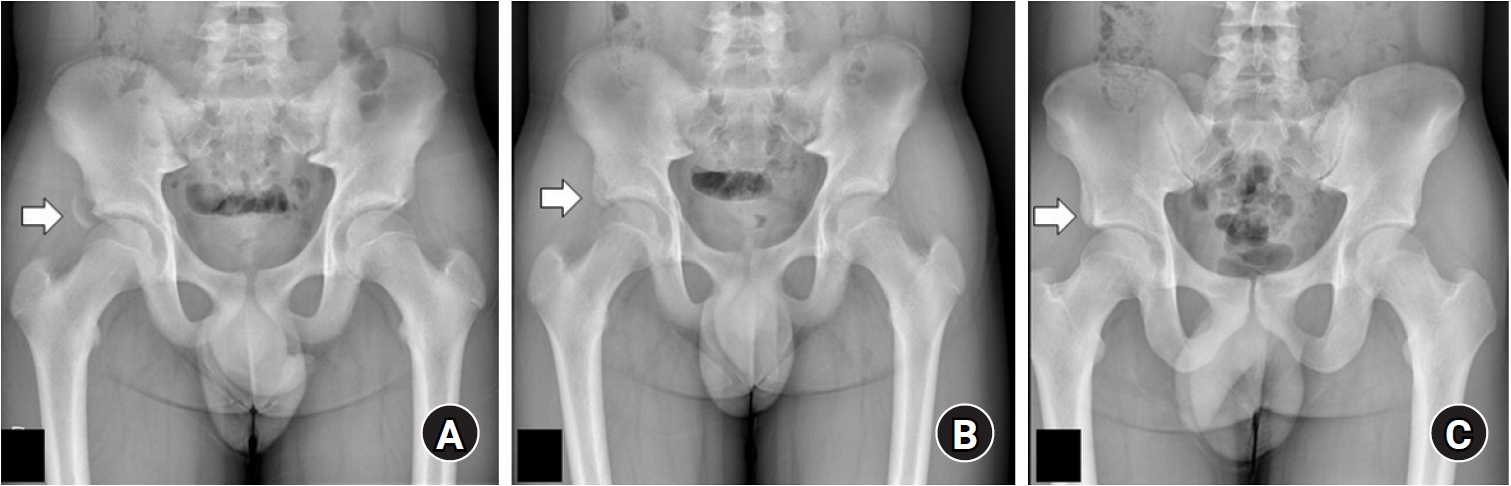
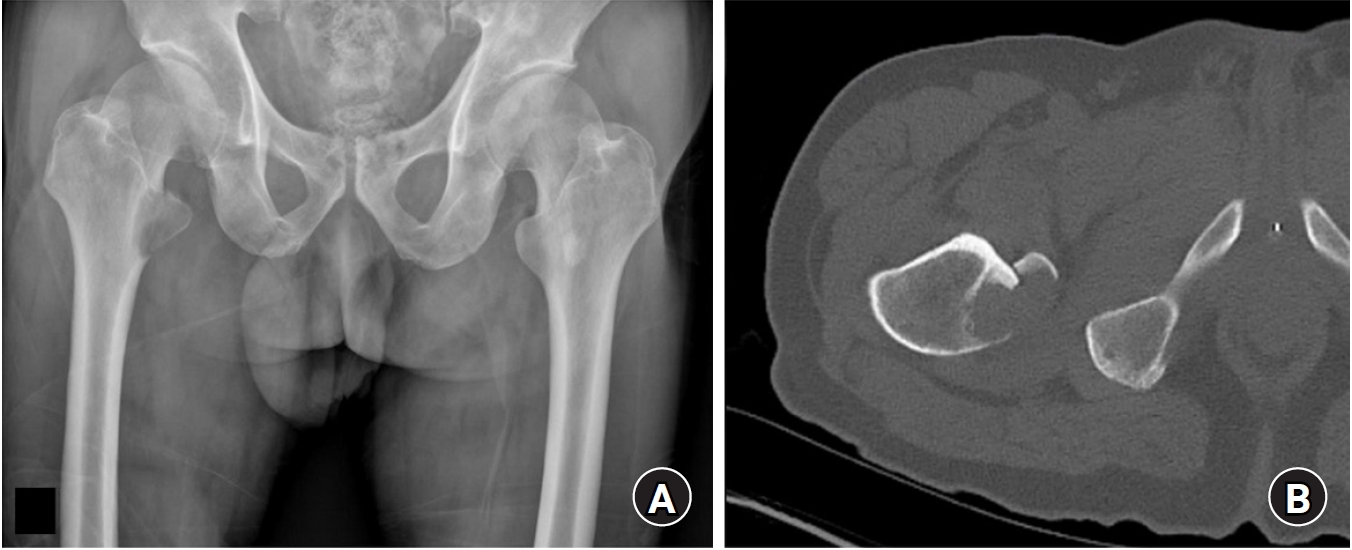
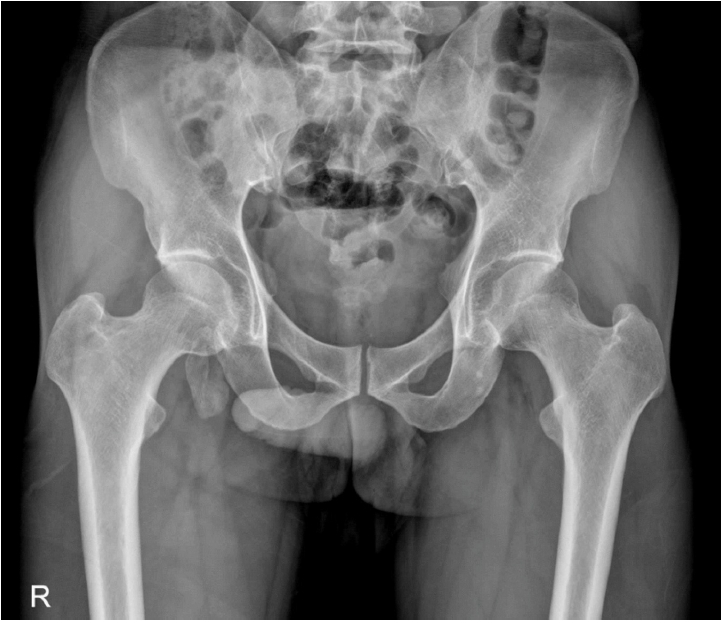
Fig. 5.A 31-year-old male patient presented to the outpatient clinic with persistent pain around the left iliac tuberosity following an injury. Radiographs revealed an avulsion fracture at the left iliac tuberosity with a non-sharp