Articles
- Page Path
- HOME > J Musculoskelet Trauma > Volume 39(2); 2026 > Article
-
Review Article
- Nonoperative management of distal radius fractures: when and how?
- Shin Woo Choi1, Jae Kwang Kim2
-
Journal of Musculoskeletal Trauma 2026;39(2):93-102.
DOI: https://doi.org/10.12671/jmt.2026.00024
Published online: March 10, 2026
1Department of Orthopedic Surgery, Gangneung Asan Hospital, University of Ulsan College of Medicine, Gangneung, Korea
2Department of Orthopedic Surgery, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
- Correspondence to: Jae Kwang Kim Department of Orthopedic Surgery, Asan Medical Center, University of Ulsan College of Medicine, 88 Olympic-ro 43-gil, Songpa-gu, Seoul 05505, Korea Tel: +82-2-3010-3523, Email: orth4535@gmail.com
© 2026 The Korean Orthopaedic Trauma Association
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 827 Views
- 5 Download
Abstract
- Distal radius fractures are among the most common injuries of the upper extremity, particularly in the elderly population. Although the use of volar locking plate fixation has increased in recent years, evidence from randomized and prospective studies demonstrates that, while operative treatment may achieve superior radiographic alignment and enable more rapid early recovery, these advantages tend to diminish over time and do not result in superior long-term patient-reported functional outcomes in elderly patients. In addition, radiographic parameters show only a limited correlation with functional recovery. Consequently, nonoperative treatment remains a valid and important treatment option for distal radius fractures. The decision to pursue nonoperative management should be based on a comprehensive assessment of radiographic parameters—including dorsal tilt, radial shortening, and intraarticular displacement—together with patient-specific factors such as age, activity level, comorbidities, and functional expectations. For stable or minimally displaced fractures, an immobilization period of 3‒4 weeks is generally recommended, whereas displaced fractures typically require immobilization for 5‒6 weeks. In cases requiring manual reduction, traditional treatment protocols recommend weekly radiographic follow-up during the first 2‒3 weeks to monitor for secondary displacement. Successful nonoperative management should also emphasize effective swelling control through limb elevation, as well as the initiation of early finger exercises to prevent hand stiffness. After removal of the cast or splint, active wrist mobilization is essential for restoring optimal range of motion and achieving functional recovery.
Introduction
Literature search strategy
Clinical considerations in nonoperative treatment
Radiographic parameters for assessing anatomical displacement
Radiographic and clinical indications
Reduction of the fracture and postinjury management
Type and duration of splint or cast immobilization
Rehabilitation after immobilization
Evidence integration
Limitations of the evidence and this review
Conclusions
-
Author contributions
Conceptualization: SWC, JKK. Supervision: JKK. Writing-original draft: SWC. Writing-review & editing: SWC, JKK. All authors have read and approved the final version of the manuscript.
-
Conflicts of interest
No potential conflict of interest relevant to this article was reported.
-
Funding
None.
-
Data availability
Not applicable.
-
Acknowledgments
None.
-
Supplementary materials
None.
Article Information
| Study | Included patients | Type of treatment | No. | Age (yr) | Sex (male: female) | Severity of fracture (AO type) | Clinical outcomes at final F/U | Radiologic outcomes | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Wrist flexion/extensiona) | Grip strengtha) | Patient-reported outcomes | Dorsal angulation (°)b) | Radial inclination (°)b) | Ulnar variance (mm)b) | |||||||||||||
