Articles
- Page Path
- HOME > J Musculoskelet Trauma > Volume 38(2); 2025 > Article
-
Review Article
- Treatment of avulsion fractures around the knee
-
Jeong-Hyun Koh, MD
 , Hyung Keun Song, MD, PhD
, Hyung Keun Song, MD, PhD , Won-Tae Cho, MD
, Won-Tae Cho, MD , Seungyeob Sakong, MD
, Seungyeob Sakong, MD , Sumin Lim, MD, PhD
, Sumin Lim, MD, PhD
-
Journal of Musculoskeletal Trauma 2025;38(2):63-73.
DOI: https://doi.org/10.12671/jmt.2025.00073
Published online: March 31, 2025
Department of Orthopedic Surgery, Ajou University School of Medicine, Suwon, Korea
- Correspondence to: Sumin Lim, MD, PhD Department of Orthopedic Surgery, Ajou University School of Medicine, 206 World cup-ro, Yeongtong-gu, Suwon 16499, Korea Tel: +82-31-219-5220 Email: khoo1003@aumc.ac.kr
© 2025 The Korean Fracture Society
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 29,533 Views
- 259 Download
- 1 Crossref
- Abstract
- Introduction
- Anterior Cruciate Ligament Avulsion Fracture
- Posterior Cruciate Ligament Avulsion Fracture
- Segond Fracture
- Iliotibial Band Avulsion Fracture
- Medial Collateral Ligament Avulsion Fracture
- Arcuate Ligament Avulsion Fracture
- Medial Patellofemoral Ligament Avulsion Fracture
- Patella Tendon, Quadriceps Tendon Avulsion Fracture
- Conclusions
- Article Information
- REFERENCES
Abstract
- Avulsion fractures of the knee occur when tensile forces cause a bone fragment to separate at the site of soft tissue attachment. These injuries, which frequently affect adolescent athletes, can involve the cruciate and collateral ligaments, arcuate complex, iliotibial band, and patellar and quadriceps tendons. Radiographs aid in the initial diagnosis, while computed tomography and magnetic resonance imaging facilitate a comprehensive evaluation of injury severity and concomitant damage. Specific avulsion fracture types