margin, indicating a healed, non-displaced configuration. Symptoms improved with conservative treatment.
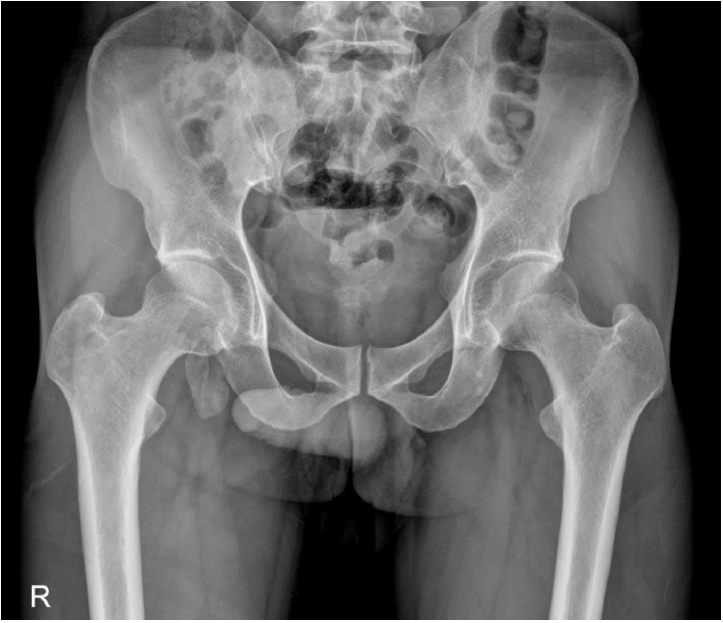
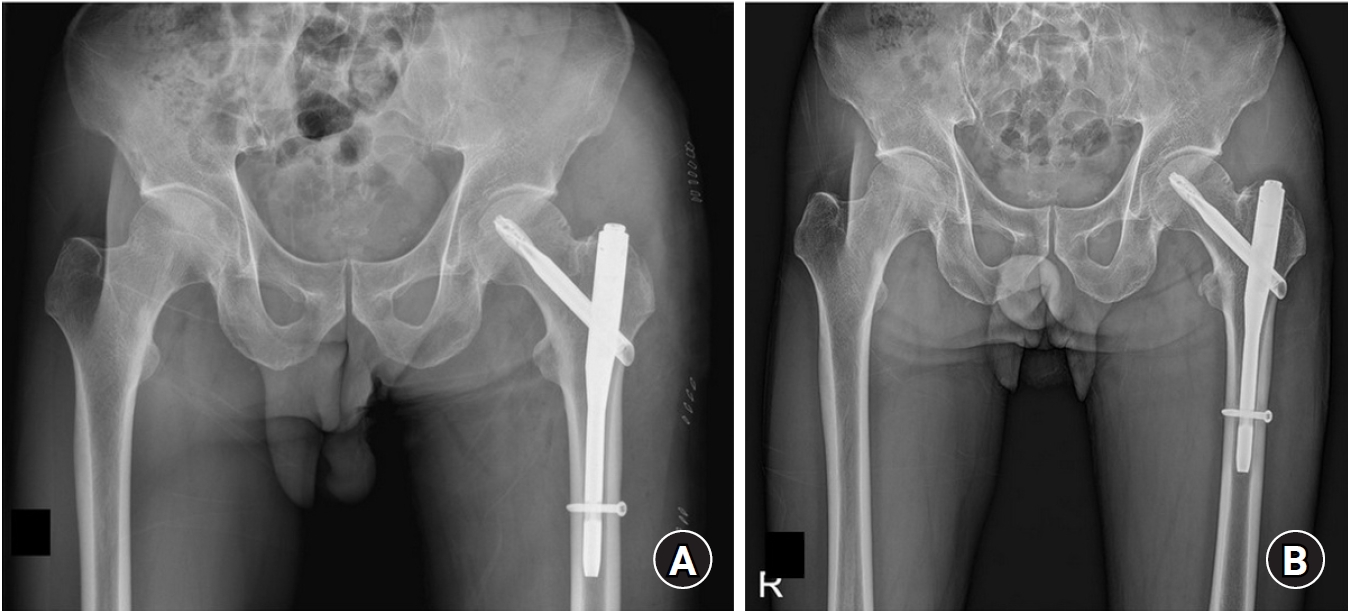
Fig. 6.(A) A 60-year-old male patient underwent surgical treatment for a left femoral intertrochanteric fracture. (B) During the second week of postoperative rehabilitation, the