Abstract
-
Background
Mayo type IIIB olecranon fractures are characterized by significant displacement and comminution, presenting a challenge in selecting the appropriate fixation technique. This study compared the clinical and radiographic outcomes, complications, and reoperation rates of reinforced tension band wiring (TBW) and precontoured plate and screw fixation (PF) in the surgical treatment of Mayo type IIIB olecranon fractures.
-
Methods
This retrospective review analyzed 24 patients diagnosed with Mayo type IIIB olecranon fractures, who were treated between 2005 and 2023. Of these, 11 patients underwent reinforced TBW, and 13 received precontoured PF. Clinical outcomes were assessed using Disabilities of the Arm, Shoulder, and Hand (DASH) scores and the Mayo Elbow Performance Score (MEPS). Radiographic outcomes focused on fracture union. Operative times, complication rates, and reoperation rates were compared between the groups.
-
Results
Both the reinforced TBW and PF groups achieved satisfactory clinical outcomes, with no significant between-group differences in DASH and MEPS scores (P>0.05). Radiographic union was achieved in all patients. The reinforced TBW group demonstrated a significantly shorter operative time than the PF group (93.6±7.4 minutes vs. 132.3±13.7 minutes; P<0.001). Complication rates were similar between the two groups (reinforced TBW, 38.4%; PF, 36.3%), but hardware-related irritation occurred more frequently in the reinforced TBW group. Reoperations were required in 15.8% of the reinforced TBW group due to hardware irritation, whereas no reoperations were necessary in the PF group.
-
Conclusions
Reinforced TBW and PF are both effective surgical options for managing Mayo type IIIB olecranon fractures, yielding comparable clinical and radiographic outcomes. While reinforced TBW offers shorter operative times and lower costs, PF is associated with fewer hardware-related complications. Further prospective studies are needed to optimize treatment strategies for these complex fractures.
-
Level of evidence
III.
-
Keywords: Elbow, Olecranon fracture, Internal fracture fixation, Bone plates, Treatment outcome
Introduction
All olecranon fractures are intraarticular fractures and represent approximately 10% of all upper extremity fractures [
1]. Considering that displacement and comminution of fracture affect treatment outcomes, the proper management of Mayo type III fractures is important [
2-
4]. The outcomes of treating Mayo type III olecranon fractures are affected by anatomic restoration of the articular surface, secure repair of the elbow extensor mechanism, restoration of joint stability and motion, and prevention of stiffness through firm fixation and early rehabilitation and other complications [
3,
4]. Various surgical techniques, including tension band wiring (TBW), plate and screw fixation (PF), intramedullary fixation, and suture techniques, have been used to gain firm fixation [
5-
7]. TBW is commonly used for simple fractures, while PF is the first-line modality for complex and comminuted fractures; however, reinforced TBW, modified technique, can be applied to these fractures. Mayo type IIIB olecranon fractures present a challenge in selecting the appropriate fixation technique. In this study, we compared patients treated with reinforced TBW with those treated with PF technique, both of which are associated with complications, including hardware irritation, wound dehiscence, infection, and stiffness [
3]. We compared the clinical and radiographic outcomes, surgical complications, and reoperation rates of reinforced TBW and PF for the treatment of Mayo type IIIB olecranon fractures.
Methods
Ethics Statement
The study was approved by the Institutional Review Board (IRB) of Inha University Hospital (IRB No. 2024-09-006) and performed in accordance with the principles of the Declaration of Helsinki. The need for written informed consent was waived because of its retrospective design by the IRB.