include: anterior cruciate ligament avulsions (tibial site, Meyers and McKeever classification), posterior cruciate ligament avulsions (tibial attachment, Griffith's classification), Segond fractures (anterolateral complex injury), iliotibial band avulsions, medial collateral ligament avulsions (reverse Segond, Stieda fractures), arcuate complex avulsions (arcuate sign), medial patellofemoral avulsions (patellar dislocations), and patellar/quadriceps tendon avulsions. The treatment depends on the fracture location, displacement, and associated injuries. Nondisplaced fractures can be managed conservatively, while displaced fractures or those with instability require surgical reduction and fixation. Prompt recognition and appropriate intervention prevent complications such as deformity, nonunion, malunion, and residual instability. This review provides an overview of the pathogenesis, diagnosis, and management of knee avulsion fractures to guide clinical decision-making.
Introduction
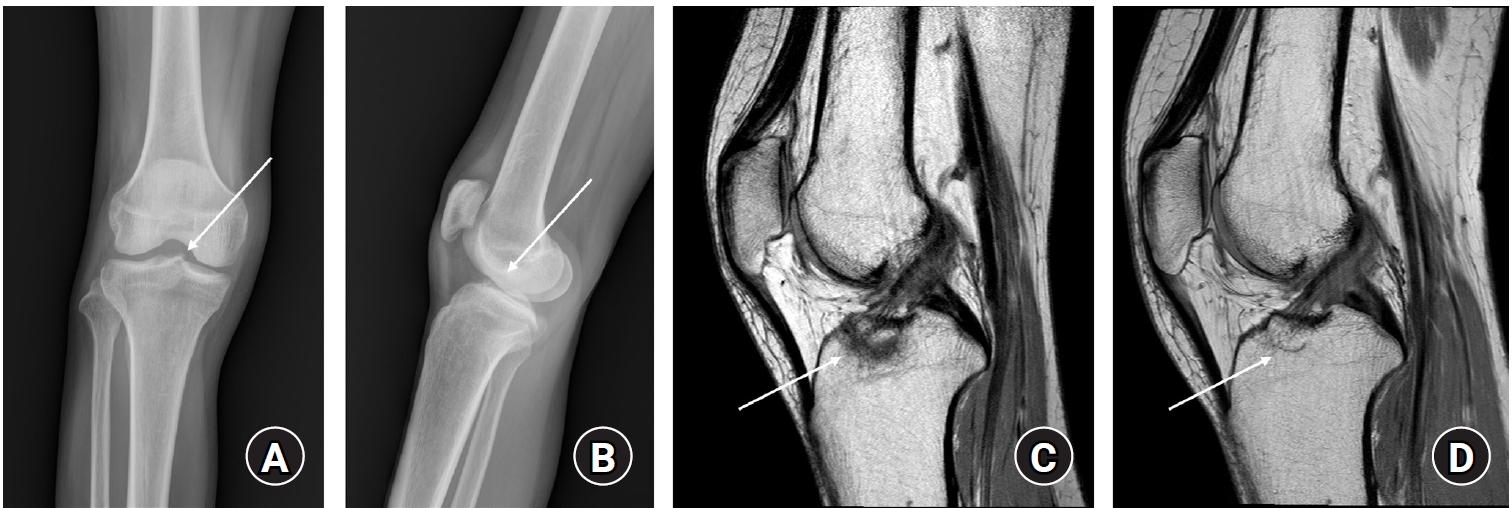
Anterior Cruciate Ligament Avulsion Fracture
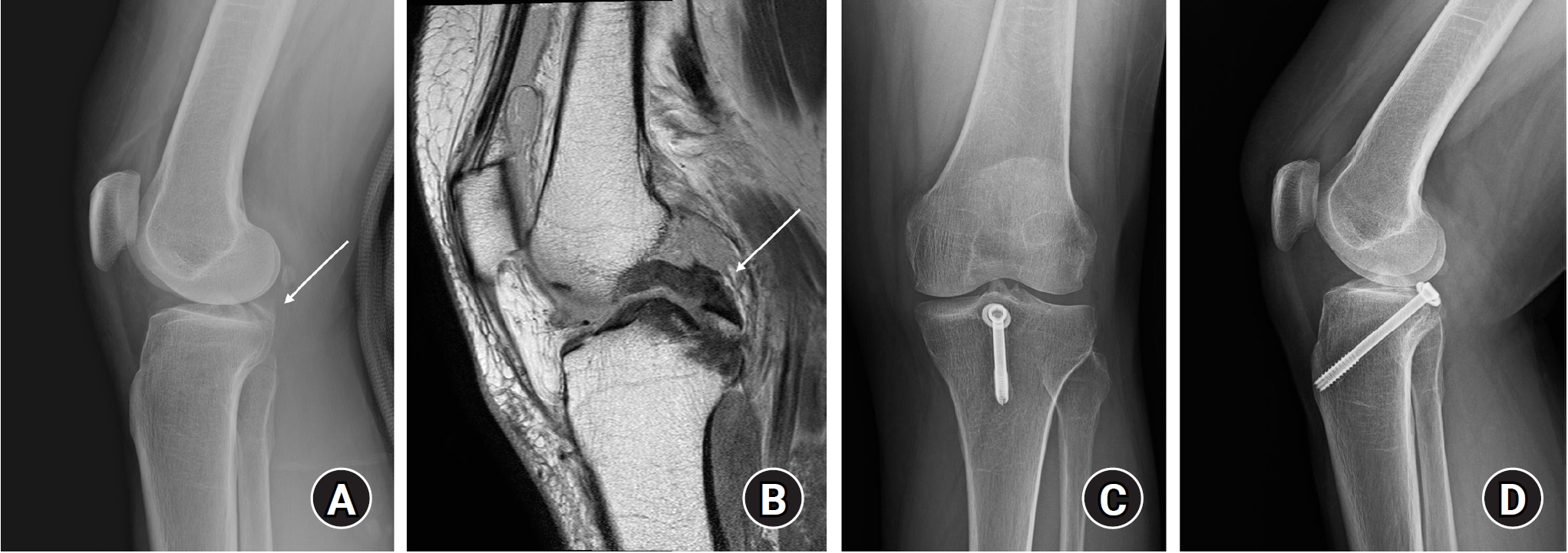
Posterior Cruciate Ligament Avulsion Fracture
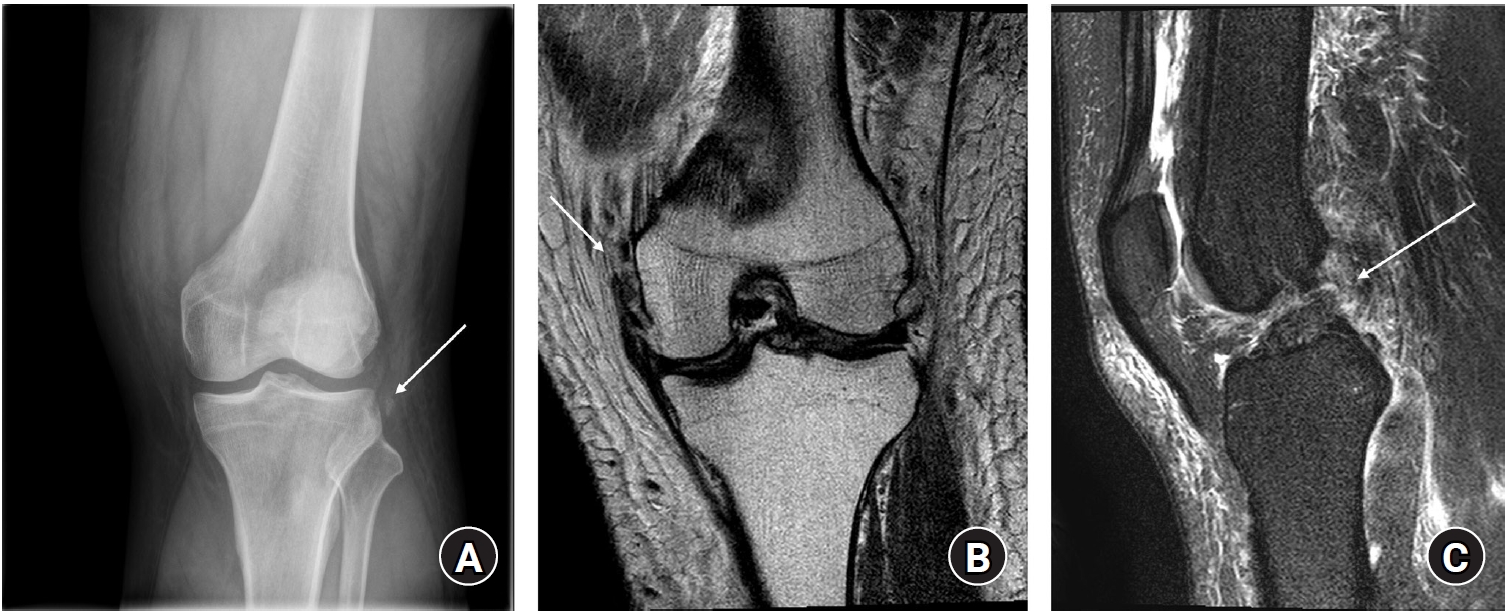
Segond Fracture
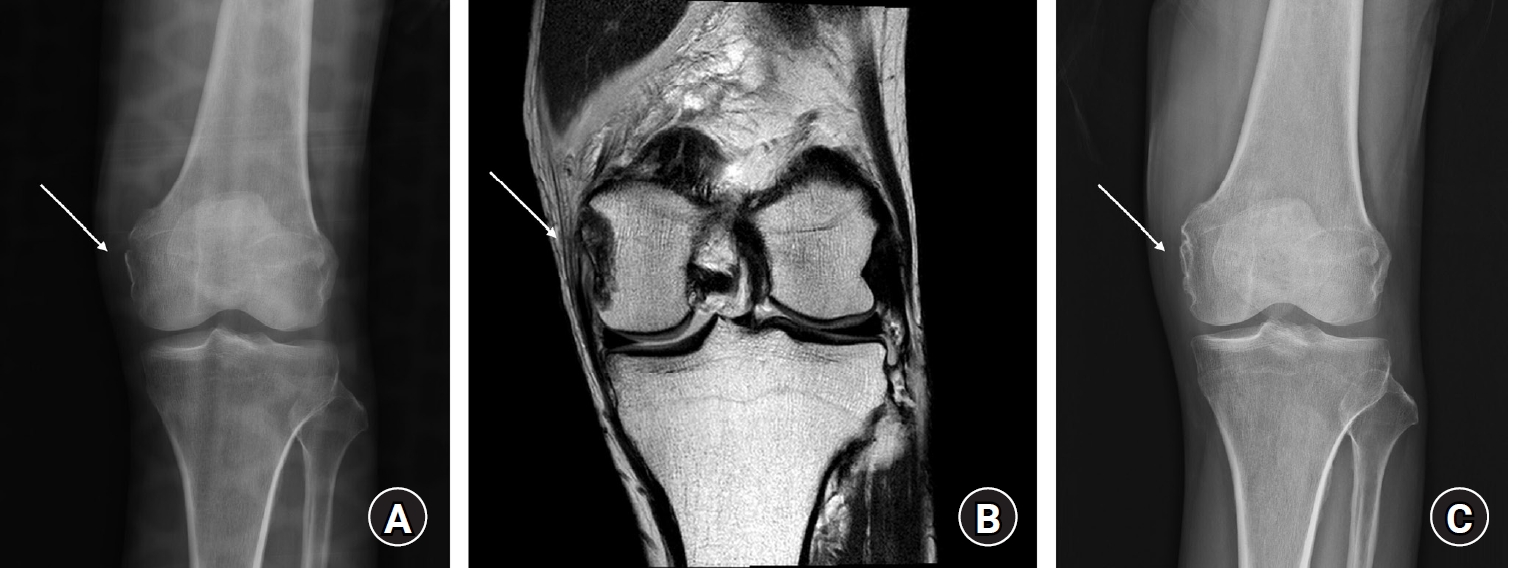
Iliotibial Band Avulsion Fracture
Medial Collateral Ligament Avulsion Fracture
Arcuate Ligament Avulsion Fracture
Medial Patellofemoral Ligament Avulsion Fracture
Patella Tendon, Quadriceps Tendon Avulsion Fracture
Conclusions
-
Author contributions
Conceptualization: SL, HKS. Investigation: JHK, SS, SL. Methodology: HKS. Supervision: HKS, WTC, SL. Writing-original draft: JHK, HKS, WTC, SS, SL. Writing-review & editing: JHK, HKS, WTC, SS, SL. All authors read and approved the final manuscript.
-
Conflict of interests