| Pre | Post | F/U | Pre | Post | F/U | Pre | Post | F/U | ||||||||||
| 2005, Azzopardi et al. [20] | Unstable, extraarticular fractures | Nonoperative | 27 | 71 | 2:25 | A3 | 88.5% | 72% | SF-36 physical: 38.2 | 29±16 | ‒5±7 | 4±8 | 18±6 | 21±3 | 19±6 | 3±3 | 0±1 | 3±2 |
| Percutaneous pinning | 27 | 72 | 4:23 | A3 | 90.5% | 77% | SF-36 physical: 42.2 | 35±15 | ‒4±7 | ‒3±10c) | 16±6 | 22±3 | 22±5 | 4±3 | 0±1 | 3±2 | ||
| 2010, Wong et al. [28] | Unstable, extraarticular fractures | Nonoperative | 30 | 71 | 5:25 | Frykman classification I:II (18:12) | 143° | 9.0 kg | Mayo wrist scores: 80.5±7.5 | 31±6 | ‒7.5±1 | 3±1 | 13±3 | 23±4 | 16±2 | 4.3±1.2 | 0.5±0.2 | 3.2±1.4 |
| Percutaneous pinning | 30 | 70 | 6:24 | Frykman classification I:II (17:13) | 145° | 8.5 kg | Mayo wrist scores: 82.2±6.2 | 33±6 | ‒8±1 | ‒4±1c) | 13±4 | 23±2 | 20±2c) | 5.2±1.8 | 0.3±0.1 | 2.1±1.1 | ||
| 2011, Arora et al. [26] | Displaced, unstable fractures | Nonoperative | 37 | 77.4 | 10:27 | A2-3, A3-9, C1-11, C2-8, C3-6 | 103.7%c) | 92.6% | DASH scores: 8.0±9.3 | 3.6±11.2 | 10.4±19.1 | 20.3±3.3 | 15.9±9.0 | 0.8±1.7 | 3.2±2.9 | |||
| ORIF with volar locking plate | 36 | 75.9 | 8:28 | A2-3, A3-7, C1-4, C2-12, C3-10 | 92.8% | 102.4%c) | DASH scores: 5.7±11.1 | ‒3.6±6.9c) | ‒0.5±4.7c) | 21.8±2.7c) | 21.2±2.6c) | 0.6±1.6 | 0.7±1.8c) | |||||
| 2014, Sharma et al. [27] | AO type B and C fractures | Nonoperative | 32 | 48.1 | 10:22 | B-13, C-19 | 135.0° | 72.2% | DASH scores: 14.0±10.2 | ‒8.4±0.4 | ‒5.2±0.5 | 18.1±0.9 | 15.2±0.8 | 0.2±0.1 | 0.3±0.1 | |||
| ORIF with volar locking plate | 32 | 52.4 | 9:23 | B-19, C-17 | 168.2°c) | 89.1%c) | DASH scores: 5.0±9.4c) | ‒10.1±1.5c) | ‒8.4±1.0c) | 20.5±1.3c) | 17.9±0.8c) | ‒0.3±0.3 | ‒0.3±0.2 | |||||
| 2019, Saving et al. [22] | Dorsally displaced fractures (≥20° dorsal tilt) | Nonoperative | 64 | 78 | 8:56 | A2-10, A3-28, C1-20, C2-6, C3-0 | 107° | 80.9% | PRWE scores: 22.4±21.4 DASH scores: 23.1±19.8 | 27±8 | 8±8 | 14±13 | 14±8 | 18±6 | 14±7 | 2.3±2.2 | 0.6±1.6 | 2.7±2.2 |
| Volar locking plate | 58 | 80 | 3:55 | A2-6, A3-33, C1-11, C2-7, C3-1 | 118° | 96.0%c) | PRWE scores: 12.7±15.0 DASH scores: 15.6±17.0c) | 31±10 | ‒1±7c) | 1±9c) | 14±13 | 18±8 | 19±8c) | 2.4±2.1 | 0.0±0.3c) | 0.5±1.3c) | ||
| 2021, Hassellund et al. [24] | Displaced, unstable fractures | Nonoperative | 50 | 73.9 | 8:42 | A2-2, A3-12, C1-11, C2-18, C3-7 | 112° | 77% | QuickDASH median: 5 PRWE median: 2 | 23 | 13 | 20 | 18 | 19 | 18 | 3 | 5 | 5 |
| Volar locking plate | 50 | 73.4 | 3:47 | A2-3, A3-9, C1-13, C2-16, C3-9 | 119° | 88%c) | QuickDASH median: 0 PRWE median: 0c) | 21 | ‒1c) | ‒1c) | 19 | 24c) | 25c) | 3 | 2c) | 2c) | ||
Table 1 summarizes key comparative studies. Differences in fracture classification, definitions of instability, and outcome instruments limit direct comparisons across studies. For patient-reported outcomes, statistical significance should be interpreted alongside clinical relevance (e.g., the minimal clinically important difference, when available). Follow-up intervals vary; early functional differences may not persist at later assessments. All of the continuous values are presented as mean or mean±standard deviation.
DASH, Disabilities of the Arm, Shoulder and Hand; SF-36, Short Form-36 Health Survey; QuickDASH, Quick Disabilities of the Arm, Shoulder and Hand; PRWE, Patient-Rated Wrist Evaluation.
a)Wrist flexion/extension arc and grip strength of the involved hand are presented as raw data or ratios compared with the contralateral side.
b)Pre denotes the values before the reduction or operation. Post means the values after the reduction or operation. F/U refers to values that were measured at the final follow-up period.
c)The value of this group is statistically significantly better than that of the comparison group.