Study Design and Participant Selection
This study was conducted at a single center between January 2005 and June 2023, using radiographic images and electronic medical records as the main data sources. The inclusion criteria for this study were patients aged ≥18 years with isolated olecranon fracture type IIIB according to the Mayo classification and who underwent surgical treatment with either reinforced TBW fixation or PF. The exclusion criteria were as follows: non-cooperative patients, patients with open fractures, and patients with previous injuries or associated concomitant lesions of the ipsilateral upper limb. Twenty-four patients met the inclusion criteria. There were 13 men and 11 women, with an average age of 60 years (range, 47–90 years). Eleven patients (45.8%) had injured their dominant arm. All patients of both groups were provided full range of motion (ROM) with an assisted long-arm brace (Seoul Prosthesis Corp.) over the course of 4 weeks after 1 week of immobilization in a splint.
The demographic characteristics of the reinforced TBW and PF groups are presented in
Table 1. Electronic medical records were evaluated to review data on clinical outcomes (ROM measured using a goniometer and via neurological examination at postoperative day 12 moths), surgical complications, and reoperations. Computed tomography image and radiographic images, including anteroposterior and lateral views, were reviewed to assess fracture classification while only radiographic images were reviewed for evaluating loss of reduction and union at postoperative day 1, 2 months, 3 months, and 12 months. The Disabilities of the Arm, Shoulder, and Hand (DASH) questionnaire and the Mayo Elbow Performance Score (MEPS) were used to determine the functional outcome. The availability of these data was considered after a minimum follow-up period of 12 months.
Surgery was performed by a single doctor (TJL) who decided on the procedure according to his preference. Reinforced TBW was performed under general or regional anesthesia, with the patient positioned laterally for optimal surgical access to the olecranon. A longitudinal incision was made using the posterior approach to expose the fracture site, providing direct access to both the proximal ulna and radial head. Anatomical reduction of articular fragments was meticulously achieved under direct visualization, restoring the original contour of the olecranon, which is an essential step for the success of tension band construction, as the anterior cortex must serve as a solid buttress and cortex continuity for effective compression. In cases requiring additional stability, adjunctive fixation methods, including screws, K-wires, cerclage wires, and triceps Krackow suture techniques, were used. Considering the pattern and position of bone fragments, screws, K-wires, and cerclage wires were used for relatively distal fragments, while triceps Krackow suture techniques were used for proximal fragments, where the application of the former methods was challenging (
Figs. 1 and
2). The stability of the construct was confirmed intraoperatively through full ROM testing of the elbow, and postoperative radiographs were obtained to verify the correct implant placement and successful restoration of anatomical alignment. PF was performed using a dorsal precontoured plate with a combination of locking and cortical screws.
Statistical analysis was conducted to assess the relative efficacy of the two groups with regard to clinical and radiographic outcomes, surgical complications, and reoperations. Fisher exact test and the Mann-Whitney U-test were used to assess differences between the two groups. Statistical significance was set at P<0.05. All analyses were performed using the IBM SPSS version 25.0 (IBM Corp.).
Results
Clinical Results
Functional outcomes, as measured using the DASH scores and MEPS, were not significantly different between the two groups. The mean DASH scores was 11.0 (range, 0–22.4) in the reinforced TBW group and 13.1 (range, 0–26.7) in the PF group (P=0.531). Similarly, the mean MEPS was 96.1 (range, 70–100) in the reinforced TBW group and 94.1 (range, 65–100) in the PF group (P=0.865).
The average elbow flexion was 142° (range, 120°–150°) in the reinforced TBW group and 140° (range, 100°–150°) in the PF group (P=0.953). The median elbow extension deficit was 7.2° (range, 0°–30°) in the reinforced TBW group and 5.5° (range, 0°–20°) in the PF group (P=0.820). Both groups demonstrated similar outcomes in terms of supination and pronation, with no significant differences. The clinical results were obtained at the final follow-up period.
Table 2 presents the results for both the groups.
The PF group had a significantly longer operative time (with an average of 132.3±13.7 minutes) than the reinforced TBW group (with an average of 93.6±7.4 minutes; P<0.001).