Hyung Keun Song is a managing editor of the journal but was not involved in the peer reviewer selection, evaluation, or decision process of this article. No other potential conflicts of interest relevant to this article were reported.
-
Funding
None.
-
Data availability
Not applicable.
Article Information
- 1. McCoy JS, Nelson R. Avulsion fractures [Internet]. StatPearls Publishing; [cited 2025 Feb 10]. Available from: https://pubmed.ncbi.nlm.nih.gov/32644594/.
- 2. Stevens MA, El-Khoury GY, Kathol MH, Brandser EA, Chow S. Imaging features of avulsion injuries. Radiographics 1999;19:655-72.ArticlePubMed
- 3. Beckett R, Le P, Rheinboldt M, Petraszko A. Avulsion fractures of the knee: a review of the pathophysiology, radiographic, and cross-sectional imaging features. Emerg Radiol 2019;26:683-9.ArticlePubMedPDF
- 4. Marupaka SK, Kataria S, Jakkani R, Jampala V, Chavva S. Avulsion fractures around the knee and their importance. Int J Contemp Med Surg Radiol 2019;4:C241-7.Article
- 5. Gottsegen CJ, Eyer BA, White EA, Learch TJ, Forrester D. Avulsion fractures of the knee: imaging findings and clinical significance. Radiographics 2008;28:1755-70.ArticlePubMed
- 6. White EA, Patel DB, Matcuk GR, et al. Cruciate ligament avulsion fractures: anatomy, biomechanics, injury patterns, and approach to management. Emerg Radiol 2013;20:429-40.ArticlePubMedPDF
- 7. Duthon VB, Barea C, Abrassart S, Fasel JH, Fritschy D, Menetrey J. Anatomy of the anterior cruciate ligament. Knee Surg Sports Traumatol Arthrosc 2006;14:204-13.ArticlePubMedPDF
- 8. Beynnon BD, Fleming BC, Labovitch R, Parsons B. Chronic anterior cruciate ligament deficiency is associated with increased anterior translation of the tibia during the transition from non-weightbearing to weightbearing. J Orthop Res 2002;20:332-7.ArticlePubMed