- 1. Baron JA, Karagas M, Barrett J, et al. Basic epidemiology of fractures of the upper and lower limb among Americans over 65 years of age. Epidemiology 1996;7:612-8.ArticlePubMed
- 2. Orbay JL, Fernandez DL. Volar fixation for dorsally displaced fractures of the distal radius: a preliminary report. J Hand Surg Am 2002;27:205-15.ArticlePubMed
- 3. Bentohami A, de Burlet K, de Korte N, et al. Complications following volar locking plate fixation for distal radial fractures: a systematic review. J Hand Surg Eur Vol 2014;39:745-54.ArticlePubMedPDF
- 4. Kodama N, Takemura Y, Ueba H, Imai S, Matsusue Y. Acceptable parameters for alignment of distal radius fracture with conservative treatment in elderly patients. J Orthop Sci 2014;19:292-7.ArticlePubMed
- 5. Palmer AK, Werner FW. Biomechanics of the distal radioulnar joint. Clin Orthop Relat Res 1984;187:26-35.Article
- 6. Bronstein AJ, Trumble TE, Tencer AF. The effects of distal radius fracture malalignment on forearm rotation: A cadaveric study. J Hand Surg Am 1997;22:258-62.ArticlePubMed
- 7. Knirk JL, Jupiter JB. Intra-articular fractures of the distal end of the radius in young adults. J Bone Joint Surg Am 1986;68:647-59.ArticlePubMed
- 8. Kazuki K, Kusunoki M, Yamada J, Yasuda M, Shimazu A. Cineradiographic study of wrist motion after fracture of the distal radius. J Hand Surg Am 1993;18:41-6.ArticlePubMed
- 9. Miyake T, Hashizume H, Inoue H, Shi Q, Nagayama N. Malunited Colles’ fracture: analysis of stress distribution. J Hand Surg Br 1994;19:737-42.ArticlePubMed
- 10. Fernandez DL. Malunion of the distal radius: current approach to management. Instr Course Lect 1993;42:99-113.PubMed
- 11. Altissimi M, Antenucci R, Fiacca C, Mancini GB. Long-term results of conservative treatment of fractures of the distal radius. Clin Orthop Relat Res 1986;206:202-10.Article
- 12. Weber ER. A rational approach for the recognition and treatment of Colles’ fracture. Hand Clin 1987;3:13-21.ArticlePubMed
- 13. Cooney WP. Fractures of the distal radius: a modern treatment-based classification. Orthop Clin North Am 1993;24:211-6.ArticlePubMed
- 14. Lafontaine M, Hardy D, Delince P. Stability assessment of distal radius fractures. Injury 1989;20:208-10.ArticlePubMed
- 15. Lee JH. Surgical indications for distal radius fractures. J Korean Soc Surg Hand 2015;20:72-6.Article
- 16. Martinez-Mendez D, Lizaur-Utrilla A, de-Juan-Herrero J. Intra-articular distal radius fractures in elderly patients: a randomized prospective study of casting versus volar plating. J Hand Surg Eur Vol 2018;43:142-7.ArticlePubMedPDF
- 17. Park MJ, Kim JP, Lee HI, et al. Is a short arm cast appropriate for stable distal radius fractures in patients older than 55 years? A randomized prospective multicentre study. J Hand Surg Eur Vol 2017;42:487-92.ArticlePubMedPDF
- 18. Simic PM, Weiland AJ. Fractures of the distal aspect of the radius: changes in treatment over the past two decades. Instr Course Lect 2003;52:185-95.ArticlePubMed
- 19. Song SW. Osteoporotic distal radius fracture-conservative treatment. J Korean Fract Soc 2008;21:81-6.Article
- 20. Azzopardi T, Ehrendorfer S, Coulton T, Abela M. Unstable extra-articular fractures of the distal radius: a prospective, randomised study of immobilisation in a cast versus supplementary percutaneous pinning. J Bone Joint Surg Br 2005;87:837-40.ArticlePubMed
- 21. Haslhofer DJ, Froschauer SM, Gotterbarm T, Schmidt M, Kwasny O, Holzbauer M. Comparison of surgical and conservative therapy in older patients with distal radius fracture: a prospective randomized clinical trial. J Orthop Traumatol 2024;25:46.ArticlePubMedPMCPDF
- 22. Saving J, Wahlgren SS, Olsson K, et al. Nonoperative treatment compared with volar locking plate fixation for dorsally displaced distal radial fractures in the elderly: a randomized controlled trial. J Bone Joint Surg Am 2019;101:961-9.ArticlePubMed
- 23. Chung KC, Kim HM, Malay S, et al. The wrist and radius injury surgical trial: 12-month outcomes from a multicenter international randomized clinical trial. Plast Reconstr Surg 2020;145:1054e-1066e.ArticlePubMedPMC
- 24. Hassellund SS, Williksen JH, Laane MM, et al. Cast immobilization is non-inferior to volar locking plates in relation to QuickDASH after one year in patients aged 65 years and older: a randomized controlled trial of displaced distal radius fractures. Bone Joint J 2021;103-B:247-55.ArticlePubMedPDF