Complication and Reoperation Rates
Table 3 shows the complication and reoperation rates in both the groups. Complications were noted in both the reinforced TBW and PF groups. Specifically, complications were observed in five of 13 patients (38.4%) in the reinforced TBW group and in four of 11 patients (36.3%) in the PF group. The most frequent complication in the reinforced TBW group was hardware irritation, affecting three patients (23%), compared with one patient (9.1%) in the PF group. Wound dehiscence was observed in one patient from each group (7.7% in the reinforced TBW group and 9.1% in the PF group). Similarly, stiffness (<90° elbow flexion arc) was reported in both groups (7.7% and 9.1% in the reinforced TBW and PF groups, respectively). Infection was reported in one patient (9.1%) in the PF group, with no cases in the reinforced TBW group. Importantly, there were no cases of implant failure or ulnar neuropathy in either patient group. Reoperation, excluding hardware removal, was necessary for one patient (7.7%) in the reinforced TBW group because of hardware irritation, whereas no reoperation was required in the PF group. After surgery, the problem resolved, and no further surgeries were required. Hardware removal was necessary for five patients (38.4%) in the reinforced TBW group and for four patients (36.3%) in the PF group.
Radiographic Outcomes
At day 1 radiographic anatomical reduction was achieved in all cases. Fracture healing was achieved in all patients, regardless of the procedure, and between 6 and 12 weeks postoperatively, without loss of reduction. No gap formation or secondary loss of reduction was observed on the final follow-up radiography.
Discussion
This study compared the clinical outcomes of reinforced TBW and PF in the surgical treatment of Mayo type IIIB olecranon fractures. Both techniques demonstrated similar functional results, complication rates, and reoperation rates, suggesting that both may be viable surgical options for Mayo IIIB fracture type. PF is widely recommended as the standard treatment for Mayo IIIB fractures. However, reinforced TBW may offer advantages observed when TBW is applied to other fracture types, potentially extending its applicability to Mayo IIIB fractures. To apply reinforced TBW effectively, anterior cortical continuity should be preserved to provide a solid buttress, and posterior cortex should be at least partially maintained with minimal intraarticular comminution to ensure stable fixation. Therefore, assessment of the pattern and position of bone fragments is essential, and appropriately use adjunctive fixation methods to determine applicability of reinforced TBW and maximize stability.
Schliemann et al. [
8] found no significant differences in the DASH scores and MEPS or in the overall ROM of the elbow between the TBW and PF groups with Mayo type IIA fractures. Similarly, our study also showed no significant differences in the DASH scores and MEPS between the two groups, indicating comparable functional recovery, regardless of the fixation method. The differences in the average elbow ROM and extension deficits were also similar. Although our study compares with a relatively less severe fracture pattern, it was conducted to supplement the lack of direct comparative studies on TBW and PF in Mayo IIIB fractures and to explore the potential expansion of reinforced TBW as a viable treatment option for these fractures.
Gathen et al. [
9] reported high complication rates in both the TBW (40%) and PF (25%) groups after Mayo type II-III fractures; however, these complications did not adversely affect excellent functional outcomes. In our study, the PF group showed a complication rate of 36.3%, whereas the reinforced TBW group had a similar complication rate of 38.4%. The most common complication in the reinforced TBW group was hardware irritation, affecting 23% of patients, whereas the PF group had a low rate of hardware irritation. Reoperation was required in the reinforced TBW group because of hardware-related complications, which aligns with previously reported rates of hardware removal following reinforced TBW [
10]. Conversely, no reoperation was necessary in the PF group.
Jia et al. [
11] conducted a meta-analysis of TBW and PF after Mayo type II fractures and reported that TBW had significantly shorter operative times and resulted in less blood loss than PF. This finding aligns with our results, which demonstrated that the operative time for PF was significantly longer than that for reinforced TBW (132.3±13.7 minutes vs. 93.6±7.4 minutes; P<0.001), although we did not assess blood loss.