patient complained of worsening pain and underwent follow-up radiography. Radiographs revealed an avulsion fracture accompanied by small bone fragments at the left femoral neck region.
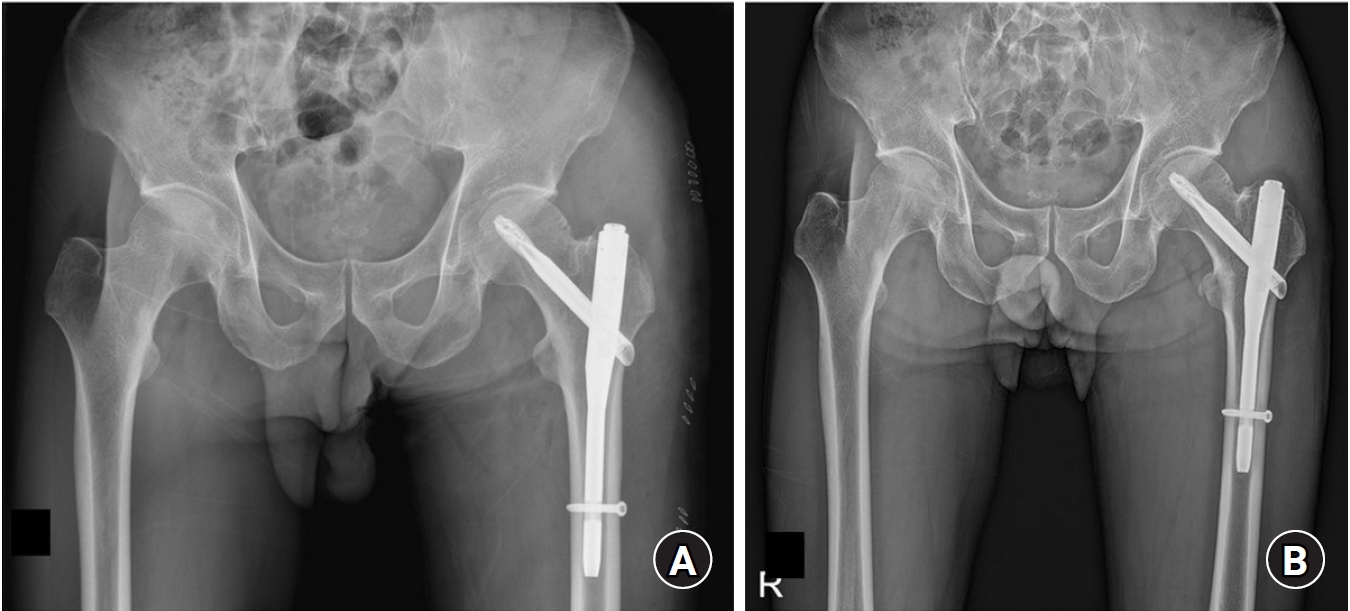
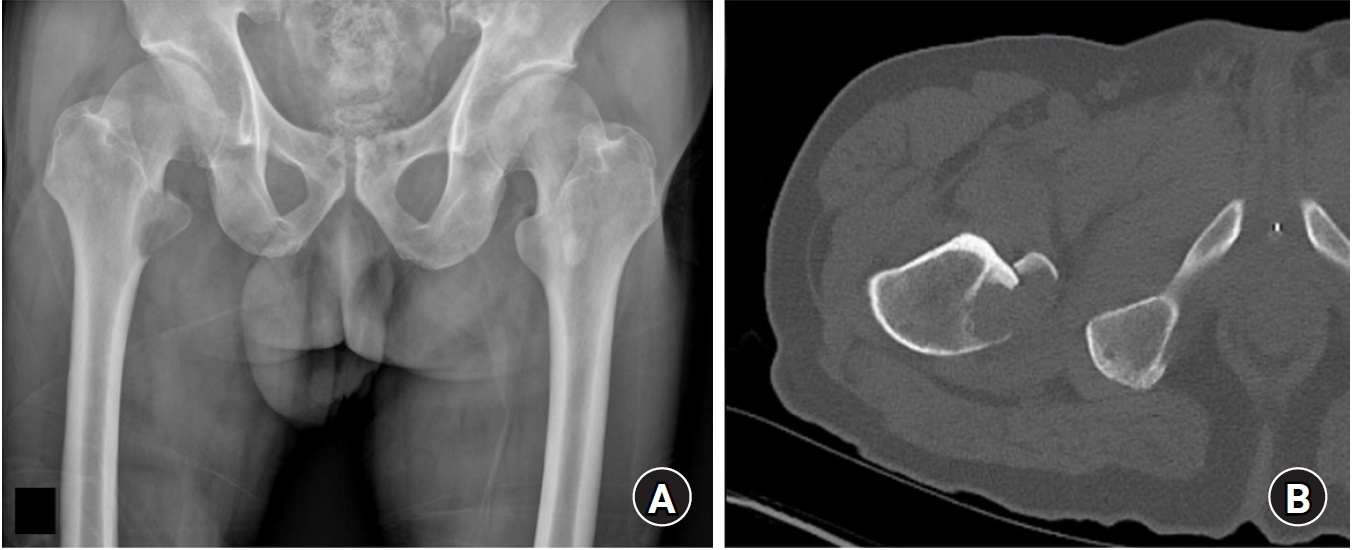
Fig. 7.A 62-year-old male patient undergoing treatment for lung cancer presented to the outpatient clinic 2 days after experiencing persistent right hip pain following coughing. (A) A hip joint radiograph revealed an avulsion fracture of the lesser trochanter of the femur, with observed bone density loss around the fracture site. (B) Computed tomography showed an avulsion fracture of the lesser trochanter accompanied by osteolysis.