- 25. Gutierrez-Espinoza H, Araya-Quintanilla F, Olguin-Huerta C, et al. Effectiveness of surgical versus conservative treatment of distal radius fractures in elderly patients: a systematic review and meta-analysis. Orthop Traumatol Surg Res 2022;108:103323.ArticlePubMed
- 26. Arora R, Lutz M, Deml C, Krappinger D, Haug L, Gabl M. A prospective randomized trial comparing nonoperative treatment with volar locking plate fixation for displaced and unstable distal radial fractures in patients sixty-five years of age and older. J Bone Joint Surg Am 2011;93:2146-53.ArticlePubMed
- 27. Sharma H, Khare GN, Singh S, Ramaswamy AG, Kumaraswamy V, Singh AK. Outcomes and complications of fractures of distal radius (AO type B and C): volar plating versus nonoperative treatment. J Orthop Sci 2014;19:537-44.ArticlePubMed
- 28. Wong TC, Chiu Y, Tsang WL, Leung WY, Yam SK, Yeung SH. Casting versus percutaneous pinning for extra-articular fractures of the distal radius in an elderly Chinese population: a prospective randomised controlled trial. J Hand Surg Eur Vol 2010;35:202-8.ArticlePubMedPDF
- 29. Jaremko JL, Lambert RG, Rowe BH, Johnson JA, Majumdar SR. Do radiographic indices of distal radius fracture reduction predict outcomes in older adults receiving conservative treatment? Clin Radiol 2007;62:65-72.ArticlePubMed
- 30. Young BT, Rayan GM. Outcome following nonoperative treatment of displaced distal radius fractures in low-demand patients older than 60 years. J Hand Surg Am 2000;25:19-28.ArticlePubMed
- 31. Kyung MG, Chung HW, Kim JS, et al. Closed reduction and cast immobilization for the treatment of distal radius fracture: does dorsal metaphyseal comminution predict radiographic and functional outcomes? J Korean Soc Surg Hand 2013;18:29-36.Article
- 32. Kim JM, Seo HJ, Jeon YD, Lee HM, Son JH. Comparative study of outcomes between operative and non-operative treatment of unstable distal radius fracture in the elderly patients. J Korean Soc Surg Hand 2015;20:43-50.Article
- 33. The Korean Society for Surgery of the Hand. Surgery of the hand. Panmuneducation; 2014.
- 34. Lee JH, Hong SH, Kim YJ, Back JH, Lee JS. Effect of different splints on displacement after closed reduction of the distal radius fractures: a comparison of short arm double splint and sugar-tong splint. J Korean Soc Surg Hand 2015;20:104-9.Article
- 35. Cho JH, Park DY, Kim JY, Han KJ. A comparison of sugar tong splint and radial gutter short arm splint after closed reduction of distal radius fracture. Arch Hand Microsurg 2009;14:194-8.
- 36. Frykman G. Fracture of the distal radius including sequelae—shoulder-hand-finger syndrome, disturbance in the distal radio-ulnar joint and impairment of nerve function: a clinical and experimental study. Acta Orthop Scand 1967;Suppl 108:3.ArticlePubMed
- 37. Bong MR, Egol KA, Leibman M, Koval KJ. A comparison of immediate postreduction splinting constructs for controlling initial displacement of fractures of the distal radius: a prospective randomized study of long-arm versus short-arm splinting. J Hand Surg Am 2006;31:766-70.ArticlePubMed
- 38. Grafstein E, Stenstrom R, Christenson J, et al. A prospective randomized controlled trial comparing circumferential casting and splinting in displaced Colles fractures. CJEM 2010;12:192-200.ArticlePubMed
- 39. Lichtman DM, Bindra RR, Boyer MI, et al. American Academy of Orthopaedic Surgeons clinical practice guideline on: The treatment of distal radius fractures. J Bone Joint Surg Am 2011;93:775-8.ArticlePubMed
- 40. Guebeli A, Thieringer F, Honigmann P, Keller M. In-house 3D-printed custom splints for non-operative treatment of distal radial fractures: a randomized controlled trial. J Hand Surg Eur Vol 2024;49:350-8.ArticlePubMedPDF
- 41. McAuliffe TB, Hilliar KM, Coates CJ, Grange WJ. Early mobilisation of Colles’ fractures. A prospective trial. J Bone Joint Surg Br 1987;69:727-9.ArticlePubMedPDF
- 42. de Bruijn MA, van Ginkel LA, Boersma EZ, et al. The past, present and future of the conservative treatment of distal radius fractures. Injury 2023;54 Suppl 5:110930.ArticlePubMed
- 43. Bucholz R, Rockwood C, Green D. Rockwood and Green’s fractures in adults. 7th ed. Philadelphia, PA: Wolters Kluwer Health/Lippincott Williams & Wilkins; 2010.
- 44. Jung M, Sung S, Choi I. Textbook of fractures. 3rd ed. Gunja; 2008.