Economically, TBW is generally considered advantageous owing to its low initial material costs. However, some studies have suggested that when reoperation rates and associated costs are considered, the financial benefit of TBW may diminish [
12]. While some studies have proposed that the total costs of TBW may be comparable to or exceed those of PF, other studies, such as those by Steadman et al. [
13] and Amini et al. [
14], have reported that the cost of TBW is approximately 40% of that of PF for Mayo type IIA fractures. Even in a hypothetical scenario where all TBW cases require reoperation, and PF cases do not require reoperation, the cost of PF remains high. Although our study involved a different fracture type and a cost analysis was not performed, we emphasize that reinforced TBW should be considered a viable alternative to plating, considering the economic costs reported by other researchers.
Our study has limitations, including its retrospective design, a long patient enrollment period, and variations and potential for bias in the selection of surgical techniques used for reinforced TBW. The patient enrollment period spanned approximately 18 years. Owing to the inclusion of surgeries performed by a single surgeon at one institution, only 24 patients were included, resulting in an imbalance between the groups. Nevertheless, despite including only 24 patients, we achieved sufficient statistical power to assess significant differences in the clinical and radiographic outcomes between the two groups. Another limitation is that we did not account for variations introduced by additional surgical techniques used for reinforced TBW, such as screws, K-wires, cerclage wires, or triceps Krackow suture techniques, which were used at the surgeon’s decision based on the degree of displacement or comminution, making statistical analyses difficult.
Conclusions
Surgical treatment with either reinforced TBW or PF achieved similar outcomes for Mayo type IIIB olecranon fractures. PF remains the first-line modality for Mayo type IIIB olecranon fractures; however, reinforced TBW can be considered as a viable option. To confirm these results, additional large-scale, prospective randomized controlled studies with long follow-up periods are necessary.
Article Information
-
Author contribution
Conceptualization: HGK, TJL, SJW. Data curation: HGK. Formal analysis: HGK, TJL, SJW. Investigation: HGK. Methodology: TJL. Project administration: TJL. Supervision: TJL, SJW. Validation: HGK, SJW. Visualization: HGK. Writing-original draft: HGK. Writing-review & editing: HGK, TJL, SJW. All authors read and approved the final manuscript.
-
Conflict of interest
None.
-
Funding
None.
-
Data availability
Contact the corresponding author for data availability.
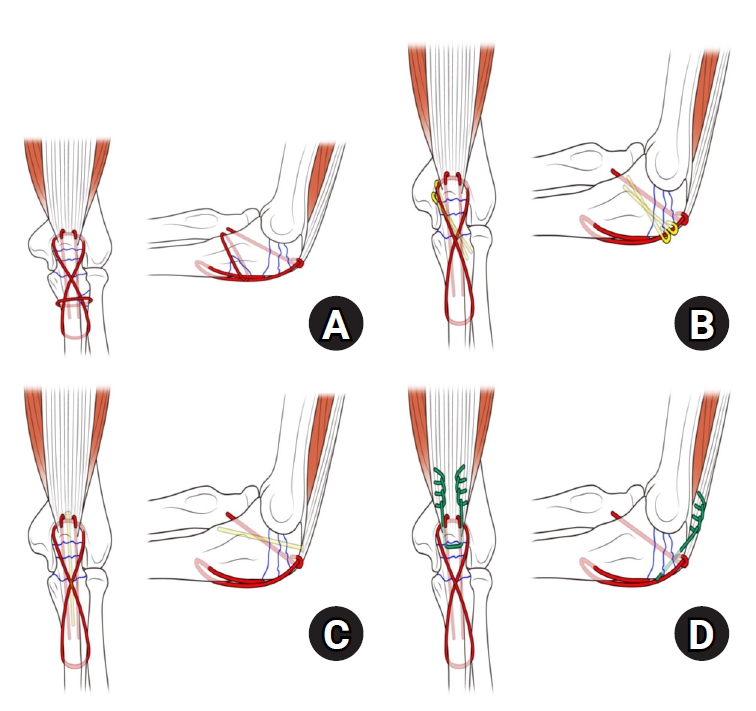
Fig. 1.(A) Reinforced tension band wiring (TBW): cerclage wire. (B) Reinforced TBW: K-wire. (C) Reinforced TBW: screw. (D) Reinforced TBW: Krackow suture through the triceps.