References
- 1. Albtoush OM, Bani-Issa J, Zitzelsberger T, Springer F. Avulsion injuries of the pelvis and hip. Rofo 2020;192:431-40.ArticlePubMed
- 2. Shaw HM, Benjamin M. Structure-function relationships of entheses in relation to mechanical load and exercise. Scand J Med Sci Sports 2007;17:303-15.ArticlePubMed
- 3. Benjamin M, Toumi H, Ralphs JR, Bydder G, Best TM, Milz S. Where tendons and ligaments meet bone: attachment sites (‘entheses’) in relation to exercise and/or mechanical load. J Anat 2006;208:471-90.ArticlePubMedPMC
- 4. Steerman JG, Reeder MT, Udermann BE, Pettitt RW, Murray SR. Avulsion fracture of the iliac crest apophysis in a collegiate wrestler. Clin J Sport Med 2008;18:102-3.ArticlePubMed
- 5. Rossi F, Dragoni S. Acute avulsion fractures of the pelvis in adolescent competitive athletes: prevalence, location and sports distribution of 203 cases collected. Skeletal Radiol 2001;30:127-31.ArticlePubMedPDF
- 6. Metzmaker JN, Pappas AM. Avulsion fractures of the pelvis. Am J Sports Med 1985;13:349-58.ArticlePubMedPDF
- 7. El-Khoury GY, Daniel WW, Kathol MH. Acute and chronic avulsive injuries. Radiol Clin North Am 1997;35:747-66.ArticlePubMed
- 8. Li X, Xu S, Lin X, Wang Q, Pan J. Results of operative treatment of avulsion fractures of the iliac crest apophysis in adolescents. Injury 2014;45:721-4.ArticlePubMed
- 9. Kong CG, In Y, Kim SJ, Sur YJ. Avulsion fracture of the iliac crest apophysis treated with open reduction and internal fixation. J Orthop Trauma 2011;25:e56-8.ArticlePubMed
- 10. Eberbach H, Hohloch L, Feucht MJ, Konstantinidis L, Südkamp NP, Zwingmann J. Operative versus conservative treatment of apophyseal avulsion fractures of the pelvis in the adolescents: a systematical review with meta-analysis of clinical outcome and return to sports. BMC Musculoskelet Disord 2017;18:162.ArticlePubMedPMCPDF
- 11. Kjellin I, Stadnick ME, Awh MH. Orthopaedic magnetic resonance imaging challenge: apophyseal avulsions at the pelvis. Sports Health 2010;2:247-51.ArticlePubMedPMCPDF
- 12. Sanders TG, Zlatkin MB. Avulsion injuries of the pelvis. Semin Musculoskelet Radiol 2008;12:42-53.ArticlePubMed
- 13. Hsu CY, Wu CM, Lin SW, Cheng KL. Anterior superior iliac spine avulsion fracture presenting as meralgia paraesthetica in an adolescent sprinter. J Rehabil Med 2014;46:188-90.ArticlePubMed
- 14. Thanikachalam M, Petros JG, O’Donnell S. Avulsion fracture of the anterior superior iliac spine presenting as acute-onset meralgia paresthetica. Ann Emerg Med 1995;26:515-7.ArticlePubMed
- 15. Dhinsa BS, Jalgaonkar A, Mann B, Butt S, Pollock R. Avulsion fracture of the anterior superior iliac spine: misdiagnosis of a bone tumour. J Orthop Traumatol 2011;12:173-6.ArticlePubMedPMC
- 16. Akhter F, Ayeni O, Almasri M. ASIS avulsion fracture repair with lag screw and tape bridge construct. Arthrosc Tech 2022;11:e875-80.ArticlePubMedPMC
- 17. Anduaga I, Seijas R, Pérez-Bellmunt A, Casasayas O, Alvarez P. Anterior iliac spine avulsion fracture treatment options in young athletes. J Invest Surg 2020;33:159-63.ArticlePubMed
- 18. Kautzner J, Trc T, Havlas V. Comparison of conservative against surgical treatment of anterior-superior iliac spine avulsion fractures in children and adolescents. Int Orthop 2014;38:1495-8.ArticlePubMedPMCPDF
- 19. Willinger L, Schanda JE, Lorenz S, Imhoff AB, Buchmann S. Surgical treatment of two adolescent athletes with dislocated avulsion fracture of the anterior superior iliac spine (ASIS). Arch Orthop Trauma Surg 2017;137:173-7.ArticlePubMedPDF
- 20. Cimerman M, Smrkolj V, Veselko M. Avulsion of the anterior superior iliac spine in two adolescent sisters: operative versus conservative treatment. Unfallchirurg 1995;98:530-1.PubMed
- 21. Wirth T. Apophyseal avulsions of the hip region in adolescents. Orthopade 2016;45:213-8.PubMed