References
Figure & Data
REFERENCES
Citations

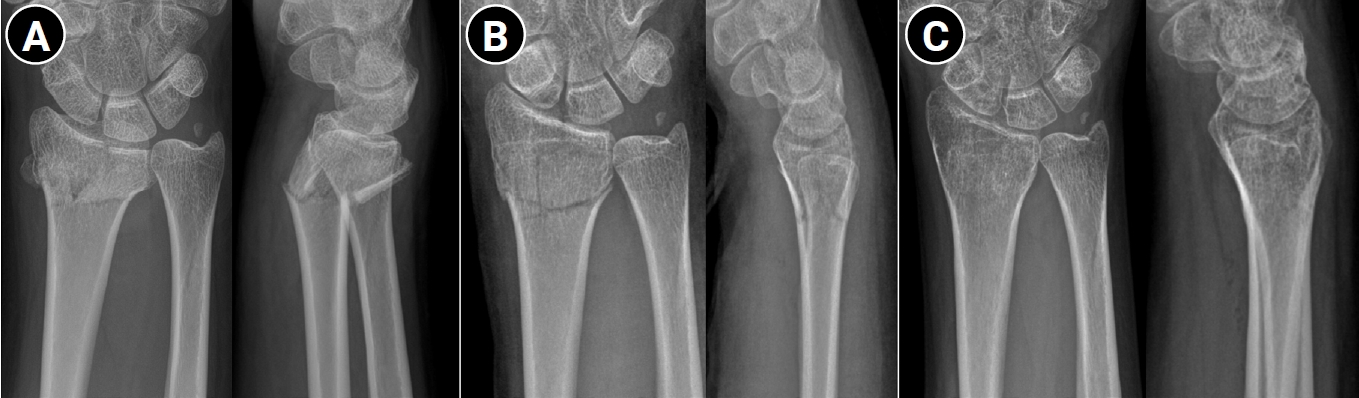