- 9. Brandsma AS, Goedhart LM, van Raaij JJ. An avulsion fracture of the anterior cruciate ligament attachment to the lateral femoral condyle in an elderly patient: a rare finding. J Surg Case Rep 2020;2020:rjaa054.PubMedPMC
- 10. Murrell GA, Maddali S, Horovitz L, Oakley SP, Warren RF. The effects of time course after anterior cruciate ligament injury in correlation with meniscal and cartilage loss. Am J Sports Med 2001;29:9-14.ArticlePubMedPDF
- 11. Zhao J, Huangfu X. Arthroscopic treatment of nonunited anterior cruciate ligament tibial avulsion fracture with figure-of-8 suture fixation technique. Arthroscopy 2007;23:405-10.ArticlePubMed
- 12. Baums MH, Klinger HM, Harer T. Treatment of malunited fractures of the anterior tibial spine. Knee Surg Sports Traumatol Arthrosc 2004;12:159-61.ArticlePubMedPDF
- 13. Mitchell JJ, Sjostrom R, Mansour AA, et al. Incidence of meniscal injury and chondral pathology in anterior tibial spine fractures of children. J Pediatr Orthop 2015;35:130-5.ArticlePubMed
- 14. Meyers MH, McKeever FM. Fracture of the intercondylar eminence of the tibia. J Bone Joint Surg Am 1970;52:1677-84.ArticlePubMed
- 15. Chang CJ, Huang TC, Hoshino Y, et al. Functional outcomes and subsequent surgical procedures after arthroscopic suture versus screw fixation for ACL tibial avulsion fractures: a systematic review and meta-analysis. Orthop J Sports Med 2022;10:23259671221085945.ArticlePubMedPMCPDF
- 16. Lu XW, Hu XP, Jin C, Zhu T, Ding Y, Dai LY. Reduction and fixation of the avulsion fracture of the tibial eminence using mini-open technique. Knee Surg Sports Traumatol Arthrosc 2010;18:1476-80.ArticlePubMedPDF
- 17. Chandrasekaran S, Ma D, Scarvell JM, Woods KR, Smith PN. A review of the anatomical, biomechanical and kinematic findings of posterior cruciate ligament injury with respect to non-operative management. Knee 2012;19:738-45.ArticlePubMed