- 22. Novais EN, Riederer MF, Provance AJ. Anterior inferior iliac spine deformity as a cause for extra-articular hip impingement in young athletes after an avulsion fracture: a case report. Sports Health 2018;10:272-6.ArticlePubMedPDF
- 23. Maalouly J, Aouad D, Ayoubi R, et al. Anterior inferior iliac spine avulsion fracture post hip arthroscopy for Femoroacetabular impingement. Trauma Case Rep 2020;29:100342.ArticlePubMedPMC
- 24. Yeager KC, Silva SR, Richter DL. Pelvic avulsion injuries in the adolescent athlete. Clin Sports Med 2021;40:375-84.ArticlePubMed
- 25. Hsu JC, Fischer DA, Wright RW. Proximal rectus femoris avulsions in national football league kickers: a report of 2 cases. Am J Sports Med 2005;33:1085-7.ArticlePubMedPDF
- 26. Gamradt SC, Brophy RH, Barnes R, Warren RF, Thomas Byrd JW, Kelly BT. Nonoperative treatment for proximal avulsion of the rectus femoris in professional American football. Am J Sports Med 2009;37:1370-4.ArticlePubMedPDF
- 27. Irmola T, Heikkilä JT, Orava S, Sarimo J. Total proximal tendon avulsion of the rectus femoris muscle. Scand J Med Sci Sports 2007;17:378-82.ArticlePubMed
- 28. Kujala UM, Orava S, Karpakka J, Leppävuori J, Mattila K. Ischial tuberosity apophysitis and avulsion among athletes. Int J Sports Med 1997;18:149-55.ArticlePubMed
- 29. Bahk WJ, Brien EW, Luck JV Jr, Mirra JM. Avulsion of the ischial tuberosity simulating neoplasm: a report of 2 cases. Acta Orthop Scand 2000;71:211-4.ArticlePubMed
- 30. Ferlic PW, Sadoghi P, Singer G, Kraus T, Eberl R. Treatment for ischial tuberosity avulsion fractures in adolescent athletes. Knee Surg Sports Traumatol Arthrosc 2014;22:893-7.ArticlePubMedPDF
- 31. Schiller J, DeFroda S, Blood T. Lower extremity avulsion fractures in the pediatric and adolescent athlete. J Am Acad Orthop Surg 2017;25:251-9.ArticlePubMed
- 32. Miller A, Stedman GH, Beisaw NE, Gross PT. Sciatica caused by an avulsion fracture of the ischial tuberosity: a case report. J Bone Joint Surg Am 1987;69:143-5.ArticlePubMed
- 33. Hayat Z, Konan S, Pollock R. Ischiofemoral impingement resulting from a chronic avulsion injury of the hamstrings. BMJ Case Rep 2014;2014:bcr2014204017.ArticlePubMedPMC
- 34. Robinson P, Salehi F, Grainger A, et al. Cadaveric and MRI study of the musculotendinous contributions to the capsule of the symphysis pubis. AJR Am J Roentgenol 2007;188:W440-5.ArticlePubMed
- 35. Serner A, Weir A, Tol JL, et al. Characteristics of acute groin injuries in the adductor muscles: a detailed MRI study in athletes. Scand J Med Sci Sports 2018;28:667-76.PubMed
- 36. Wiley JJ. Traumatic osteitis pubis: the gracilis syndrome. Am J Sports Med 1983;11:360-63.ArticlePubMedPDF
- 37. Schneider R, Kaye J, Ghelman B. Adductor avulsive injuries near the symphisis pubis. Radiology 1976;120:567-9.ArticlePubMed
- 38. Serner A, Tol JL, Jomaah N, et al. Diagnosis of acute groin injuries: a prospective study of 110 athletes. Am J Sports Med 2015;43:1857-64.ArticlePubMedPDF
- 39. Serner A, Roemer FW, Hölmich P, et al. Reliability of MRI assessment of acute musculotendinous groin injuries in athletes. Eur Radiol 2017;27:1486-95.ArticlePubMedPDF
- 40. Wong-On M, Turmo-Garuz A, Arriaza R, et al. Injuries of the obturator muscles in professional soccer players. Knee Surg Sports Traumatol Arthrosc 2018;26:1936-42.ArticlePubMedPDF
- 41. Walsh PJ, Farooq M, Walz DM. Occult fracture propagation in patients with isolated greater trochanteric fractures: patterns and management. Skeletal Radiol 2022;51:1391-8.ArticlePubMedPDF
- 42. Freitas A, Macedo SL Sr. Apophyseal fracture or avulsion of the greater trochanter. Acta Ortop Bras 2016;24:164-6.ArticlePubMedPMC
- 43. Kaweblum M, Lehman WB, Grant AD, Strongwater A.. Avascular necrosis of the femoral head as sequela of fracture of the greater trochanter: a case report and review of the literature. Clin Orthop Relat Res 1993;(294):193-5.