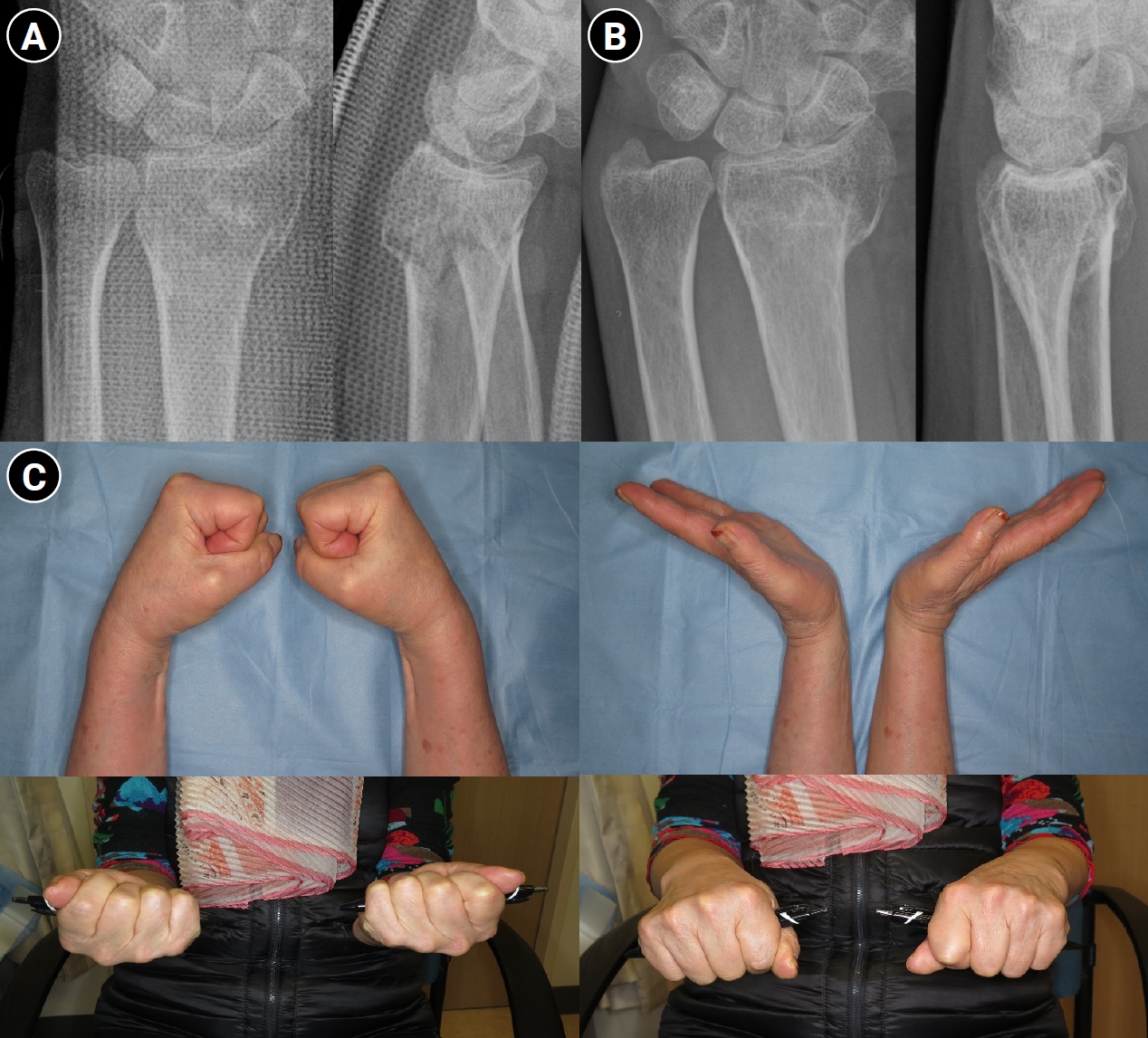
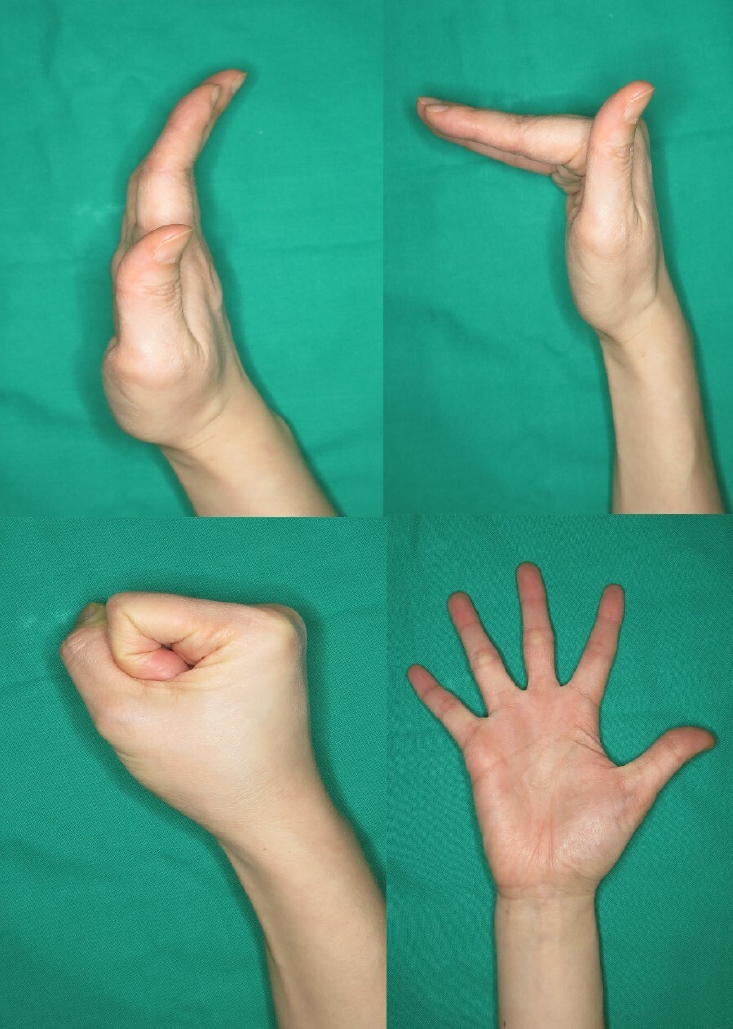