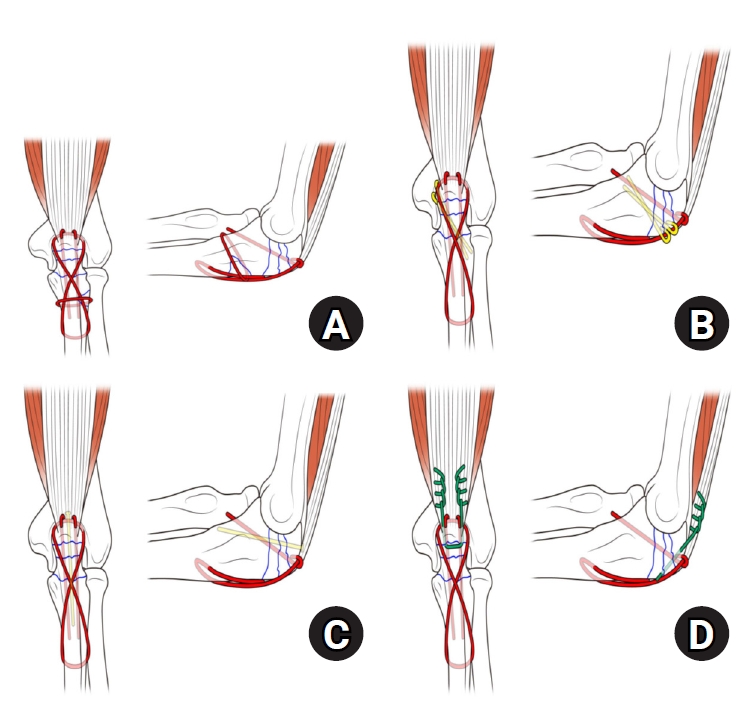
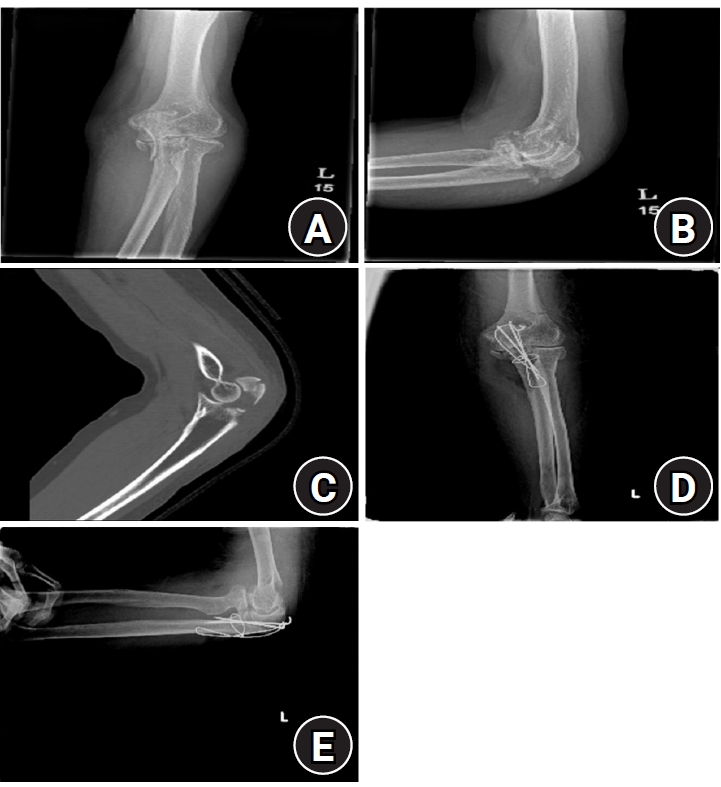
Fig. 2.A patient was treated with reinforced tension band wiring (TBW) using cerclage. (A) Radiograph in anteroposterior view before surgery. (B) Radiograph in lateral view before surgery. (C) Computed tomography image in sagittal view before surgery. (D) Radiograph in anteroposterior view after reinforced TBW surgery. (E) Radiograph in lateral view after reinforced TBW surgery.