- 44. O’Rourke MR, Weinstein SL. Osteonecrosis following isolated avulsion fracture of the greater trochanter in children: a report of two cases. J Bone Joint Surg Am 2003;85:2000-5.PubMed
- 45. Khalifa MA, Alaya Z, Hassini L, Bouattour K, Osman W, Ben Ayèche ML. Ipsilateral open anterior hip dislocation and avulsion fracture of the greater trochanter: an unusual case report. Arch Pediatr 2019;26:422-5.ArticlePubMed
- 46. Giles E, Henderson S, Halim A, Smith BG, Milewski MD. Apophyseal avulsion of the greater trochanter in an adolescent: treatment with abduction bracing: a case report. JBJS Case Connect 2016;6:e47. PubMed
- 47. Memminger MK. Avulsion fracture of the trochanter minor in the adolescent. Acta Biomed 2018;90(1-S):175-6.PubMed
- 48. Tahir T, Manzoor QW, Gul IA, Bhat SA, Kangoo KA. Isolated avulsion fractures of lesser trochanter in adolescents: a case series and brief literature review. J Orthop Case Rep 2019;9:11-4.
- 49. McMillan T, Rehman H, Mitchell M. Lesser trochanter avulsion fracture in an adolescent after seizure. J Emerg Med 2016;51:457-60.ArticlePubMed
- 50. Afra R, Boardman DL, Kabo JM, Eckardt JJ. Avulsion fracture of the lesser trochanter as a result of a preliminary malignant tumor of bone: a report of four cases. J Bone Joint Surg Am 1999;81:1299-304.PubMed
- 51. Cho HS, Lee YK, Yoon BH, Park JW, Ha YC, Koo KH. Isolated avulsion fracture of the lesser trochanter in adults. In Vivo 2020;34:3519-26.ArticlePubMedPMC
- 52. Linni K, Mayr J, Höllwarth ME. Apophyseal fractures of the pelvis and trochanter minor in 20 adolescents and 2 young children. Unfallchirurg 2000;103:961-4.PubMed
- 53. Ruffing T, Rückauer T, Bludau F, Hofmann A, Muhm M, Suda AJ. Avulsion fracture of the lesser trochanter in adolescents. Injury 2018;49:1278-81.ArticlePubMed
- 54. Miyake Y, Mitani S, Namba Y, Kikuoka R. An avulsion fracture of the lesser trochanter of the femur with prodromal symptoms in an adult: a case report and review of literature. J Orthop Case Rep 2022;12:1-4.Article
- 55. Anderson K, Strickland SM, Warren R. Hip and groin injuries in athletes. Am J Sports Med 2001;29:521-33.ArticlePubMedPDF
- 56. Quarrier NF, Wightman AB. A ballet dancer with chronic hip pain due to a lesser trochanter bony avulsion: the challenge of a differential diagnosis. J Orthop Sports Phys Ther 1998;28:168-73.ArticlePubMed
- 57. Khemka A, Raz G, Bosley B, Ludger G, Al Muderis M. Arthroscopically assisted fixation of the lesser trochanter fracture: a case series. J Hip Preserv Surg 2014;1:27-32.ArticlePubMedPMC
 , Yonghan Cha, MD1
, Yonghan Cha, MD1 , Jung-Taek Kim, MD2
, Jung-Taek Kim, MD2 , Jun-Il Yoo, MD3
, Jun-Il Yoo, MD3 , Jin-Woo Kim, MD4
, Jin-Woo Kim, MD4









 E-submission
E-submission KOTA
KOTA TOTA
TOTA TOTS
TOTS
 ePub Link
ePub Link Cite
Cite