- 18. Hooper PO 3rd, Silko C, Malcolm TL, Farrow LD. Management of posterior cruciate ligament tibial avulsion injuries: a systematic review. Am J Sports Med 2018;46:734-42.ArticlePubMedPDF
- 19. Katsman A, Strauss EJ, Campbell KA, Alaia MJ. Posterior cruciate ligament avulsion fractures. Curr Rev Musculoskelet Med 2018;11:503-9.ArticlePubMedPMCPDF
- 20. Margheritini F, Mancini L, Mauro CS, Mariani PP. Stress radiography for quantifying posterior cruciate ligament deficiency. Arthroscopy 2003;19:706-11.ArticlePubMed
- 21. Pardiwala DN, Agrawal D, Patil V, Saini U, Dhawal P. Paper 133: comparison of open versus arthroscopic fixation for isolated PCL tibial bony avulsions: a prospective randomized study with minimum 2 year follow-up. Arthroscopy 2012;28:e413-4.Article
- 22. Gross ML, Grover JS, Bassett LW, Seeger LL, Finerman GA. Magnetic resonance imaging of the posterior cruciate ligament: clinical use to improve diagnostic accuracy. Am J Sports Med 1992;20:732-7.ArticlePubMedPDF
- 23. Sonin AH, Fitzgerald SW, Hoff FL, Friedman H, Bresler ME. MR imaging of the posterior cruciate ligament: normal, abnormal, and associated injury patterns. Radiographics 1995;15:551-61.ArticlePubMed
- 24. Zhao J, He Y, Wang J. Arthroscopic treatment of acute tibial avulsion fracture of the posterior cruciate ligament with suture fixation technique through Y-shaped bone tunnels. Arthroscopy 2006;22:172-81.ArticlePubMed
- 25. Yoon KH, Kim SG, Park JY. The amount of displacement can determine non-operative treatment in posterior cruciate ligament avulsion fracture. Knee Surg Sports Traumatol Arthrosc 2021;29:1269-75.ArticlePubMedPDF
- 26. Griffith JF, Antonio GE, Tong CW, Ming CK. Cruciate ligament avulsion fractures. Arthroscopy 2004;20:803-12.ArticlePubMed
- 27. Segond PF. Recherches cliniques et experimentales sur les epanchements sanguins du genou par entorse. Aux Bureaux du Progres Medical; 1879.