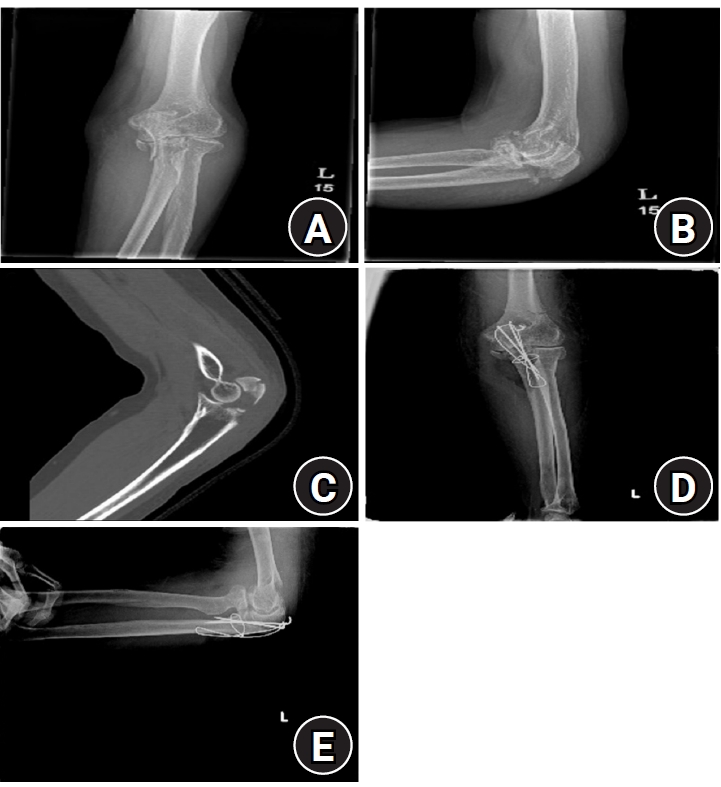
Table 1.Demographic characteristics
|
Characteristic |
Reinforced tension band wiring |
Plate and screw fixation |
|
Number |
13 |
11 |
|
Age at trauma (yr) |
58.5±8.5 |
60.3±11.1 |
|
Female sex |
6 (46.2) |
5 (45.6) |
|
Dominant arm |
6 (46.2) |
5 (45.6) |
|
Follow-up (mo) |
38.8±13.8 |
28.5±7.8 |
Table 2.