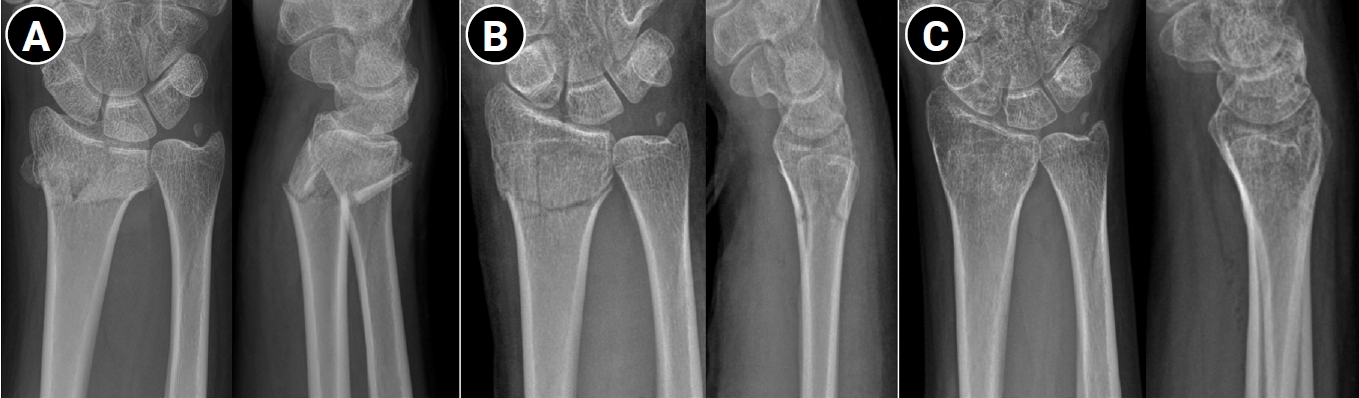
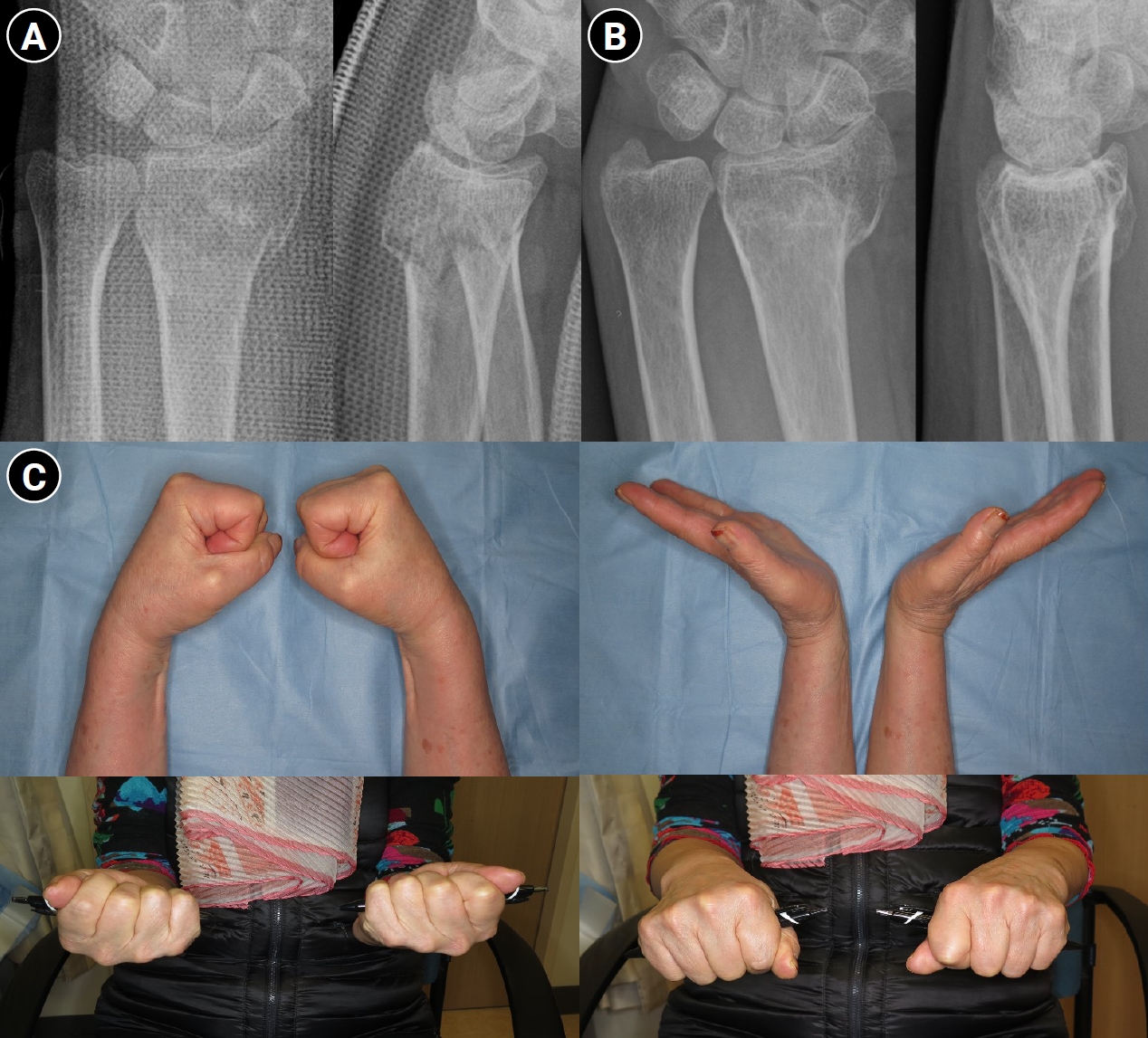
Fig. 1.
Fig. 2.
Fig. 3.