- 28. Kaplan EB. The iliotibial tract: clinical and morphological significance. J Bone Joint Surg Am 1958;40:817-32.
- 29. Terry GC, Hughston JC, Norwood LA. The anatomy of the iliopatellar band and iliotibial tract. Am J Sports Med 1986;14:39-45.ArticlePubMedPDF
- 30. Claes S, Vereecke E, Maes M, Victor J, Verdonk P, Bellemans J. Anatomy of the anterolateral ligament of the knee. J Anat 2013;223:321-8.ArticlePubMedPMCPDF
- 31. Getgood A, Brown C, Lording T, et al. The anterolateral complex of the knee: results from the International ALC Consensus Group Meeting. Knee Surg Sports Traumatol Arthrosc 2019;27:166-76.ArticlePubMedPDF
- 32. Woods GW, Stanley RF, Tullos HS. Lateral capsular sign: x-ray clue to a significant knee instability. Am J Sports Med 1979;7:27-33.ArticlePubMedPDF
- 33. Goldman AB, Pavlov H, Rubenstein D. The Segond fracture of the proximal tibia: a small avulsion that reflects major ligamentous damage. AJR Am J Roentgenol 1988;151:1163-7.ArticlePubMed
- 34. Melugin HP, Johnson NR, Wu IT, Levy BA, Stuart MJ, Krych AJ. Is treatment of Segond fracture necessary with combined anterior cruciate ligament reconstruction. Am J Sports Med 2018;46:832-8.ArticlePubMedPDF
- 35. Dietz GW, Wilcox DM, Montgomery JB. Segond tibial condyle fracture: lateral capsular ligament avulsion. Radiology 1986;159:467-9.ArticlePubMed
- 36. Weber WN, Neumann CH, Barakos JA, Petersen SA, Steinbach LS, Genant HK. Lateral tibial rim (Segond) fractures: MR imaging characteristics. Radiology 1991;180:731-4.ArticlePubMed
- 37. Sulaiman Y, Li J, Chen G, Abudouaini H, Li Q, Tang X. The relationship between a Segond fracture and meniscus injury in patients with anterior cruciate ligament tears. Knee 2021;33:193-9.ArticlePubMed
- 38. Slagstad I, Parkar AP, Strand T, Inderhaug E. Incidence and prognostic significance of the Segond fracture in patients undergoing anterior cruciate ligament reconstruction. Am J Sports Med 2020;48:1063-8.ArticlePubMedPMCPDF
- 39. Lau BC, Rames J, Belay E, Riboh JC, Amendola A, Lassiter T. Anterolateral complex reconstruction augmentation of anterior cruciate ligament reconstruction: biomechanics, indications, techniques, and clinical outcomes. JBJS Rev 2019;7:e5. ArticlePubMedPMC
- 40. Garcia-Mansilla I, Zicaro JP, Martinez EF, Astoul J, Yacuzzi C, Costa-Paz M. Overview of the anterolateral complex of the knee. World J Clin Cases 2022;10:8474-81.ArticlePubMedPMC
- 41. Sabatini L, Capella M, Vezza D, et al. Anterolateral complex of the knee: state of the art. World J Orthop 2022;13:679-92.ArticlePubMedPMC
- 42. Phua SK, Lim JY, Li T, Ho SW. The Segond fracture: a narrative review of the anatomy, biomechanics and clinical implications. J Clin Orthop Trauma 2023;38:102127.ArticlePubMedPMC
- 43. Nagai K, Kamada K, Kay J, et al. Clinical outcomes after anterior cruciate ligament reconstruction in patients with a concomitant Segond fracture: a systematic review. Am J Sports Med 2023;51:525-33.ArticlePubMedPDF
- 44. Hutchinson LA, Lichtwark GA, Willy RW, Kelly LA. The iliotibial band: a complex structure with versatile functions. Sports Med 2022;52:995-1008.ArticlePubMedPMCPDF
- 45. Hayes CW, Brigido MK, Jamadar DA, Propeck T. Mechanism-based pattern approach to classification of complex injuries of the knee depicted at MR imaging. Radiographics 2000;20 Spec No:S121-34.ArticlePubMed
- 46. Khetan V, Sabnis B, Usman S, Joshi A. An unusual case of isolated iliotibial band avulsion fracture. J Arthrosc Surg Sport Med 2021;2:119-23.Article
- 47. Haims AH, Medvecky MJ, Pavlovich R Jr, Katz LD. MR imaging of the anatomy of and injuries to the lateral and posterolateral aspects of the knee. AJR Am J Roentgenol 2003;180:647-53.ArticlePubMed
- 48. Stevens KJ, Albtoush OM, Lutz AM. The Stieda fracture revisited. Skeletal Radiol 2021;50:945-53.ArticlePubMedPDF
- 49. Stieda A. Uber eine typische verletzung am unteren femurende. Archiv klin Chir 1908;85:815-26.