|
Variable |
Reinforced TBW |
Plate and screw fixation |
P-value |
|
Flexion (°) |
142 (120–150) |
140 (100–150) |
0.953 |
|
Extension deficit (°) |
7.2 (0–30) |
5.5 (0–20) |
0.820 |
|
Supination (°) |
80 (50–85) |
80 (65–85) |
0.608 |
|
Pronation (°) |
81 (60–85) |
80 (70–85) |
0.569 |
|
MEPS |
96.1 (70–100) |
94.1 (65–100) |
0.865 |
|
DASH score |
11.0 (0–22.4) |
13.1 (0–26.7) |
0.531 |
|
Operative time (min) |
93.6±7.4 |
132.3±13.7 |
<0.001 |
Table 3.Complication and reoperation rates
|
Complication |
Reinforced TBW (%) |
Plate and screw fixation (%) |
P-value |
|
Overall |
5 (38.4) |
4 (36.3) |
0.999 |
|
Hardware irritation |
3 (23) |
1 (9.1) |
0.596 |
|
Wound dehiscence |
1 (7.7) |
1 (9.1) |
0.999 |
|
Infection |
0 |
1 (9.1) |
0.458 |
|
Stiffness |
1 (7.7) |
1 (9.1) |
0.999 |
|
Implant failure |
0 |
0 |
- |
|
Ulnar neuropathy |
0 |
0 |
- |
|
Reoperation |
1 (7.7) |
0 |
0.999 |
|
Hardware removal |
5 (38.4) |
4 (36.3) |
0.999 |
References
- 1. Duckworth AD, Clement ND, Aitken SA, Court-Brown CM, McQueen MM. The epidemiology of fractures of the proximal ulna. Injury 2012;43:343-6.ArticlePubMed
- 2. Rommens PM, Küchle R, Schneider RU, Reuter M. Factors influencing outcome. Injury 2004;35:1149-57.ArticlePubMed
- 3. Wiegand L, Bernstein J, Ahn J. Olecranon fractures. Clin Orthop Relat Res 2012;470:3637-41.PubMedPMC
- 4. Sullivan CW, Desai K. Mayo classification of olecranon fractures. Clin Orthop Relat Res 2019;477:908-10.ArticlePubMed
- 5. Siebenlist S, Buchholz A, Braun KF. Current concepts in surgical management. EFORT Open Rev 2019;4:1-9.PubMedPMC
- 6. Oitment C, Koziarz A, Bozzo A, Johal H. Intramedullary cancellous screw fixation of simple olecranon fractures. Strategies Trauma Limb Reconstr 2019;14:163-7.ArticlePubMedPMC
- 7. Das AK, Jariwala A, Watts AC. Suture repair of simple transverse olecranon fractures and chevron olecranon osteotomy. Tech Hand Up Extrem Surg 2016;20:1-5.ArticlePubMed
- 8. Schliemann B, Raschke MJ, Groene P, et al. Comparison of tension band wiring and precontoured locking compression plate fixation in Mayo type IIA olecranon fractures. Acta Orthop Belg 2014;80:106-11.PubMed
- 9. Gathen M, Jaenisch M, Peez C, et al. Plate fixation and tension band wiring after isolated olecranon fracture comparison of outcome and complications. J Orthop 2019;18:69-75.ArticlePubMedPMC
- 10. Ren YM, Qiao HY, Wei ZJ, et al. Efficacy and safety of tension band wiring versus plate fixation in olecranon fractures: a systematic review and meta-analysis. J Orthop Surg Res 2016;11:137.ArticlePubMedPMCPDF
- 11. Jia Y, Liu A, Guo T, Chen J, Yu W, Zhai J. Efficacy and safety of tension band wire versus plate for Mayo II olecranon fractures: a systematic review and meta-analysis. J Orthop Surg Res 2022;17:373.ArticlePubMedPMCPDF
- 12. Powell AJ, Farhan-Alanie OM, McGraw IW. Tension band wiring versus locking plate fixation for simple, two-part Mayo 2A olecranon fractures: a comparison of post-operative outcomes, complications, reoperations and economics. Musculoskelet Surg 2019;103:155-60.ArticlePubMedPDF
- 13. Steadman JN, Stephens AR, Zhang C, Presson AP, Kazmers NH. Cost assessment of plating versus tension band wiring constructs for treating Mayo type 2A olecranon fractures. J Hand Surg Am 2022;47:311-9.ArticlePubMedPMC
- 14. Amini MH, Azar FM, Wilson BR, Smith RA, Mauck BM, Throckmorton TW. Comparison of outcomes and costs of tension-band and locking-plate osteosynthesis in transverse olecranon fractures: a matched-cohort study. Am J Orthop (Belle Mead NJ) 2015;44:E211-5.PubMed
 , Tong Joo Lee, MD
, Tong Joo Lee, MD , Samuel Jaeyoon Won, MD
, Samuel Jaeyoon Won, MD




 E-submission
E-submission KOTA
KOTA TOTA
TOTA TOTS
TOTS
 ePub Link
ePub Link Cite
Cite