| Study | Included patients | Type of treatment | No. | Age (yr) | Sex (male: female) | Severity of fracture (AO type) | Clinical outcomes at final F/U | Radiologic outcomes | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Wrist flexion/extension |
Grip strength |
Patient-reported outcomes | Dorsal angulation (°) |
Radial inclination (°) |
Ulnar variance (mm) |
|||||||||||||
| Pre | Post | F/U | Pre | Post | F/U | Pre | Post | F/U | ||||||||||
| 2005, Azzopardi et al. [20] | Unstable, extraarticular fractures | Nonoperative | 27 | 71 | 2:25 | A3 | 88.5% | 72% | SF-36 physical: 38.2 | 29±16 | ‒5±7 | 4±8 | 18±6 | 21±3 | 19±6 | 3±3 | 0±1 | 3±2 |
| Percutaneous pinning | 27 | 72 | 4:23 | A3 | 90.5% | 77% | SF-36 physical: 42.2 | 35±15 | ‒4±7 | ‒3±10 |
16±6 | 22±3 | 22±5 | 4±3 | 0±1 | 3±2 | ||
| 2010, Wong et al. [28] | Unstable, extraarticular fractures | Nonoperative | 30 | 71 | 5:25 | Frykman classification I:II (18:12) | 143° | 9.0 kg | Mayo wrist scores: 80.5±7.5 | 31±6 | ‒7.5±1 | 3±1 | 13±3 | 23±4 | 16±2 | 4.3±1.2 | 0.5±0.2 | 3.2±1.4 |
| Percutaneous pinning | 30 | 70 | 6:24 | Frykman classification I:II (17:13) | 145° | 8.5 kg | Mayo wrist scores: 82.2±6.2 | 33±6 | ‒8±1 | ‒4±1 |
13±4 | 23±2 | 20±2 |
5.2±1.8 | 0.3±0.1 | 2.1±1.1 | ||
| 2011, Arora et al. [26] | Displaced, unstable fractures | Nonoperative | 37 | 77.4 | 10:27 | A2-3, A3-9, C1-11, C2-8, C3-6 | 103.7% |
92.6% | DASH scores: 8.0±9.3 | 3.6±11.2 | 10.4±19.1 | 20.3±3.3 | 15.9±9.0 | 0.8±1.7 | 3.2±2.9 | |||
| ORIF with volar locking plate | 36 | 75.9 | 8:28 | A2-3, A3-7, C1-4, C2-12, C3-10 | 92.8% | 102.4% |
DASH scores: 5.7±11.1 | ‒3.6±6.9 |
‒0.5±4.7 |
21.8±2.7 |
21.2±2.6 |
0.6±1.6 | 0.7±1.8 |
|||||
| 2014, Sharma et al. [27] | AO type B and C fractures | Nonoperative | 32 | 48.1 | 10:22 | B-13, C-19 | 135.0° | 72.2% | DASH scores: 14.0±10.2 | ‒8.4±0.4 | ‒5.2±0.5 | 18.1±0.9 | 15.2±0.8 | 0.2±0.1 | 0.3±0.1 | |||
| ORIF with volar locking plate | 32 | 52.4 | 9:23 | B-19, C-17 | 168.2° |
89.1% |
DASH scores: 5.0±9.4 |
‒10.1±1.5 |
‒8.4±1.0 |
20.5±1.3 |
17.9±0.8 |
‒0.3±0.3 | ‒0.3±0.2 | |||||
| 2019, Saving et al. [22] | Dorsally displaced fractures (≥20° dorsal tilt) | Nonoperative | 64 | 78 | 8:56 | A2-10, A3-28, C1-20, C2-6, C3-0 | 107° | 80.9% | PRWE scores: 22.4±21.4 DASH scores: 23.1±19.8 | 27±8 | 8±8 | 14±13 | 14±8 | 18±6 | 14±7 | 2.3±2.2 | 0.6±1.6 | 2.7±2.2 |
| Volar locking plate | 58 | 80 | 3:55 | A2-6, A3-33, C1-11, C2-7, C3-1 | 118° | 96.0% |
PRWE scores: 12.7±15.0 DASH scores: 15.6±17.0 |
31±10 | ‒1±7 |
1±9 |
14±13 | 18±8 | 19±8 |
2.4±2.1 | 0.0±0.3 |
0.5±1.3 |
||
| 2021, Hassellund et al. [24] | Displaced, unstable fractures | Nonoperative | 50 | 73.9 | 8:42 | A2-2, A3-12, C1-11, C2-18, C3-7 | 112° | 77% | QuickDASH median: 5 PRWE median: 2 | 23 | 13 | 20 | 18 | 19 | 18 | 3 | 5 | 5 |
| Volar locking plate | 50 | 73.4 | 3:47 | A2-3, A3-9, C1-13, C2-16, C3-9 | 119° | 88% |
QuickDASH median: 0 PRWE median: 0 |
21 | ‒1 |
‒1 |
19 | 24 |
25 |
3 | 2 |
2 |
||
Table 1 summarizes key comparative studies. Differences in fracture classification, definitions of instability, and outcome instruments limit direct comparisons across studies. For patient-reported outcomes, statistical significance should be interpreted alongside clinical relevance (e.g., the minimal clinically important difference, when available). Follow-up intervals vary; early functional differences may not persist at later assessments. All of the continuous values are presented as mean or mean±standard deviation. DASH, Disabilities of the Arm, Shoulder and Hand; SF-36, Short Form-36 Health Survey; QuickDASH, Quick Disabilities of the Arm, Shoulder and Hand; PRWE, Patient-Rated Wrist Evaluation. Wrist flexion/extension arc and grip strength of the involved hand are presented as raw data or ratios compared with the contralateral side. Pre denotes the values before the reduction or operation. Post means the values after the reduction or operation. F/U refers to values that were measured at the final follow-up period. The value of this group is statistically significantly better than that of the comparison group.

 E-submission
E-submission KOTA
KOTA TOTA
TOTA TOTS
TOTS
 ePub Link
ePub Link Cite
Cite