- 50. Hall FM, Hochman MG. Medial Segond-type fracture: cortical avulsion off the medial tibial plateau associated with tears of the posterior cruciate ligament and medial meniscus. Skeletal Radiol 1997;26:553-5.ArticlePubMedPDF
- 51. Kose O, Ozyurek S, Turan A, Guler F. Reverse Segond fracture and associated knee injuries: a case report and review of 13 published cases. Acta Orthop Traumatol Turc 2016;50:587-91.ArticlePubMedPMC
- 52. Guo D, Yu H, Huang B, Gao X, Qin Y, Liu X. Avulsion of the femoral attachment of the medial collateral ligament in the setting of knee multiligament injury: a case report. Medicine (Baltimore) 2019;98:e18376. PubMedPMC
- 53. Haddad S, Sallent A, Minguell J, Castellet E. Avulsion of the femoral attachment of the medial collateral ligament of the knee associated to complete tear of the posterior cruciate ligament: a case report. Surg J (N Y) 2017;3:e38-41.ArticlePubMedPMC
- 54. Angelini FJ, Malavolta EA, D'Elia CO, Pecora JR, Hernandez A, Camanho GL. Avulsion fracture of the medial tibial plateau (reverse Segond injury). Acta Ortop Bras 2007;15:169-70.Article
- 55. Kwon OS, Park MJ, Tjoumakaris FP. Medial and lateral segond fractures in a skeletally immature patient: a radiographic marker for the multiply injured knee. Orthopedics 2011;34:e772-5.ArticlePubMed
- 56. Shindell R, Walsh WM, Connolly JF. Avulsion fracture of the fibula: the ‘arcuate sign’ of posterolateral knee instability. Nebr Med J 1984;69:369-71.PubMed
- 57. Lee J, Papakonstantinou O, Brookenthal KR, Trudell D, Resnick DL. Arcuate sign of posterolateral knee injuries: anatomic, radiographic, and MR imaging data related to patterns of injury. Skeletal Radiol 2003;32:619-27.ArticlePubMedPDF
- 58. LaPrade RF, Ly TV, Wentorf FA, Engebretsen L. The posterolateral attachments of the knee: a qualitative and quantitative morphologic analysis of the fibular collateral ligament, popliteus tendon, popliteofibular ligament, and lateral gastrocnemius tendon. Am J Sports Med 2003;31:854-60.PubMed
- 59. Dietrich G, Maeder B, Nyland J, Maeder Y, Akiki A, Martin R. Isolated femoral LCL avulsion fracture in the adult knee: two patient cases and literature review. Case Rep Orthop 2022;2022:6507577.ArticlePubMedPMCPDF
- 60. Huang GS, Yu JS, Munshi M, et al. Avulsion fracture of the head of the fibula (the “arcuate” sign): MR imaging findings predictive of injuries to the posterolateral ligaments and posterior cruciate ligament. AJR Am J Roentgenol 2003;180:381-7.ArticlePubMed
- 61. Spadafore S, Khodaee M. Avulsion fracture of the proximal fibula (arcuate sign) in a young woman. BMJ Case Rep 2020;13:e237368. ArticlePubMedPMC
- 62. Chahla J, Moatshe G, Dean CS, LaPrade RF. Posterolateral corner of the knee: current concepts. Arch Bone Jt Surg 2016;4:97-103.PubMedPMC
- 63. Gupta R, Singh J, Khatri K, Bither N. Common peroneal nerve laceration in closed fibular head avulsion fracture: a case report. J Orthop Case Rep 2016;6:23.PubMed
- 64. Oh HK, Kim JH, Lee CS, Singh PK, Wang KH, Nha KW. Isolated avulsion fracture of the fibular head: a new fixation technique using a suture anchor. Orthopedics 2011;34:100-4.ArticlePubMed
- 65. Sharma B, Parmar RS, Kapoor K, Kumar N, Verma R. a prospective study of rare entity. Int J Orthop Sci 2017;3(3j):677-82.Article
- 66. Kim JM, Park BM, Lee SH, Jeon SJ, Shin JB, Song KS. Surgical management of comminuted avulsion fracture of the proximal fibula with lateral collateral ligament injury: technical note. J Korean Fract Soc 2013;26:77-80.Article
- 67. Elias DA, White LM, Fithian DC. Acute lateral patellar dislocation at MR imaging: injury patterns of medial patellar soft-tissue restraints and osteochondral injuries of the inferomedial patella. Radiology 2002;225:736-43.ArticlePubMed
- 68. Sillanpää PJ, Salonen E, Pihlajamäki H, Mäenpää HM. Medial patellofemoral ligament avulsion injury at the patella: classification and clinical outcome. Knee Surg Sports Traumatol Arthrosc 2014;22:2414-8.ArticlePubMedPDF
- 69. Guerrero P, Li X, Patel K, Brown M, Busconi B. Medial patellofemoral ligament injury patterns and associated pathology in lateral patella dislocation: an MRI study. Sports Med Arthrosc Rehabil Ther Technol 2009;1:17.ArticlePubMedPMCPDF
- 70. Sillanpää PJ, Peltola E, Mattila VM, Kiuru M, Visuri T, Pihlajamäki H. Femoral avulsion of the medial patellofemoral ligament after primary traumatic patellar dislocation predicts subsequent instability in men: a mean 7-year nonoperative follow-up study. Am J Sports Med 2009;37:1513-21.ArticlePubMedPDF
- 71. Danielsen O, Poulsen TA, Eysturoy NH, Mortensen ES, Holmich P, Barfod KW. Trochlea dysplasia, increased TT-TG distance and patella alta are risk factors for developing first-time and recurrent patella dislocation: a systematic review. Knee Surg Sports Traumatol Arthrosc 2023;31:3806-46.ArticlePubMedPDF
- 72. Palmu S, Kallio PE, Donell ST, Helenius I, Nietosvaara Y. Acute patellar dislocation in children and adolescents: a randomized clinical trial. J Bone Joint Surg Am 2008;90:463-70.ArticlePubMed
- 73. Nikku R, Nietosvaara Y, Aalto K, Kallio PE. Operative treatment of primary patellar dislocation does not improve medium-term outcome: a 7-year follow-up report and risk analysis of 127 randomized patients. Acta Orthop 2005;76:699-704.PubMed
- 74. Sillanpaa PJ, Mattila VM, Maenpaa H, Kiuru M, Visuri T, Pihlajamäki H. Treatment with and without initial stabilizing surgery for primary traumatic patellar dislocation: a prospective randomized study. J Bone Joint Surg Am 2009;91:263-73.PubMed
- 75. Scolaro J, Bernstein J, Ahn J. Patellar fractures. Clin Orthop Relat Res 2011;469:1213-5.PubMed
- 76. Potla R, Williamson T, Ramlatchan SR, Mangal RK, Ganti L. Patellar avulsion fracture. Cureus 2023;15:e46695. ArticlePubMedPMC
- 77. Bradko V, Stoll WT, Haruno LS, Rosenfeld SB, McKay SD. Two cases of combined patellar tendon avulsion from the tibia and patella. SICOT J 2018;4:17.ArticlePubMedPMC
- 78. Gwinner C, Märdian S, Schwabe P, Schaser KD, Krapohl BD, Jung TM. Current concepts review: fractures of the patella. GMS Interdiscip Plast Reconstr Surg DGPW 2016;5:Doc01.PubMedPMC
- 79. Shimasaki K, Uesugi M, Kobayashi T, Tanaka H, Ichimura H. Inferior pole sleeve fracture of the patella in an adolescent: a case report. Cureus 2023;15:e33494. ArticlePubMedPMC
REFERENCES
Figure & Data
REFERENCES
Citations

- Lateral marginal fractures of the patella and patellofemoral pain
Jae-Ang Sim, Chul-Ho Kim, Ji Wan Kim
Journal of Musculoskeletal Trauma.2025; 38(3): 152. CrossRef





 E-submission
E-submission KOTA
KOTA TOTA
TOTA TOTS
TOTS
 ePub Link
ePub Link Cite
Cite

